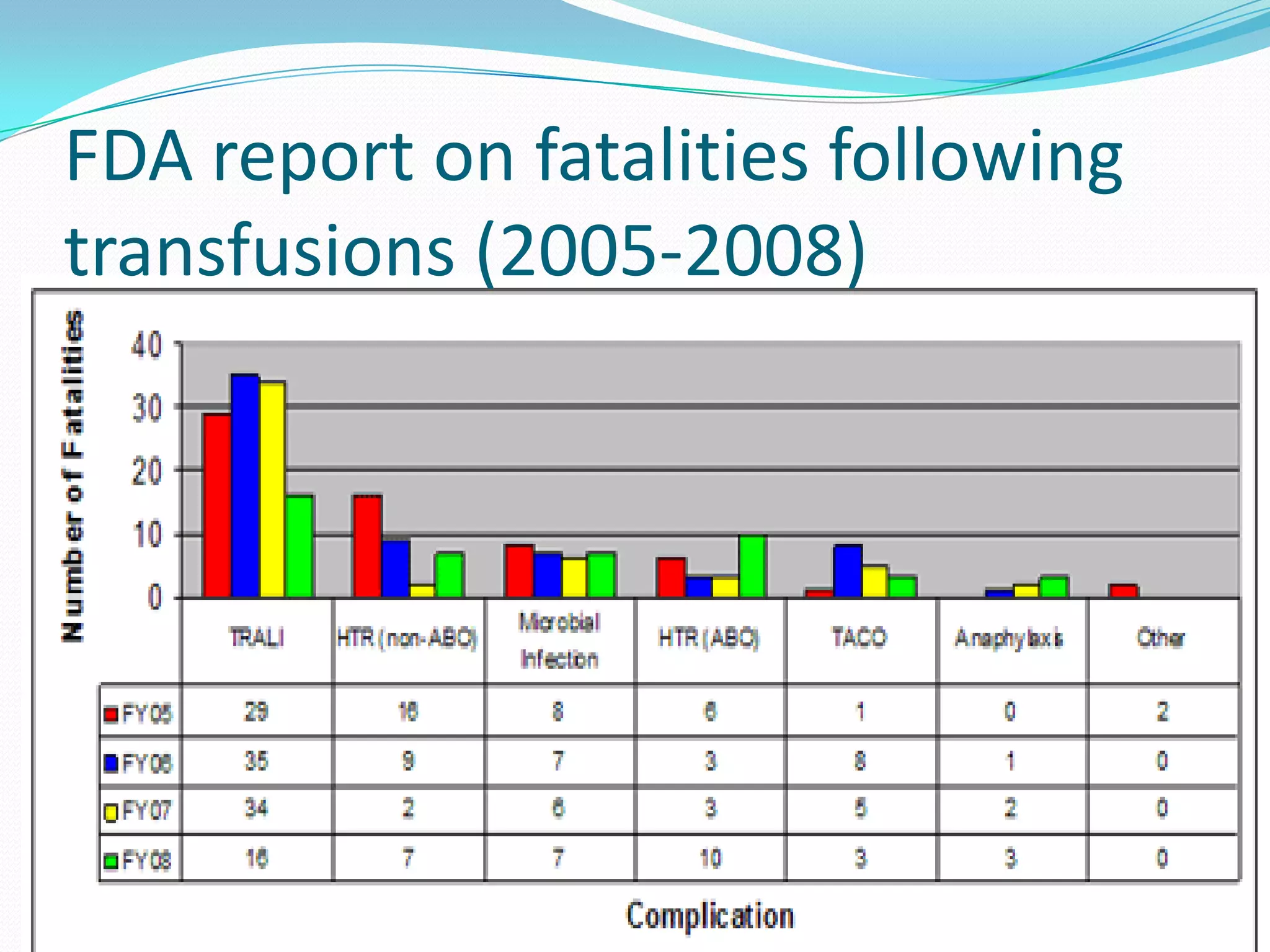
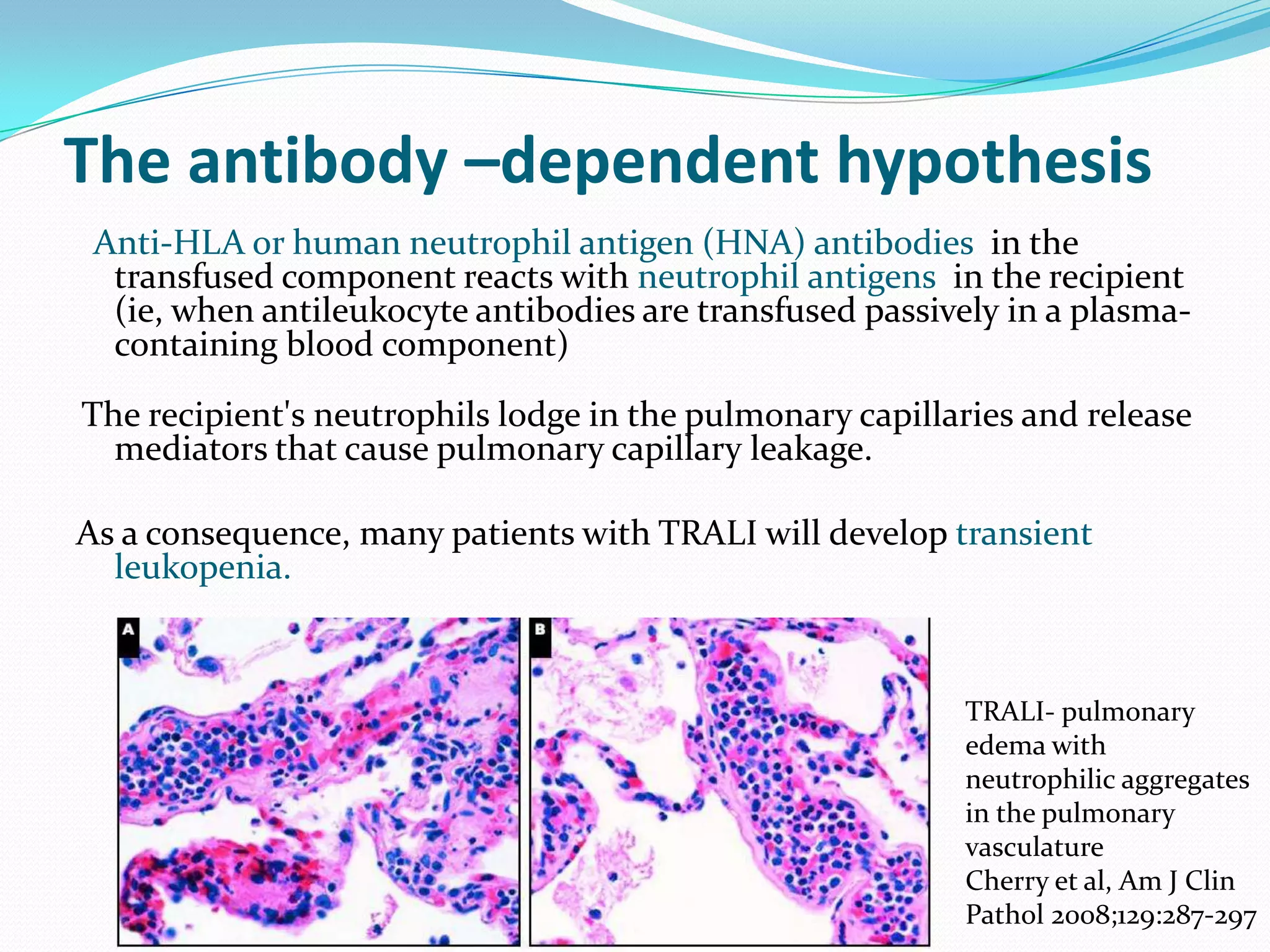
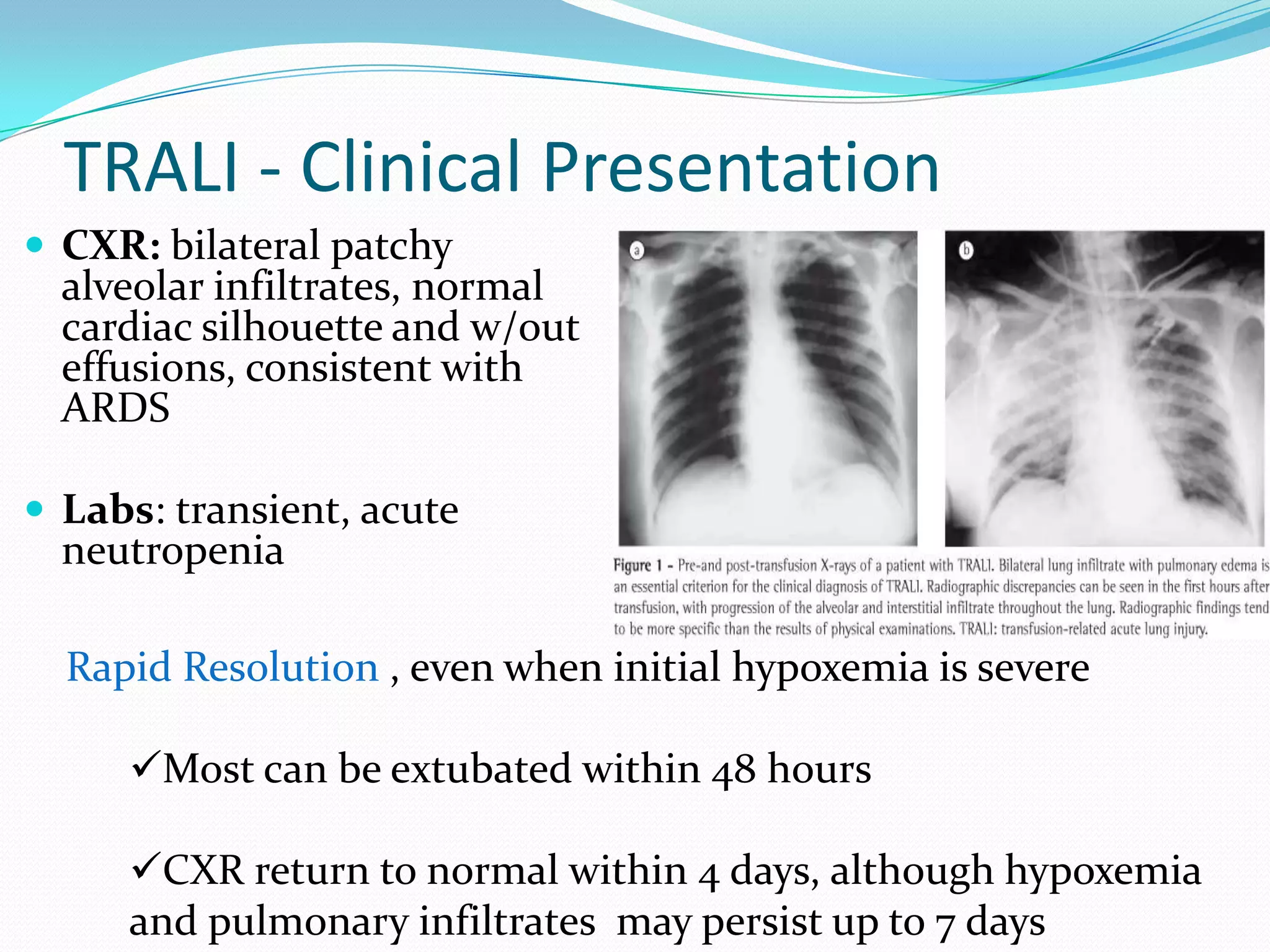
Blood transfusion involves transferring blood or blood components from a donor to a recipient. There are several types of blood transfusions including whole blood transfusion and transfusion of individual blood components like red blood cells, platelets, and plasma. Blood transfusions can cause various complications such as transfusion-related acute lung injury (TRALI), febrile nonhemolytic reactions, allergic reactions, hemolytic reactions if there is an ABO incompatibility, infections transmitted through the blood, and transfusion-associated circulatory overload (TACO). It is important to carefully screen and type donor blood and properly match it to the recipient to reduce risks of complications from blood transfusions.