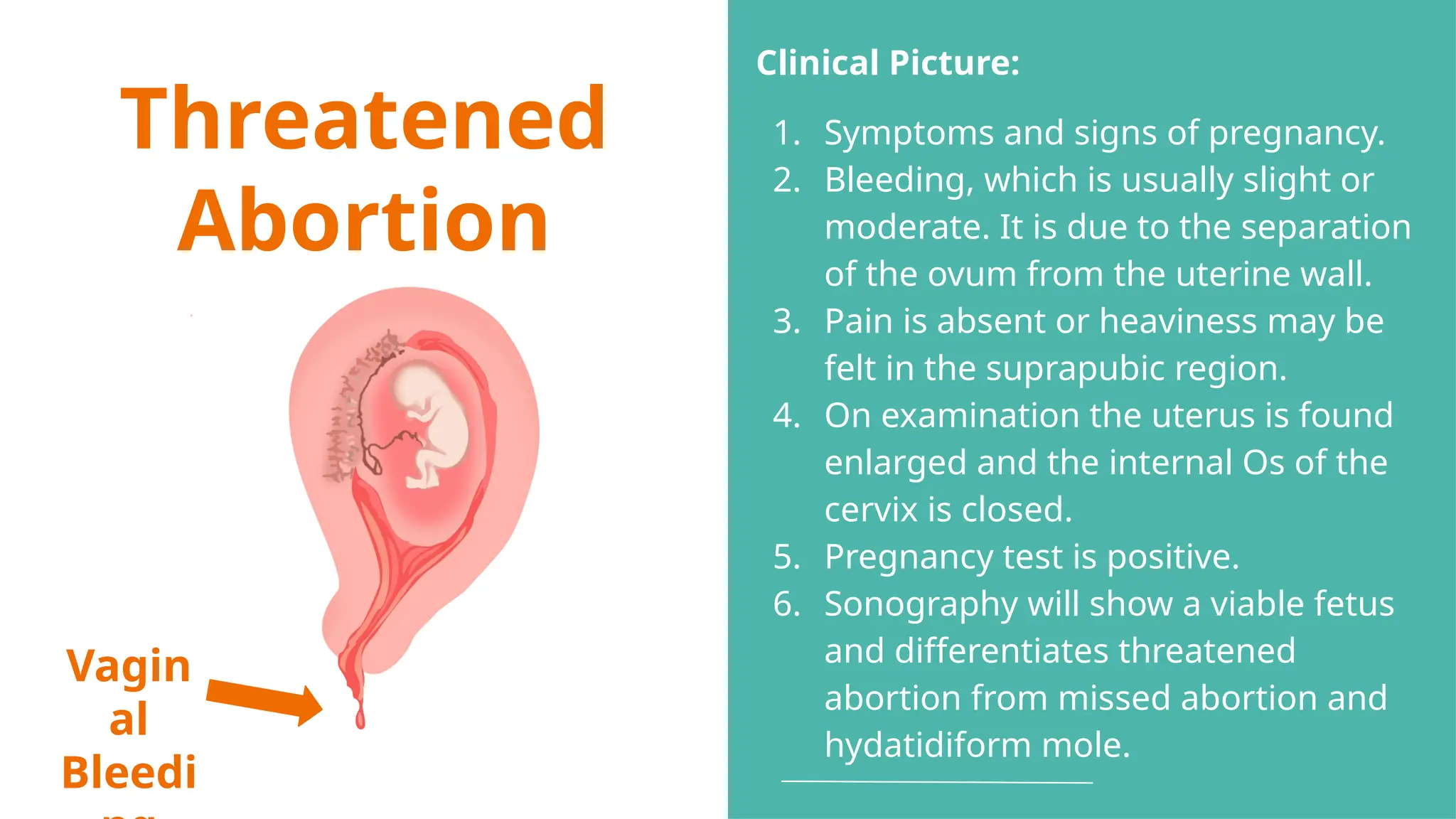
