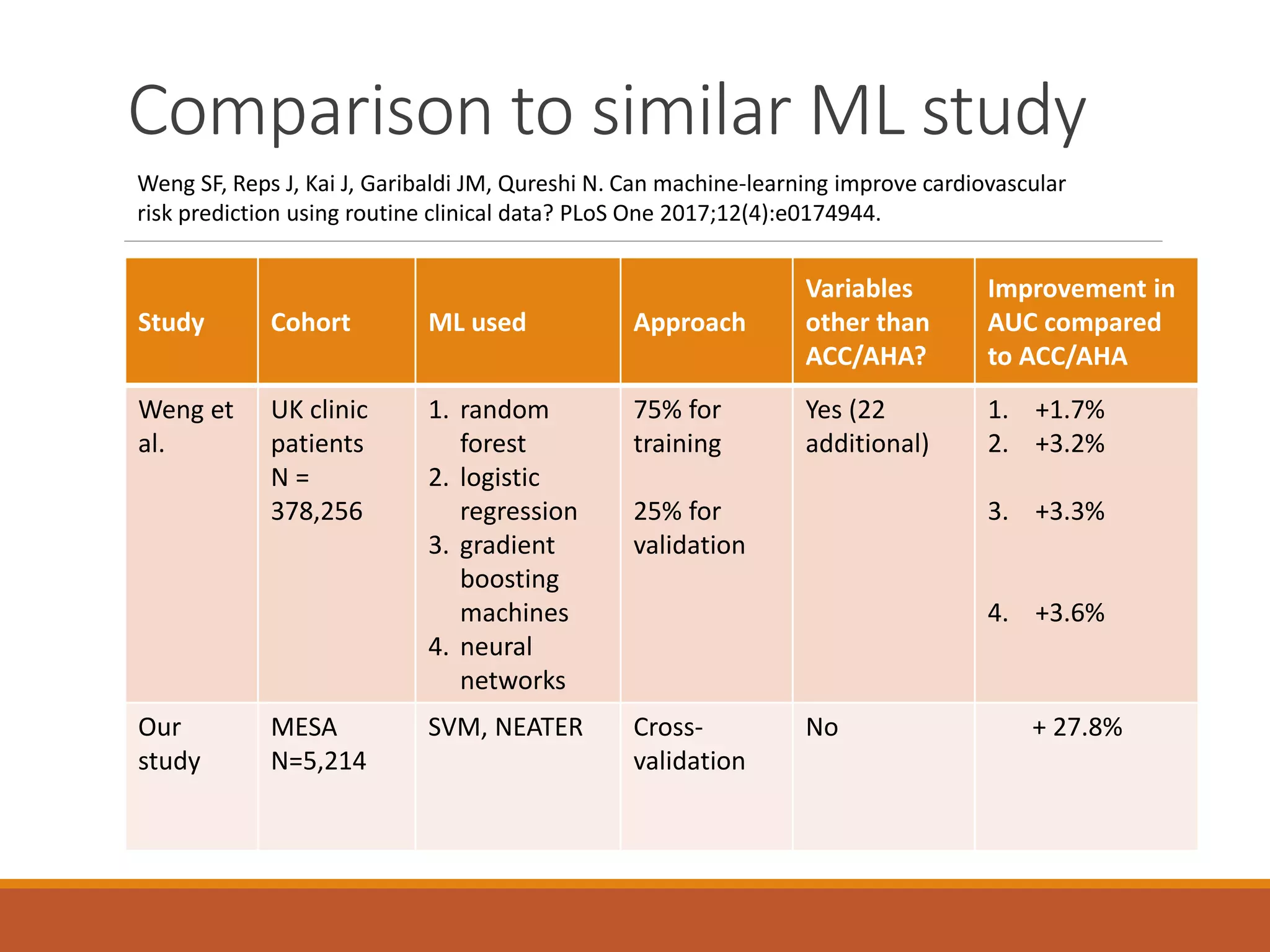
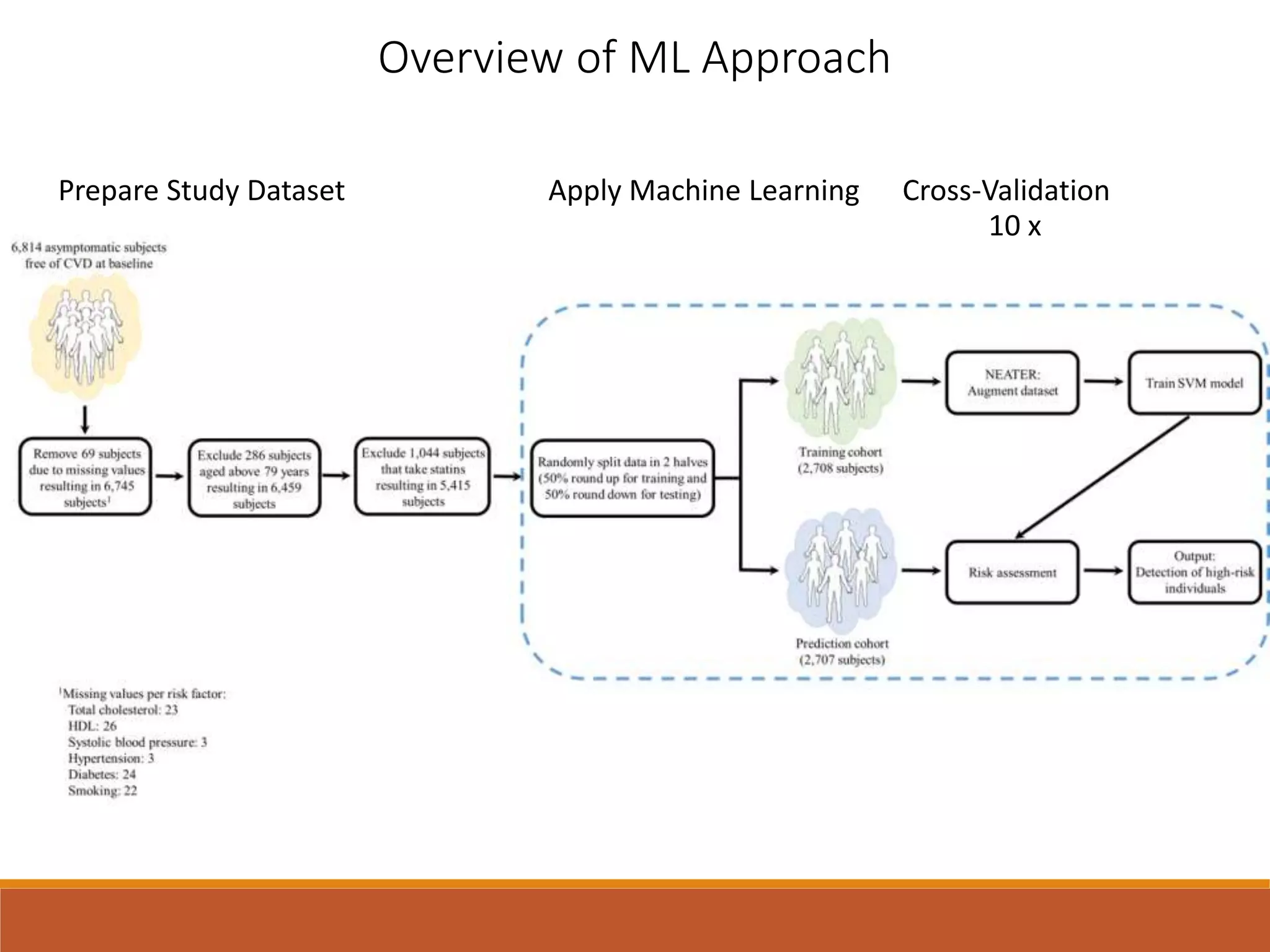
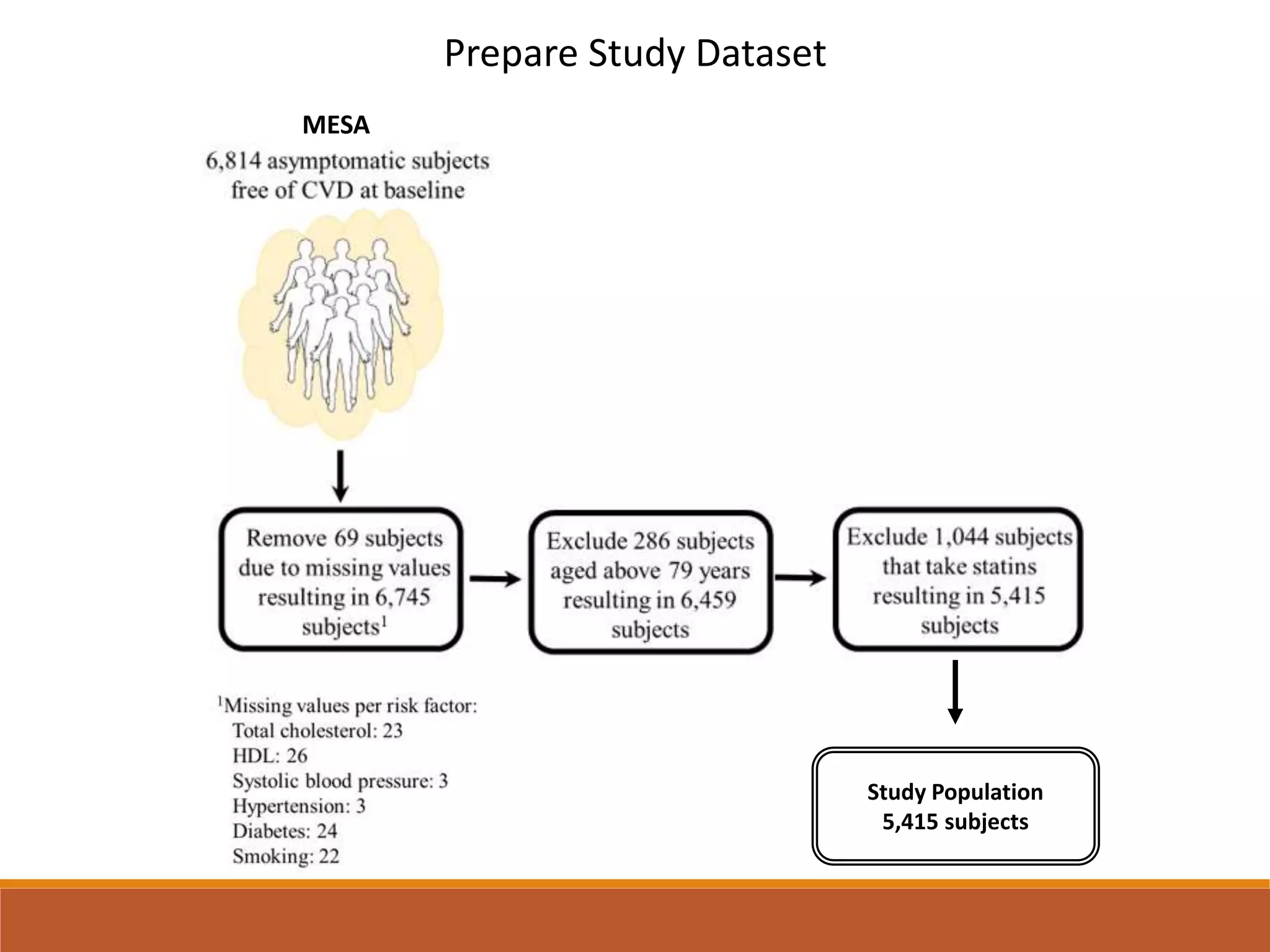
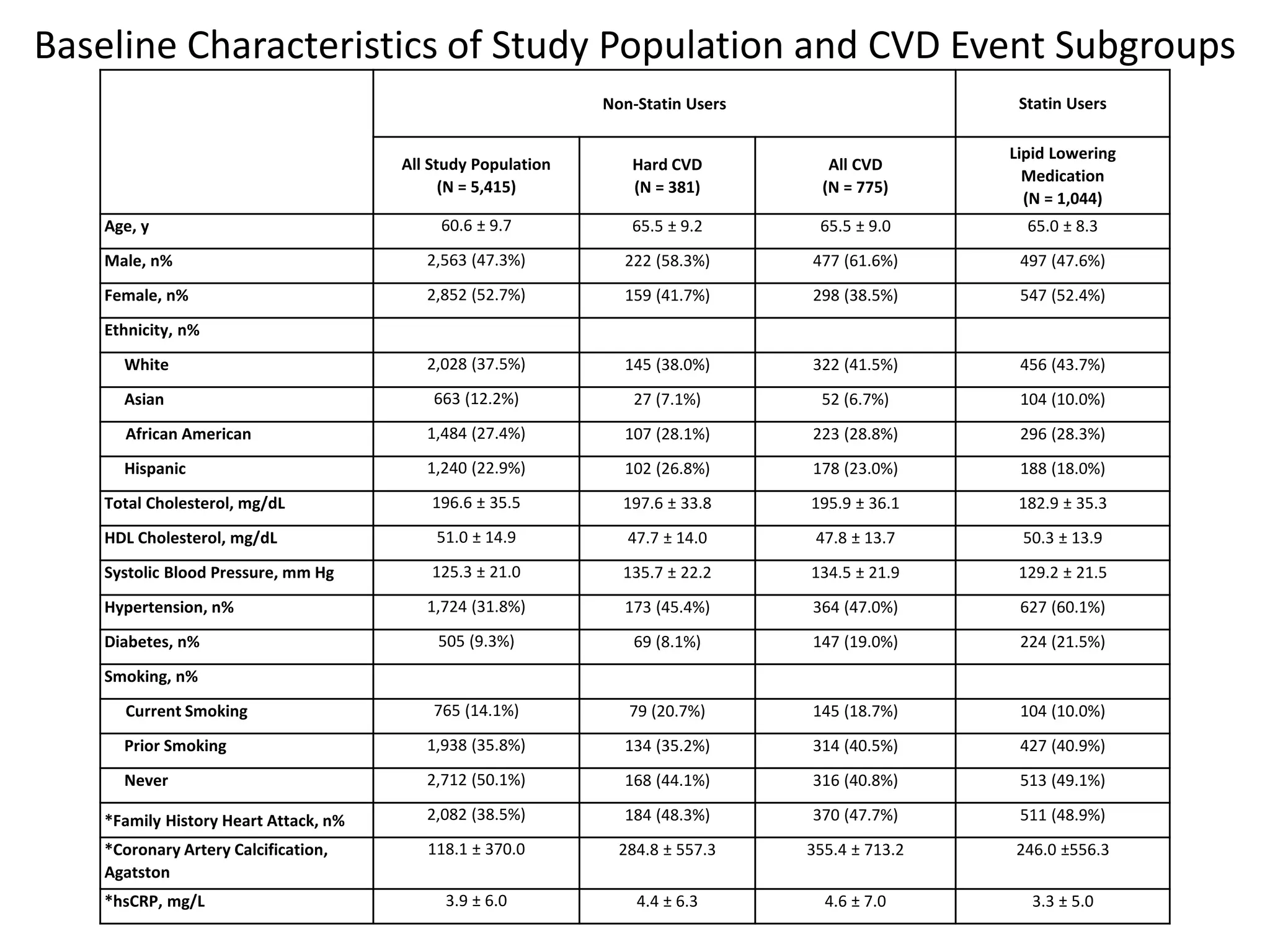
