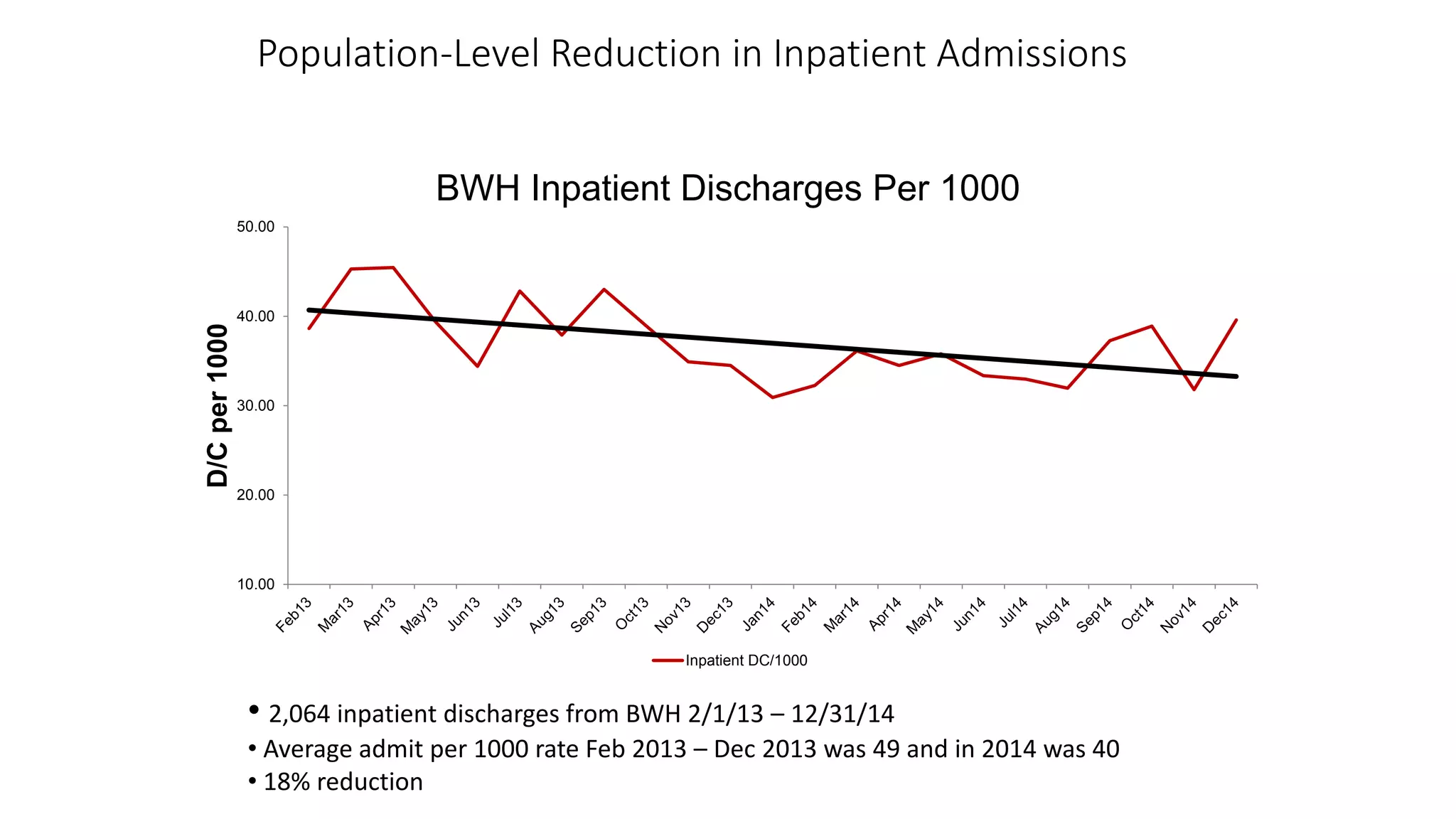
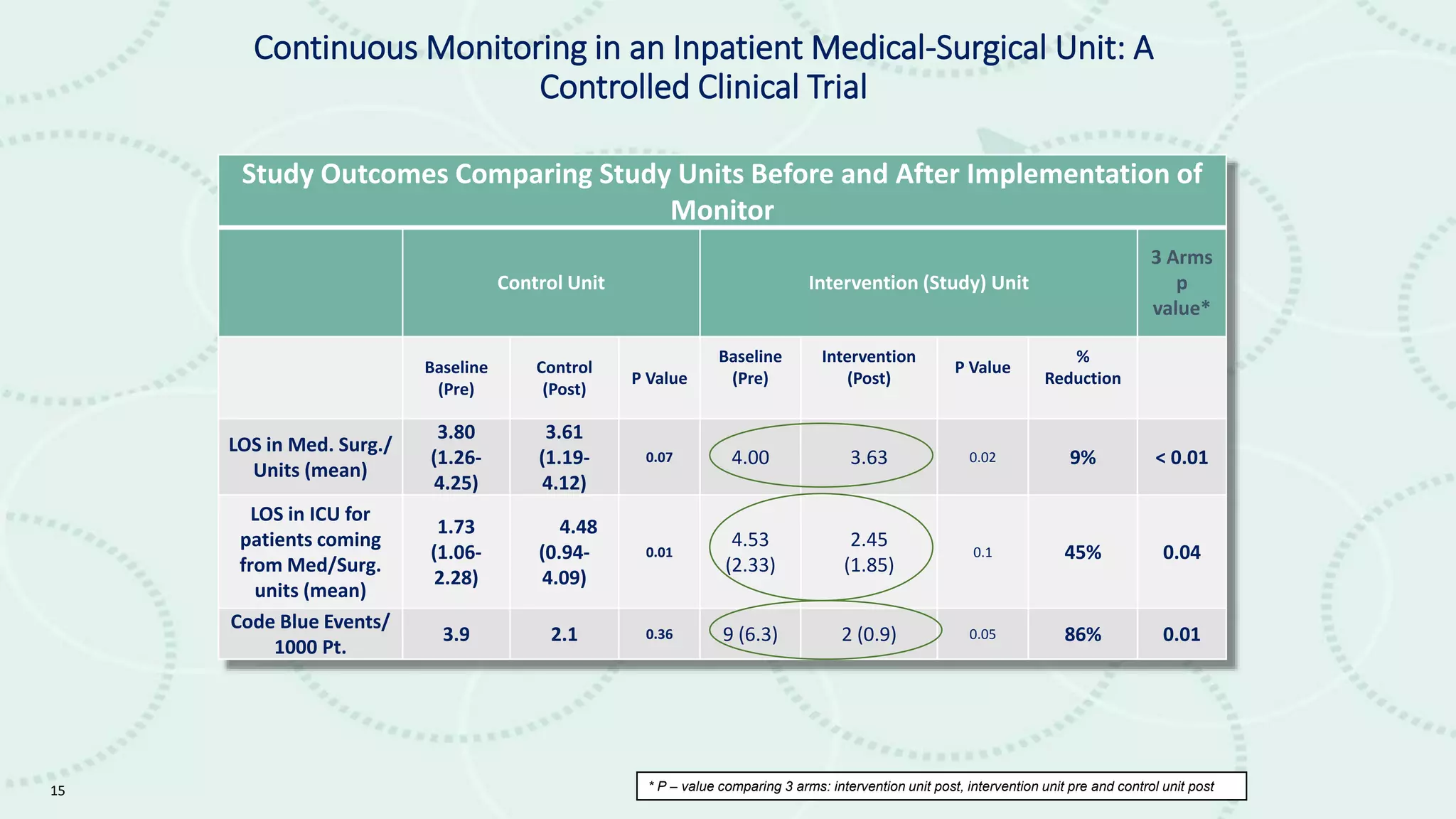
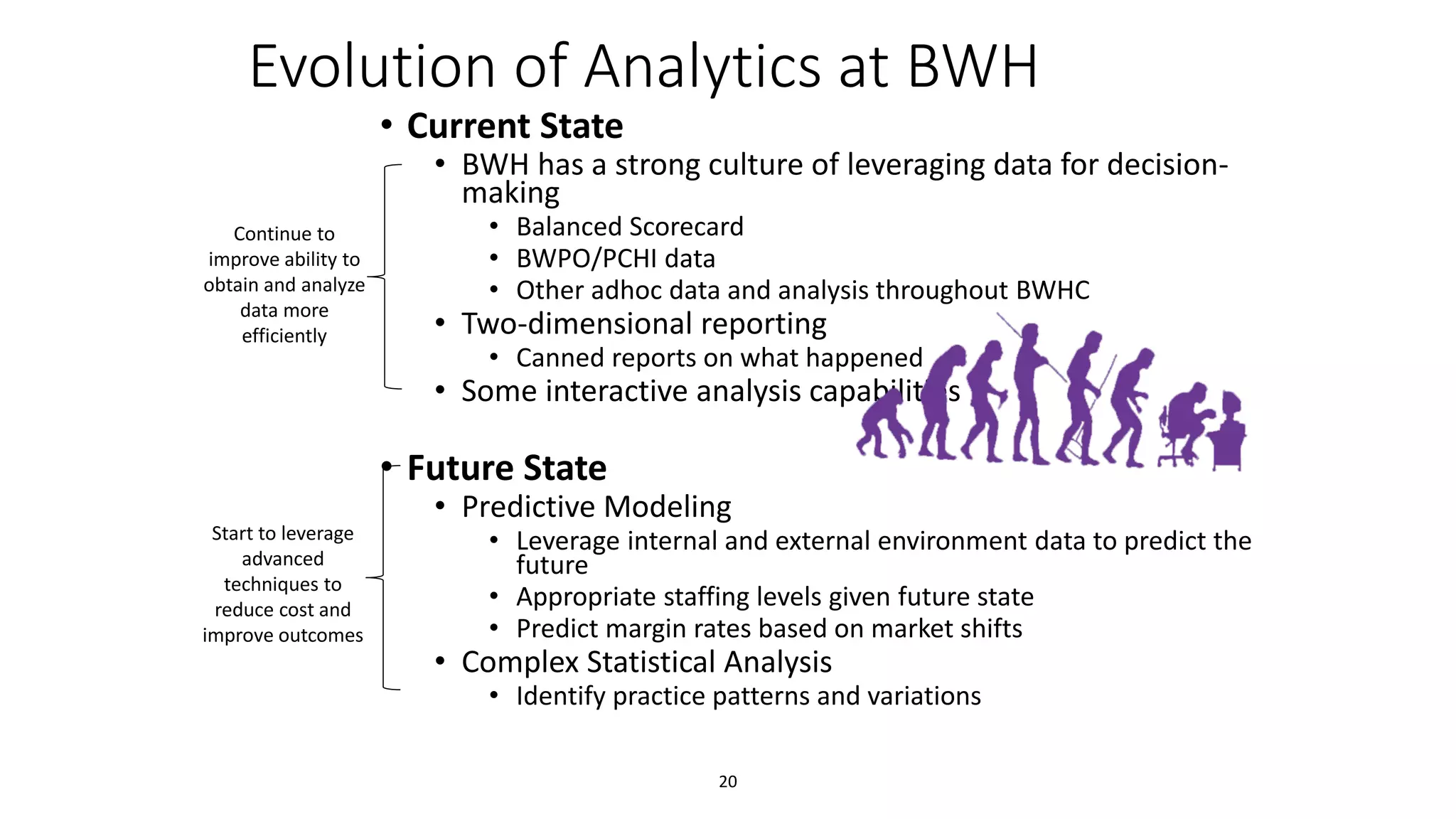
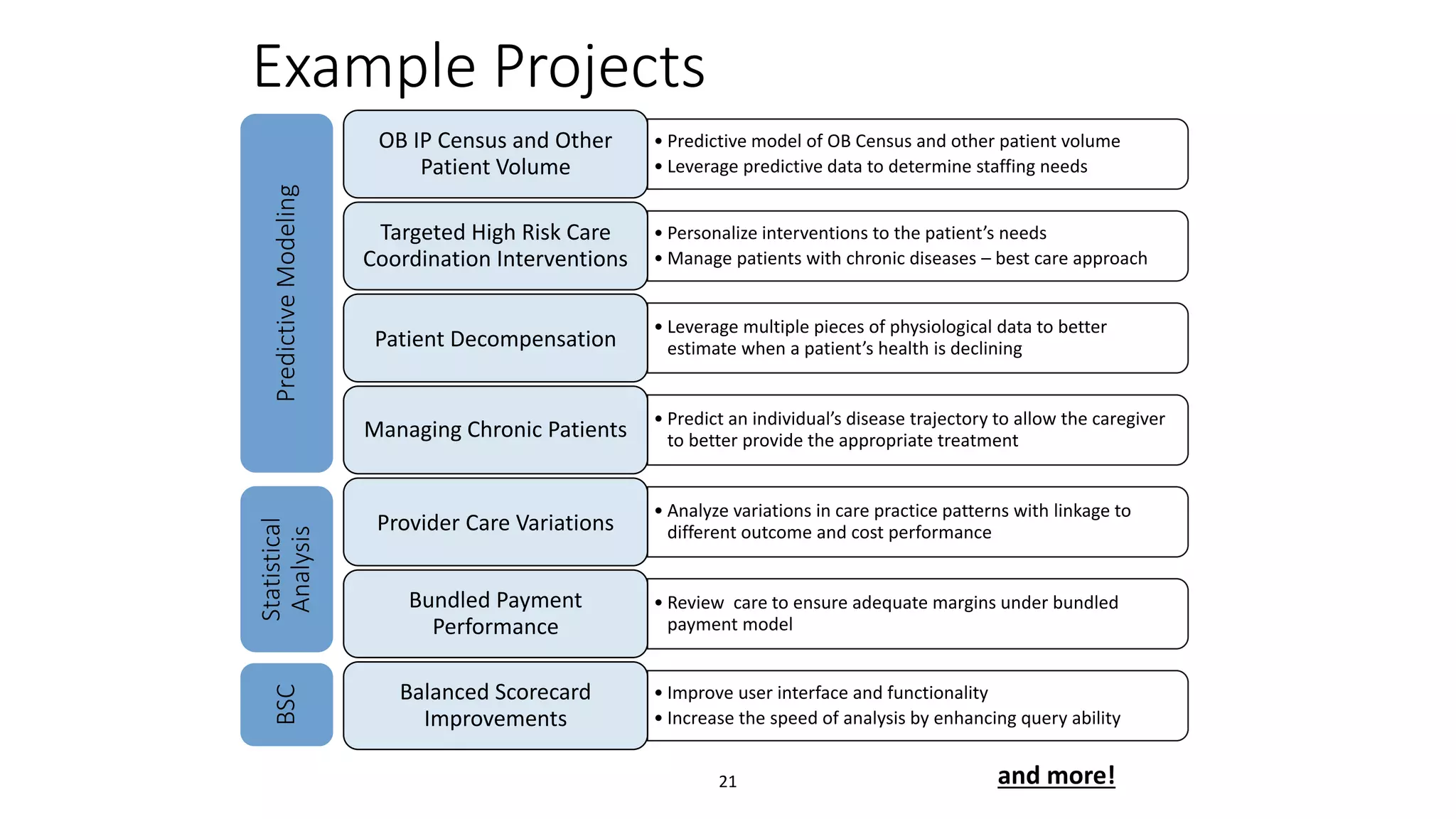
The document discusses the impact of emerging technologies, particularly big data, on the quality of healthcare. It highlights the use of predictive analytics to identify high-cost patients, optimize treatment, and reduce hospital readmissions, emphasizing the role of continuous monitoring and mobile apps in improving patient outcomes. Overall, it underscores the need for a data strategy to leverage these technologies effectively in clinical settings.