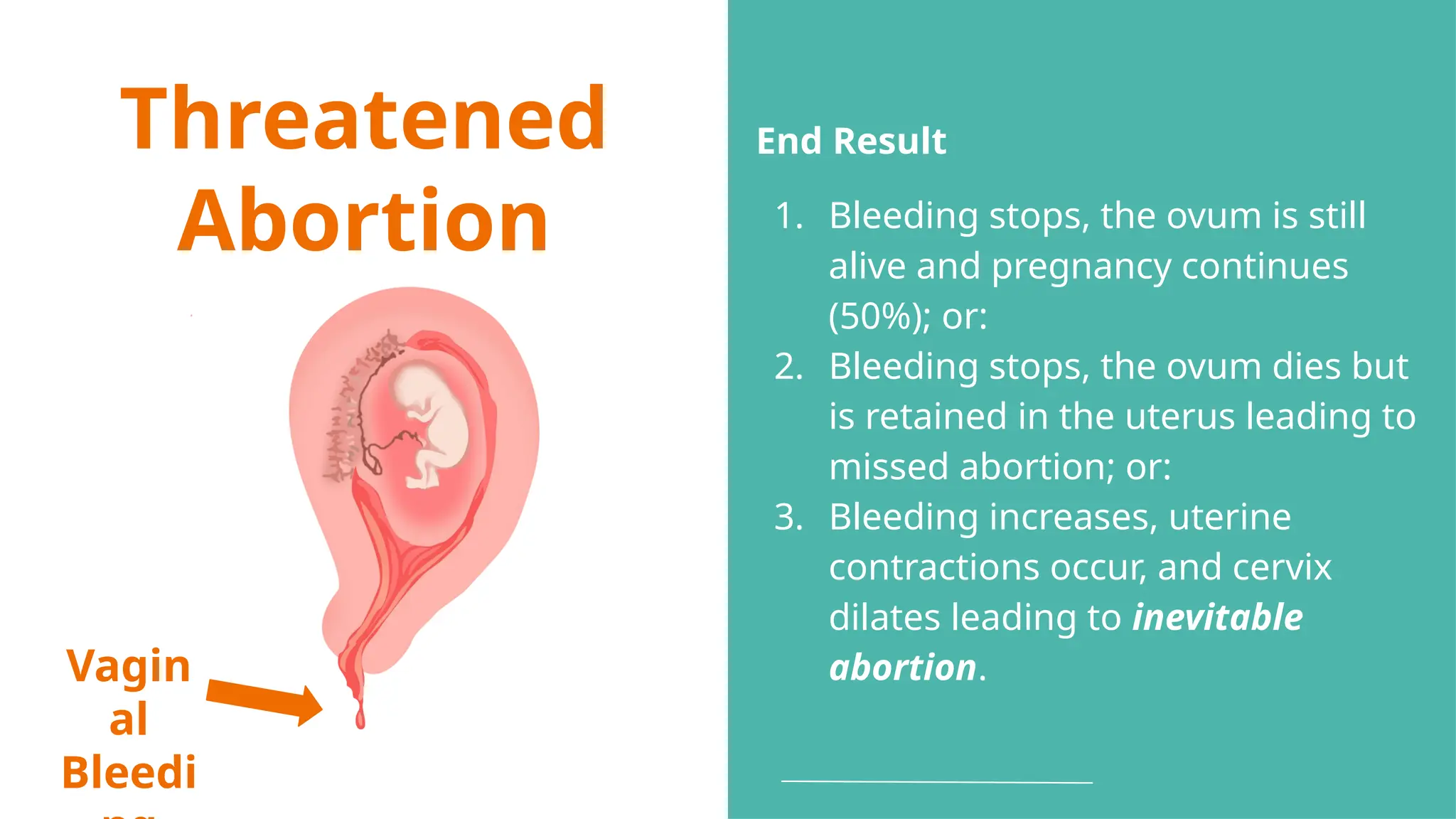