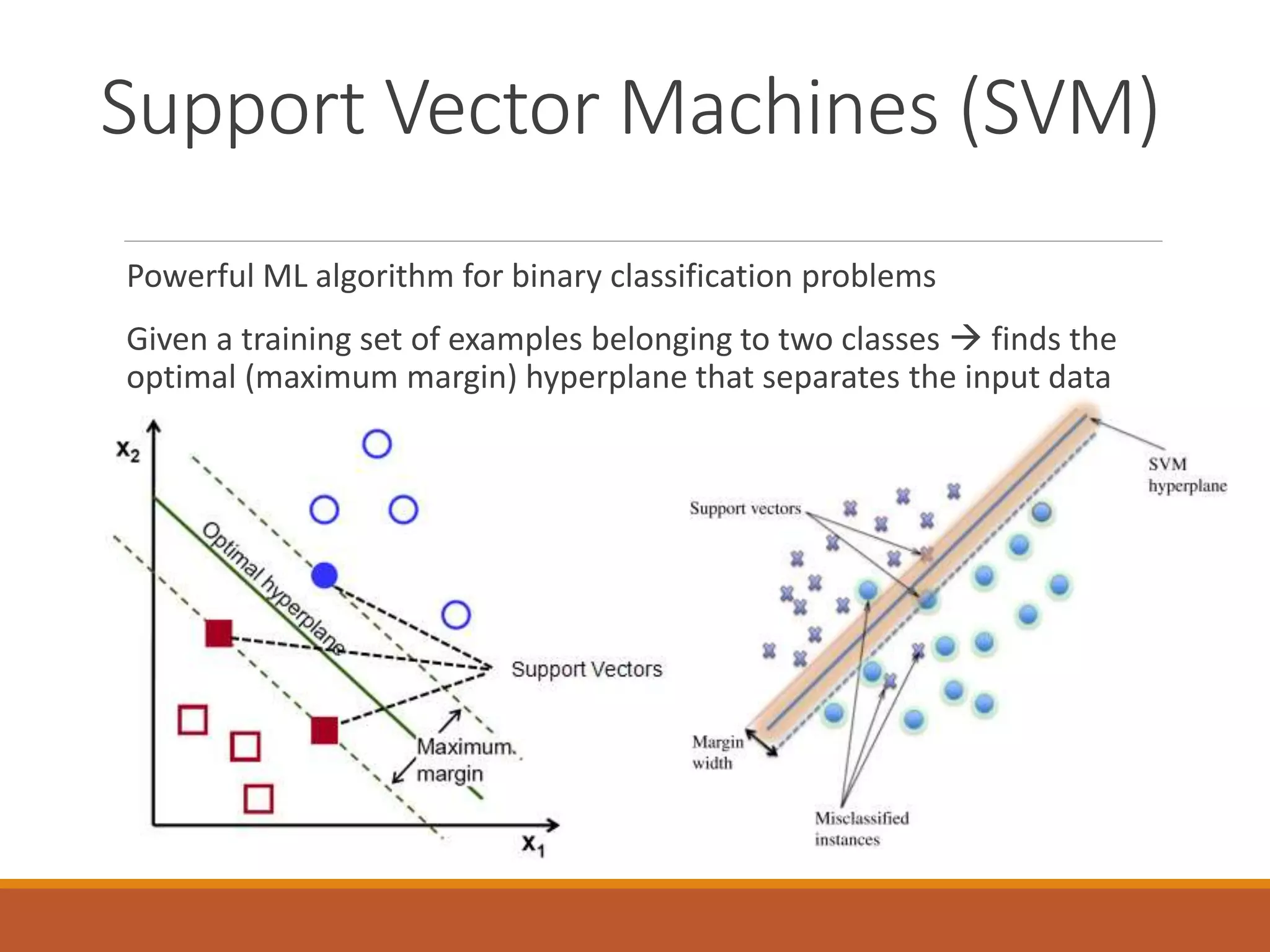
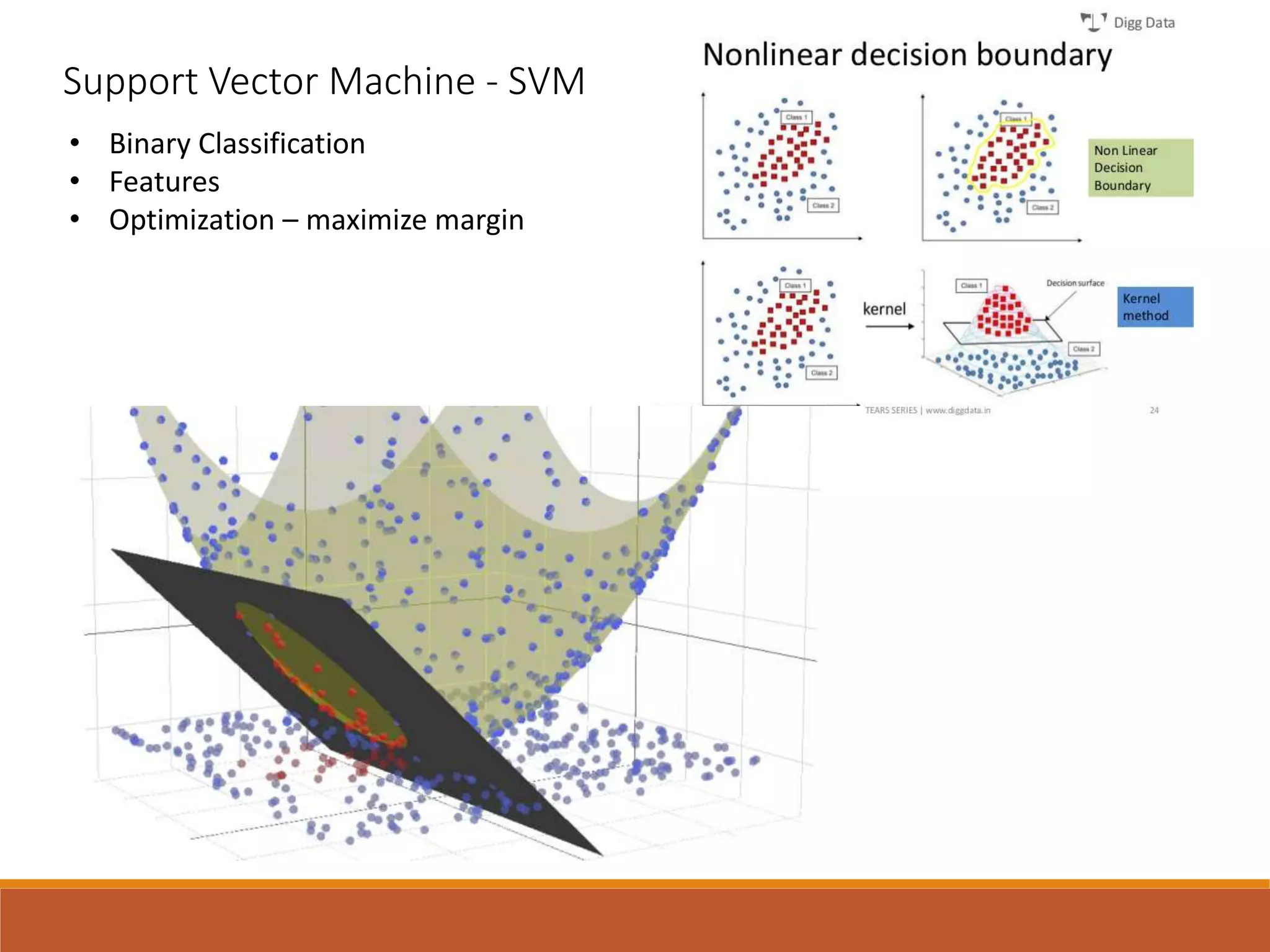
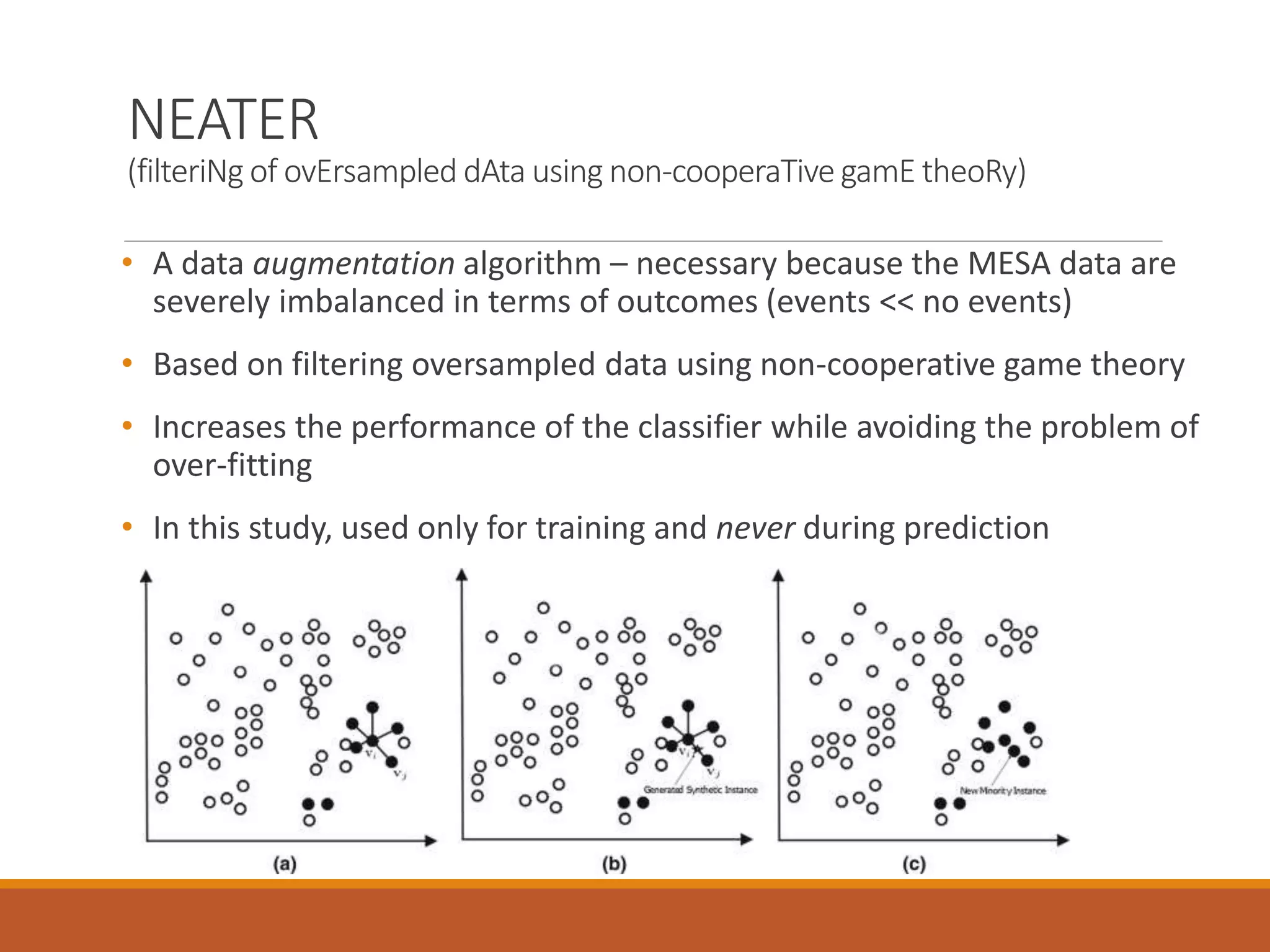
