The document presents an overview of bundled payment changes and strategies to succeed in implementing them, particularly focusing on the Bundled Payments for Care Improvement (BPCI) Advanced program. It discusses the operationalization of these payment models, data utilization, and key activities for driving successful transformation in care delivery. Key sections cover an outline of bundled payment programs, opportunities for clinical transformation, and the necessary data sources and leadership structures needed for effective implementation.






![© 2018
Health
Catalyst
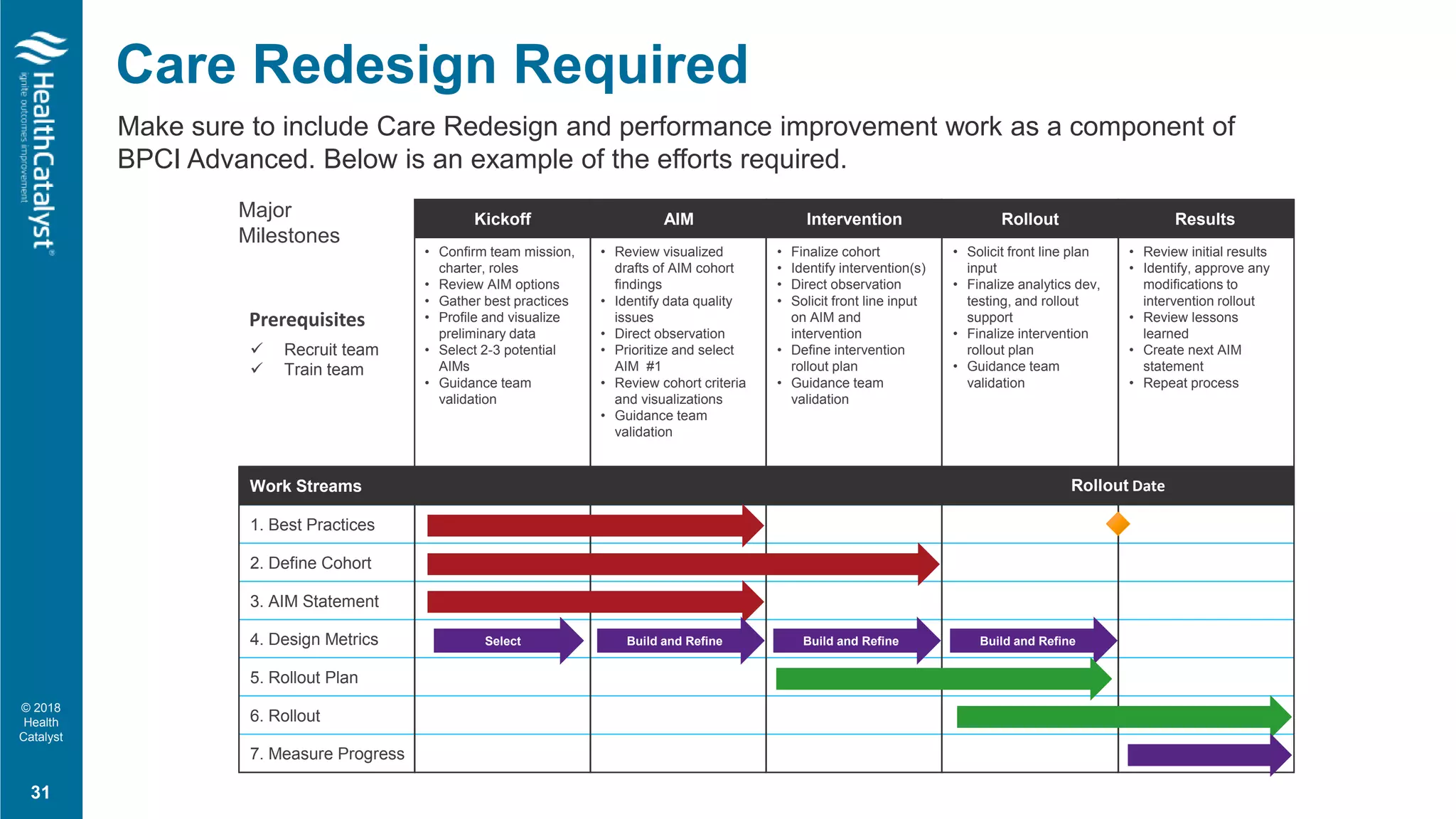
Components of a Bundle