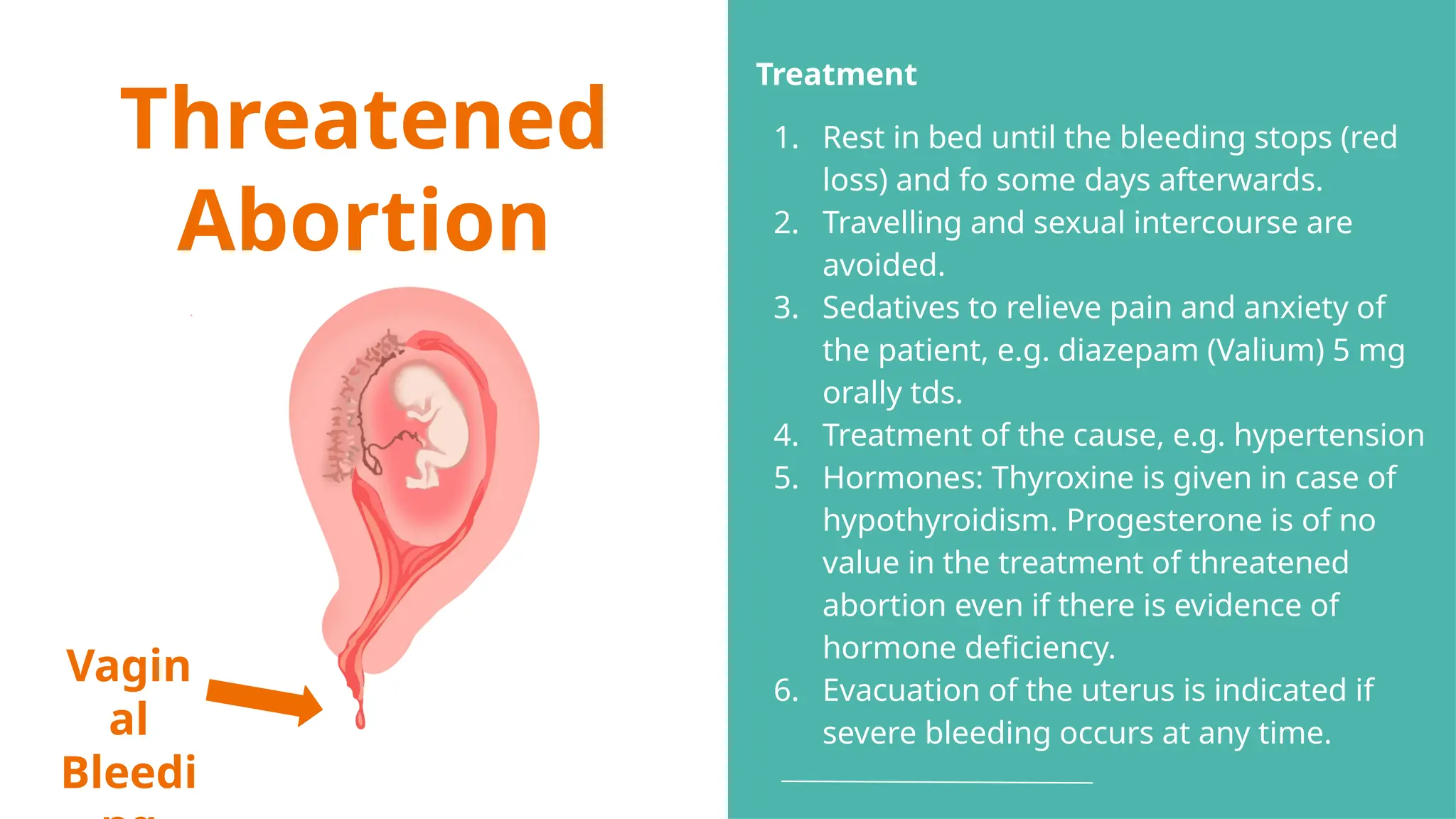