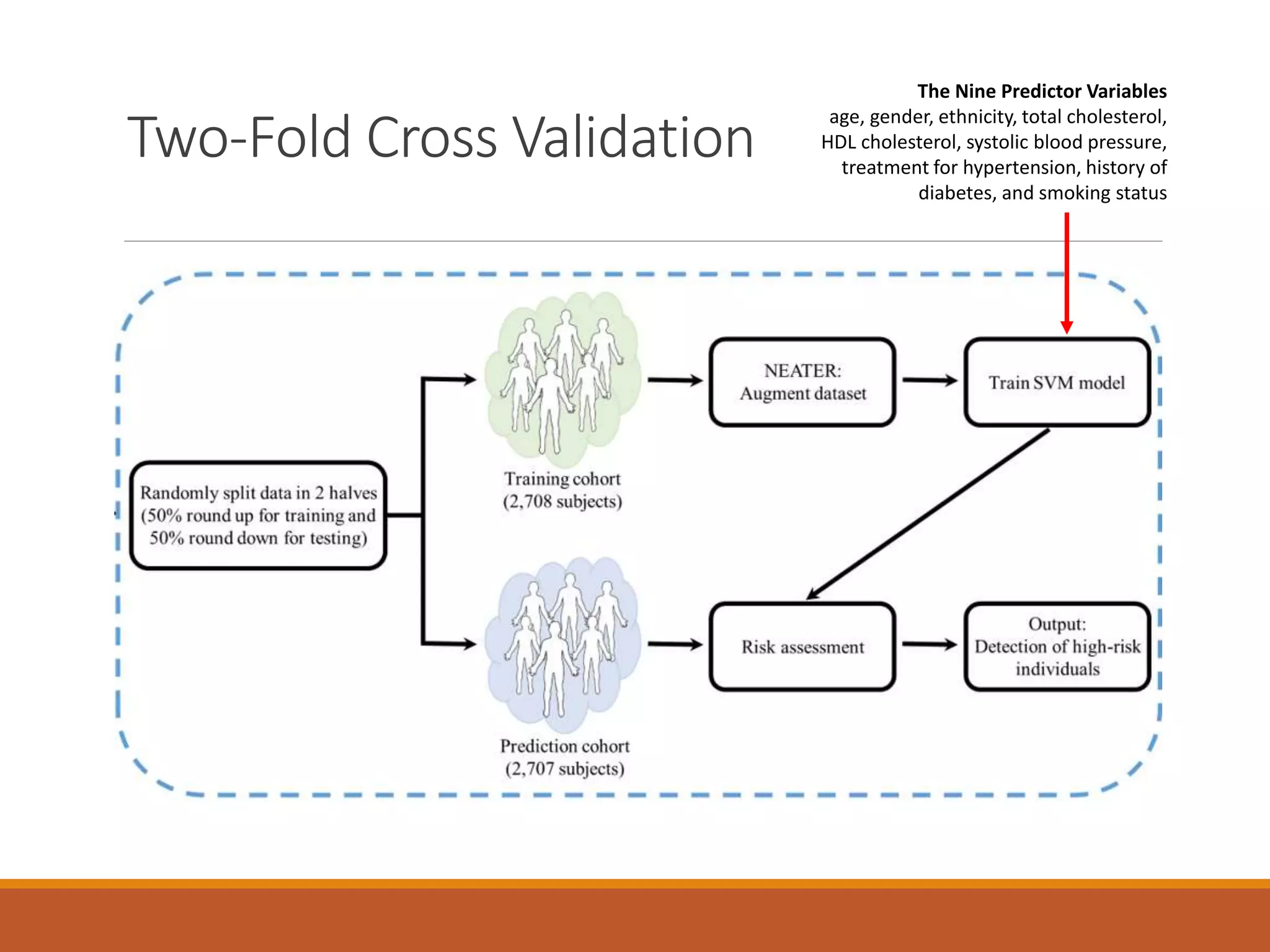
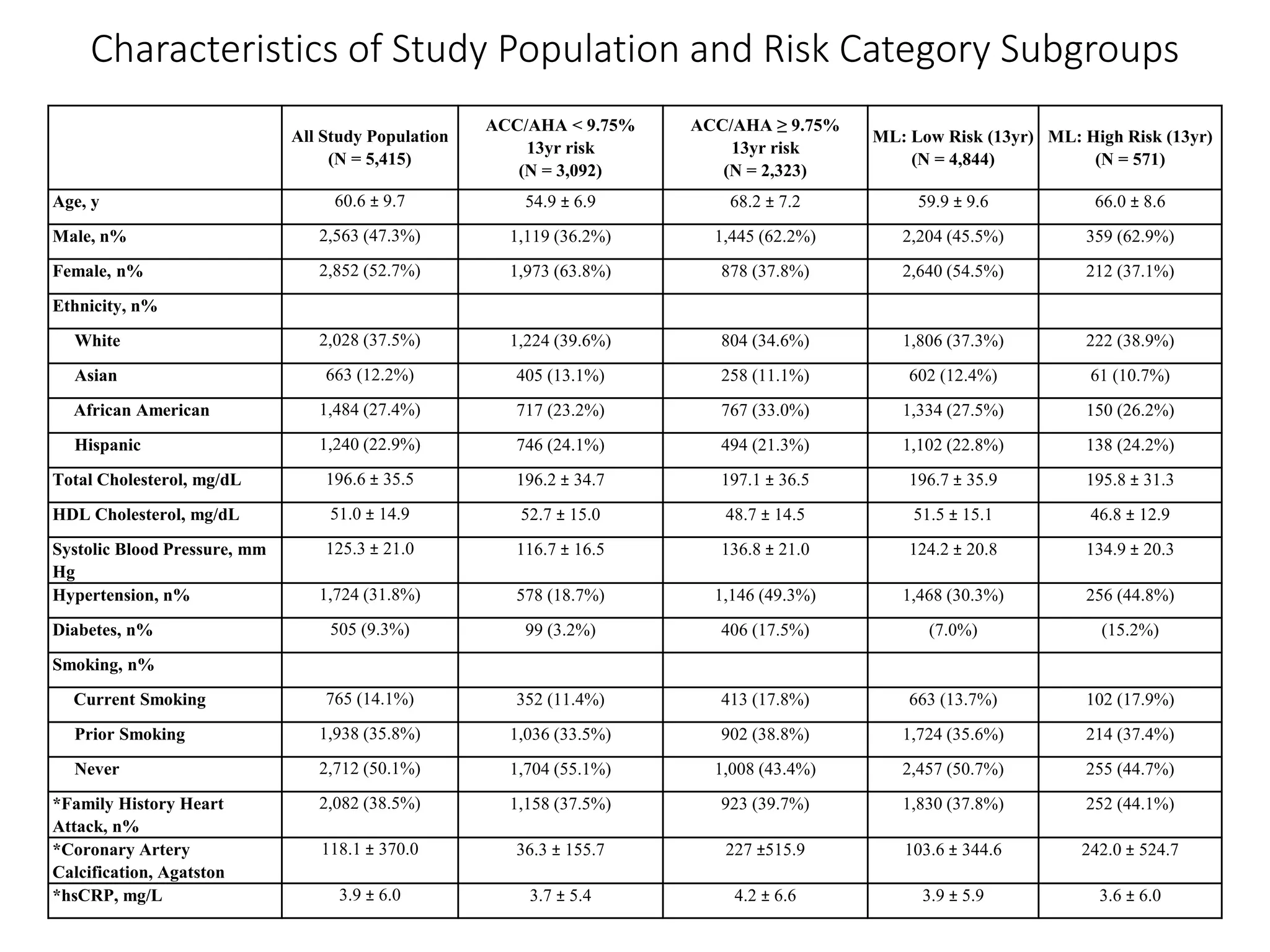
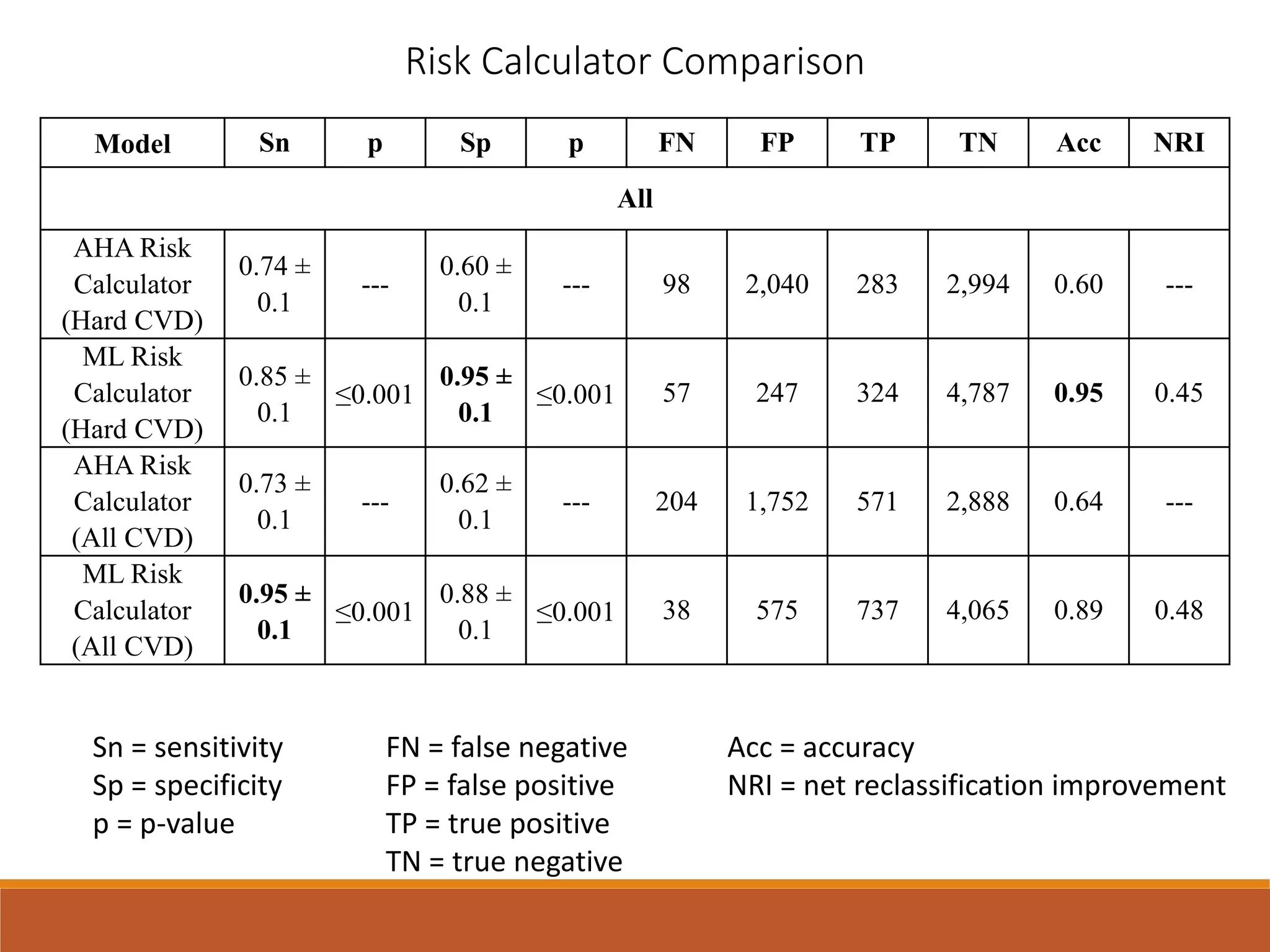
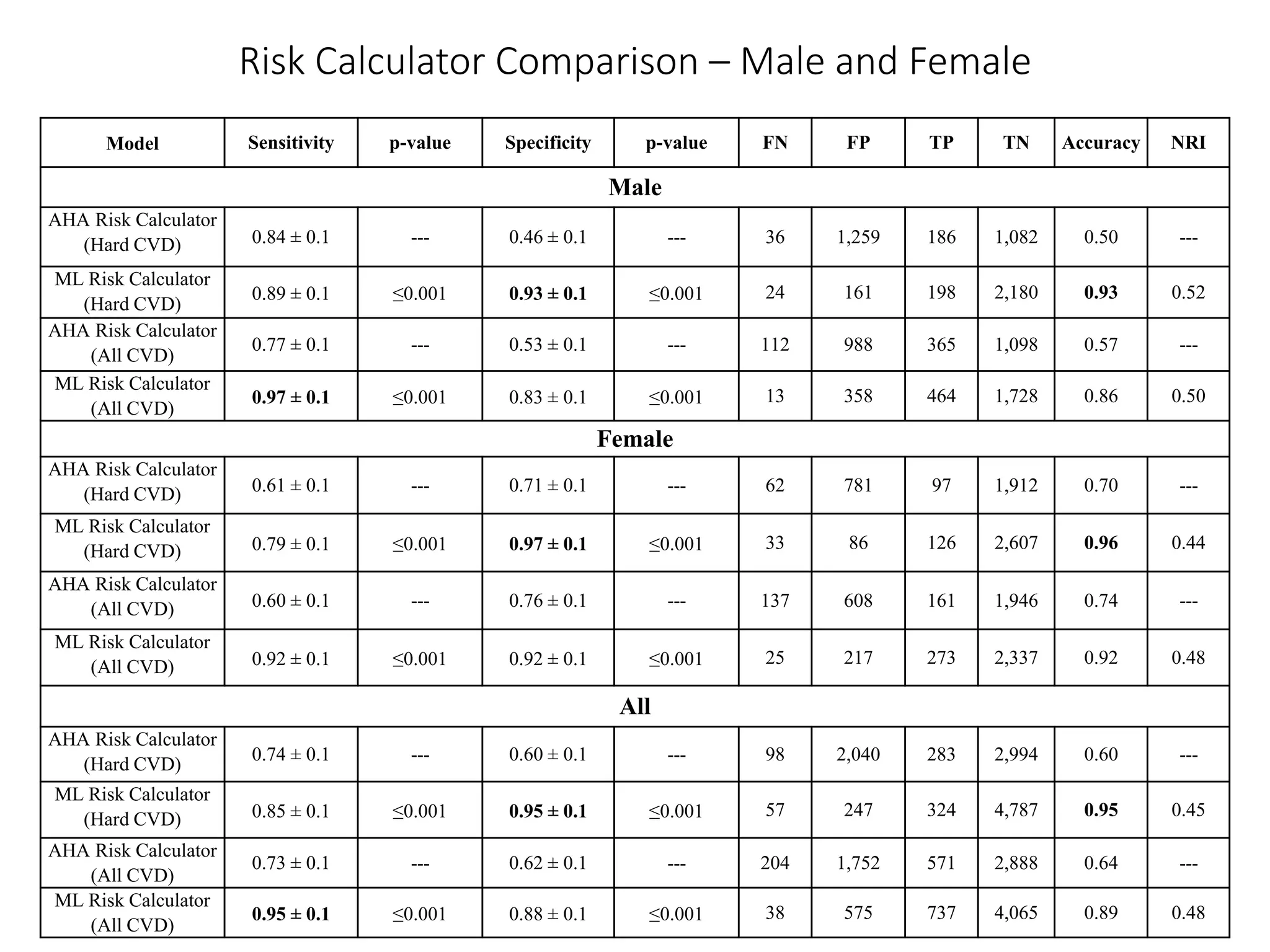