• Goal of ACOs: Reduce annual
total cost of care across the care
continuum
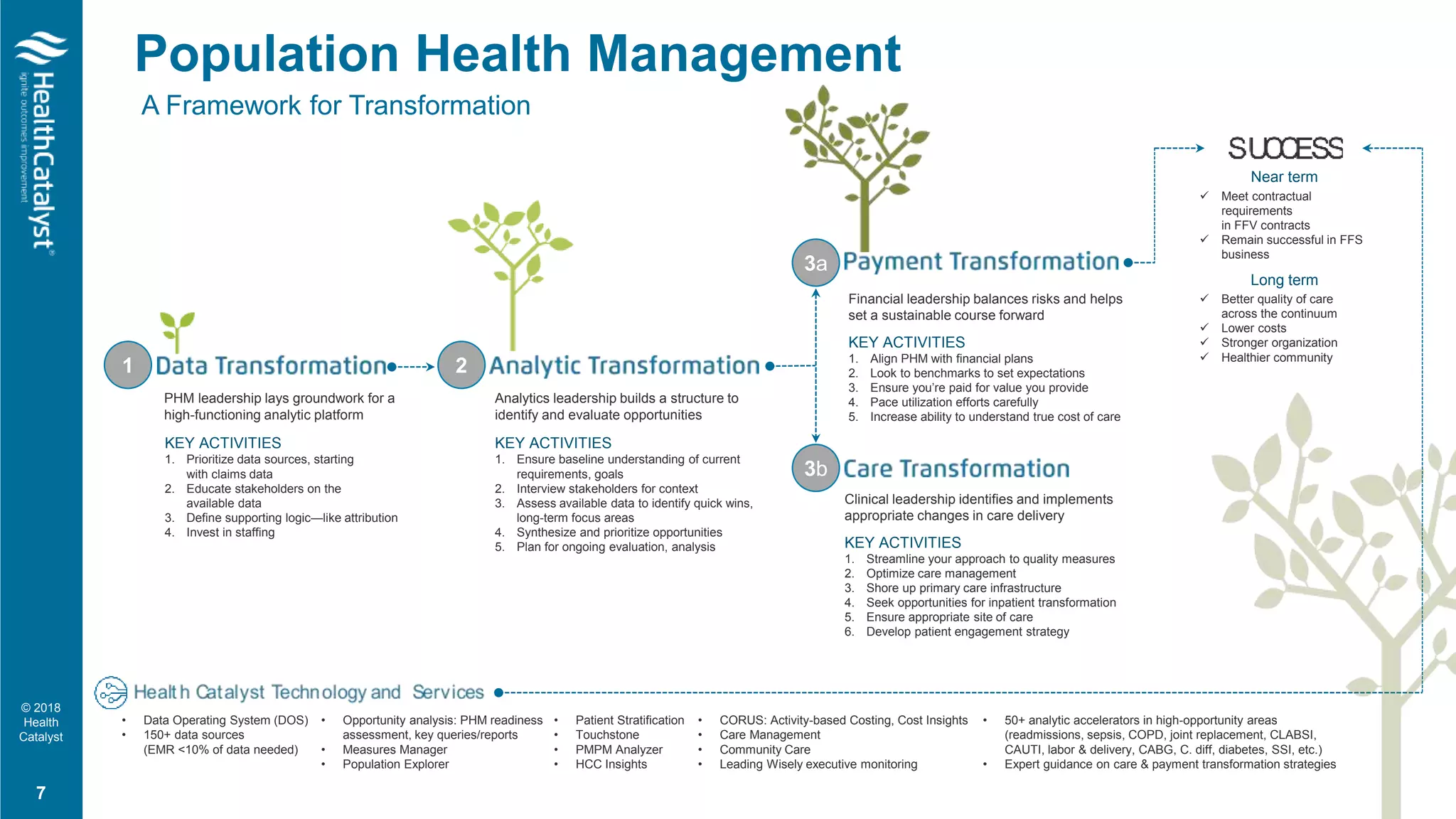
• Scale PHM Infrastructure
HCPLAN’s Components of
Episodes of Care Components of PHM Infrastructures:
9
Source: Health Care Payment Learning & Action Network. (2016). Clinical
Episode Payment Models [White paper].
https://www.friends.edu/wp-content/uploads/2015/08/ElectronicReference.pdf
Accountable
Entity
IPA
Entity
Ind.
MDs
Hospital
/ Health
System
Post-
Acute
Care](https://image.slidesharecdn.com/2018-06-20bundledpayments-final-180621171113/75/Bundled-Payment-Changes-Learn-What-s-New-and-How-to-Succeed-9-2048.jpg)