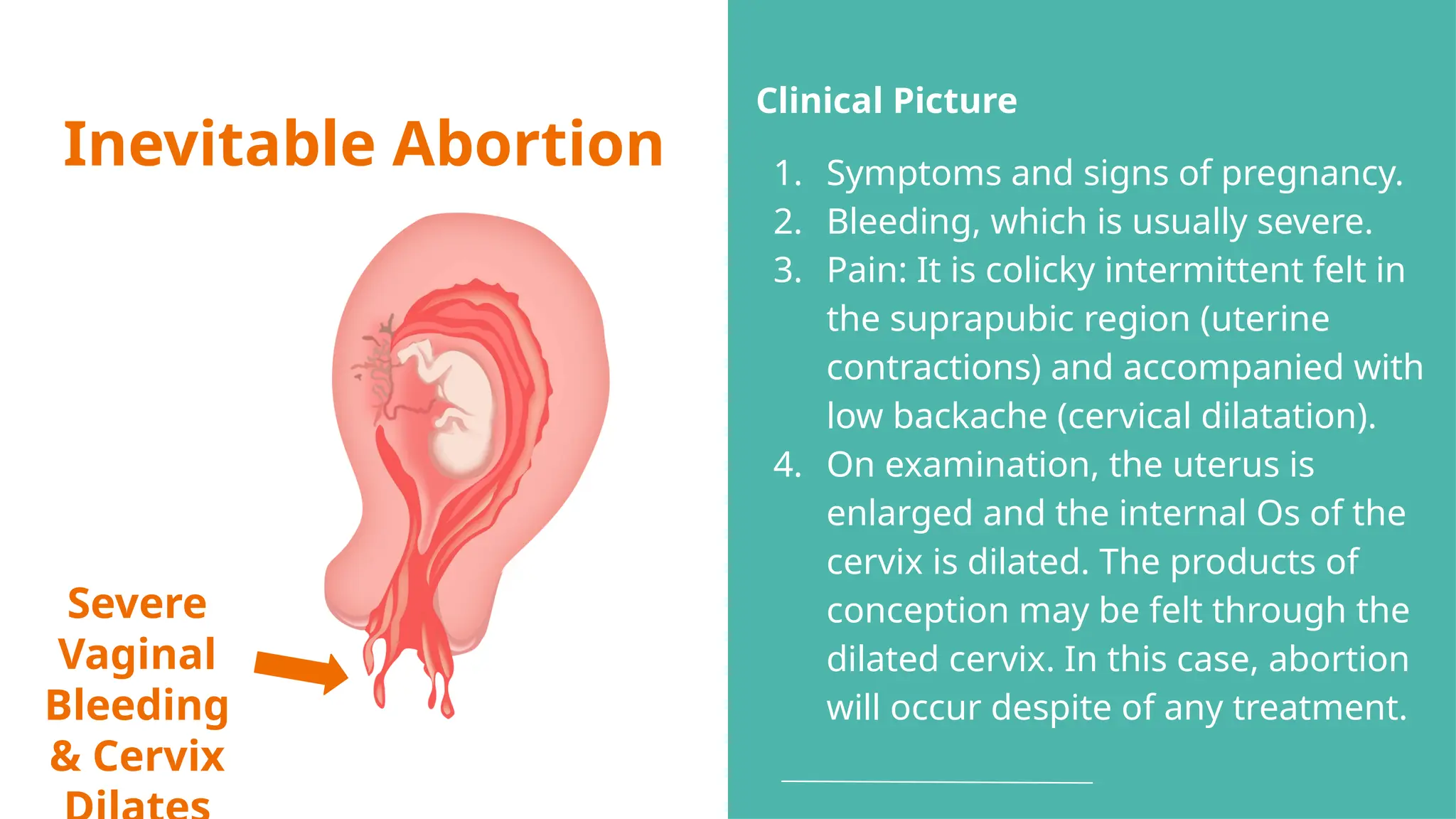