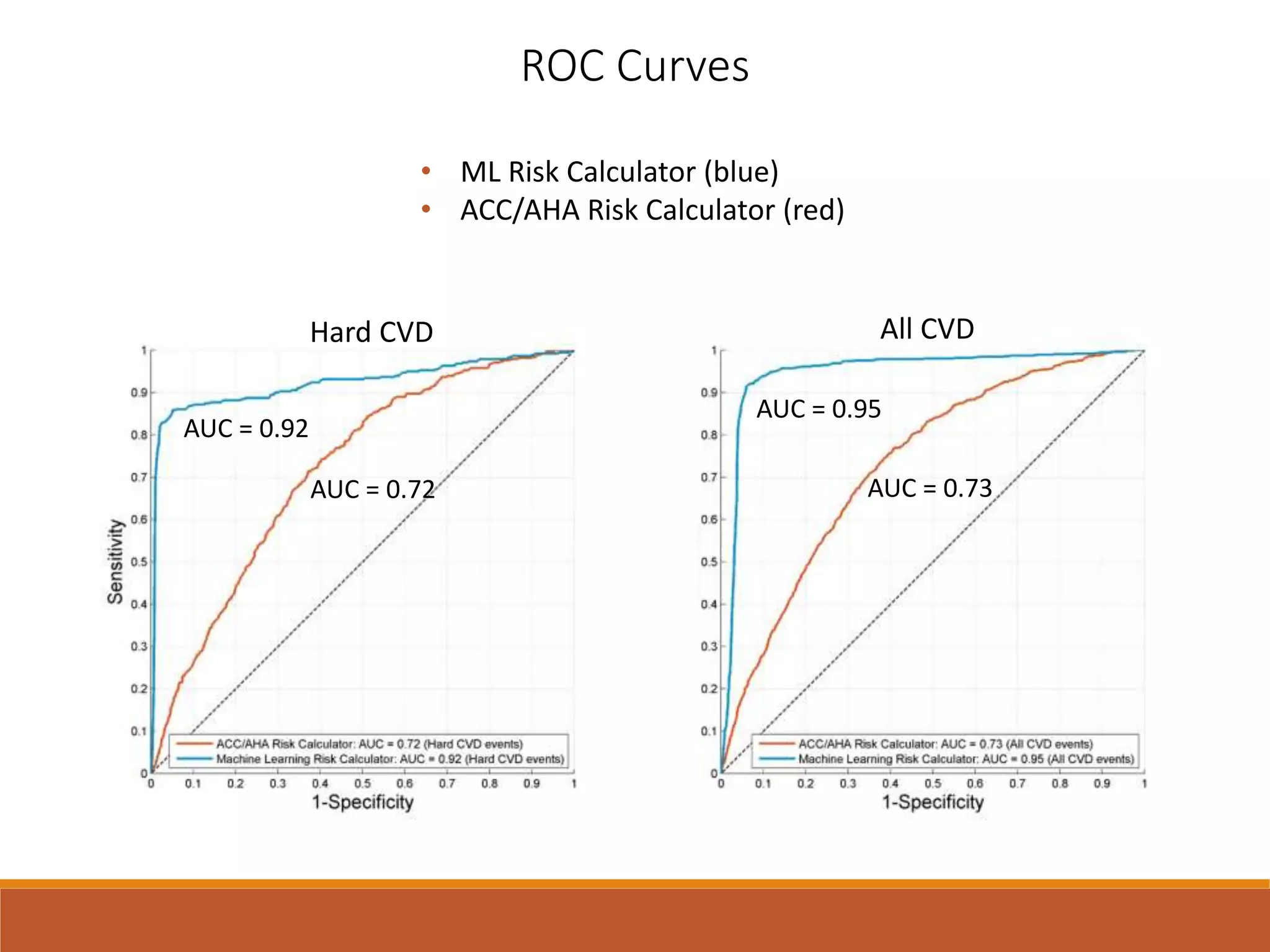
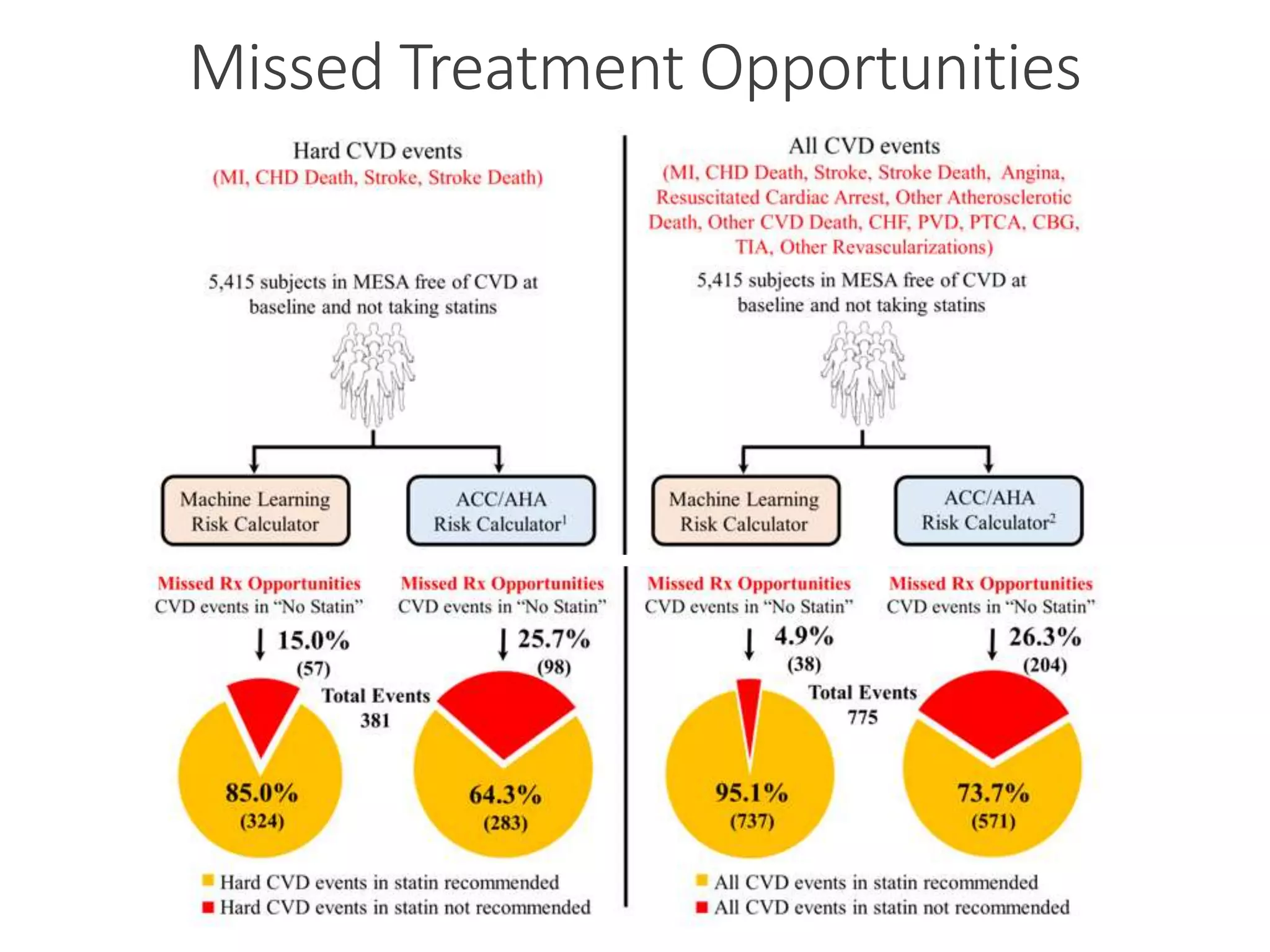
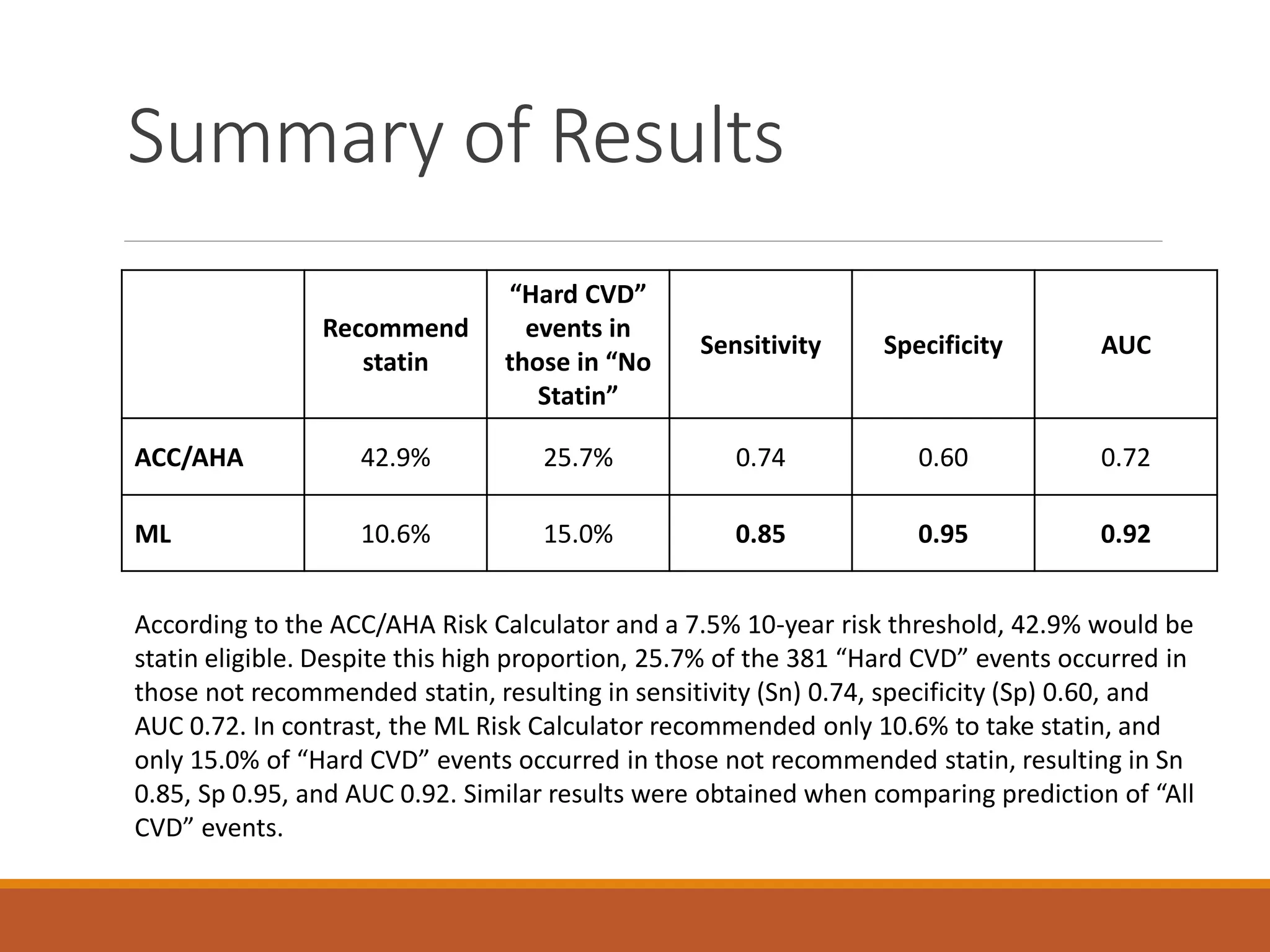
A machine learning model outperformed the ACC/AHA Pooled Cohort Equations Risk Calculator in detecting high-risk asymptomatic individuals and recommending statin treatment for cardiovascular disease prevention in the Multi-Ethnic Study of Atherosclerosis. The machine learning model used support vector machines and data augmentation to derive a CVD risk predictor from nine variables in the MESA study population. It demonstrated higher sensitivity, specificity, and AUC compared to the ACC/AHA risk calculator, recommending statin treatment for fewer individuals while missing fewer cardiovascular events.