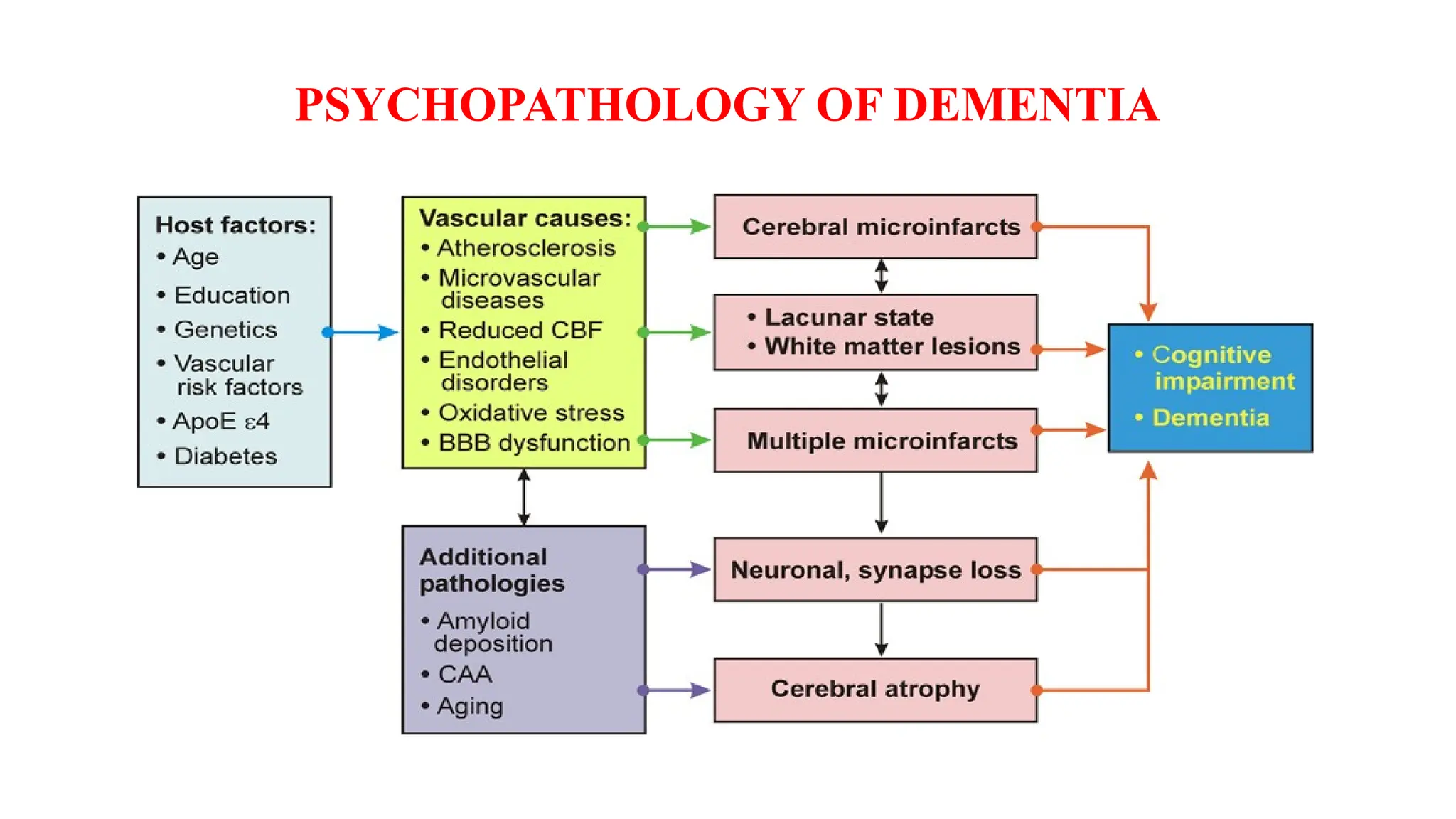
The document outlines objectives and information regarding dementia, specifically focusing on Alzheimer's disease, its etiology, incidence, risk factors, stages, symptoms, diagnosis, and management. It emphasizes the importance of nursing diagnosis and interventions, along with treatment and rehabilitation strategies for both patients and caregivers. The document aims to enhance understanding of dementia-related disorders and their impact on individuals and families.


































![TREATMENT MODALITIES
• T - Tacrin hydrocholoride[cognex]
• T - Donepezil hydrochloride [Aricept]
• Antipsychotic medication
• Benzodiazepines
• Antidepressants
• Anticonvulsants
• Other prophylactic nutritional agents](https://image.slidesharecdn.com/dementia-organicdisoder-1-241020174537-9a266d8b/75/dementia-organic-disorders-mental-health-nursing-40-2048.jpg)