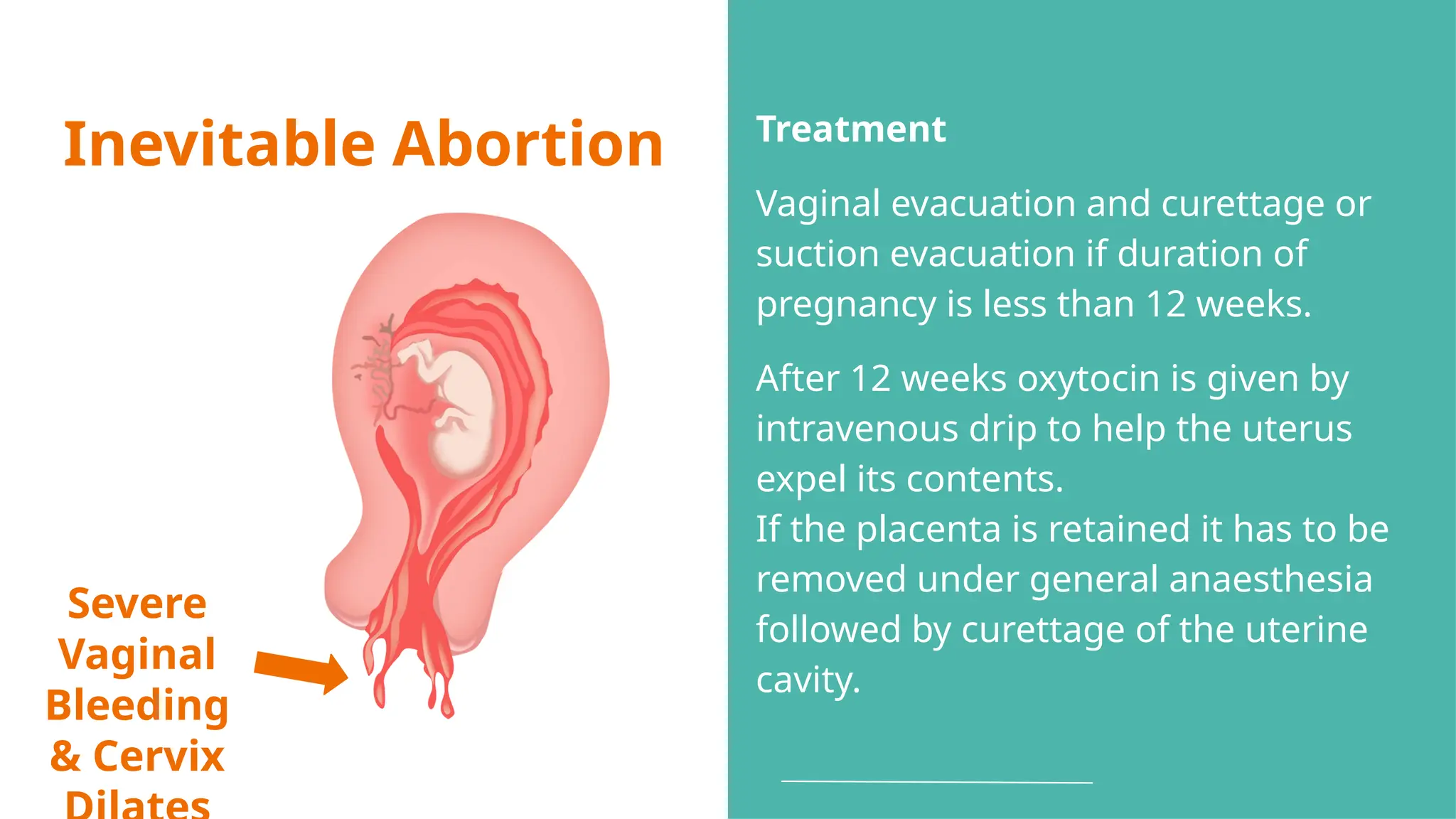
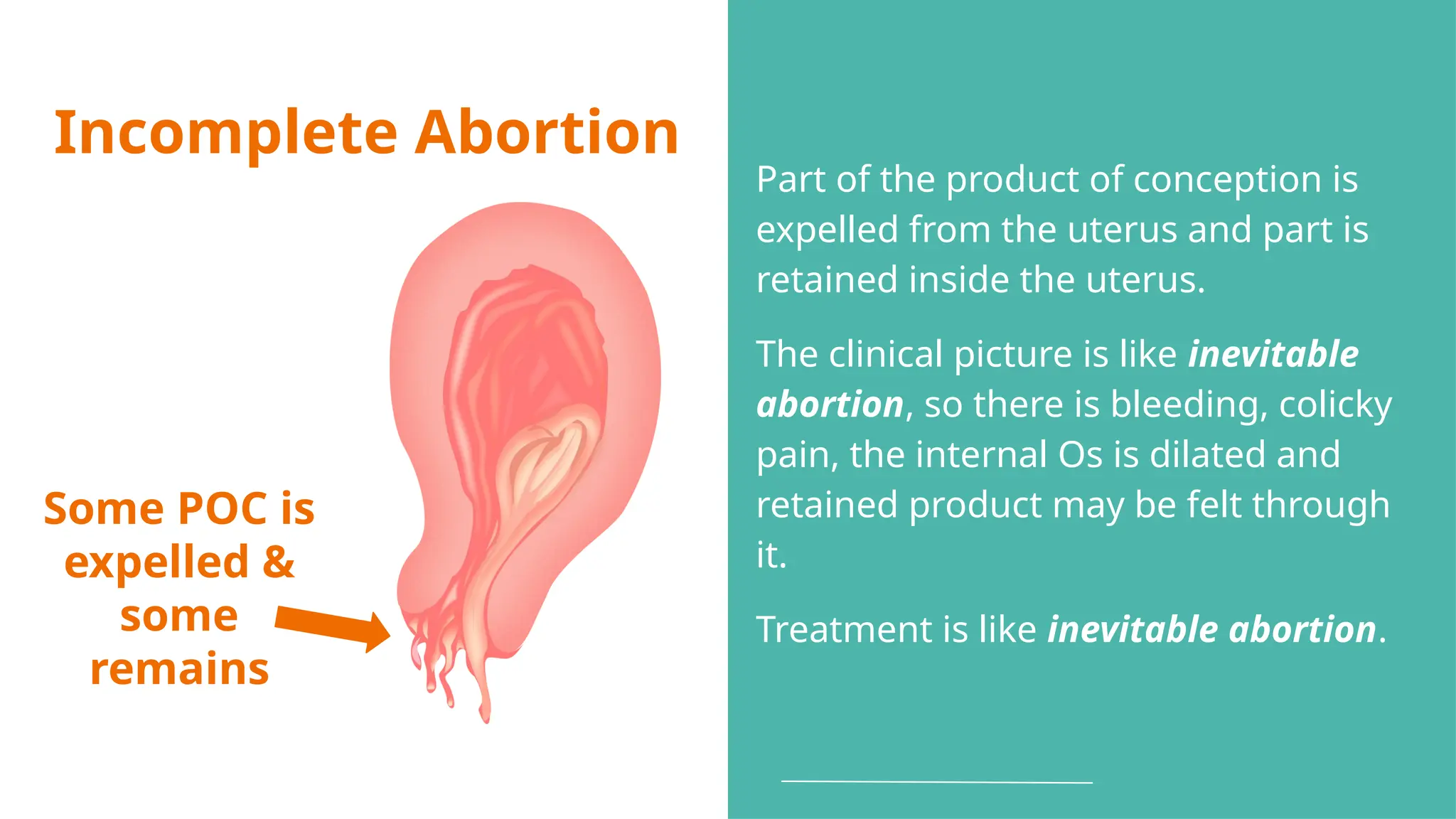
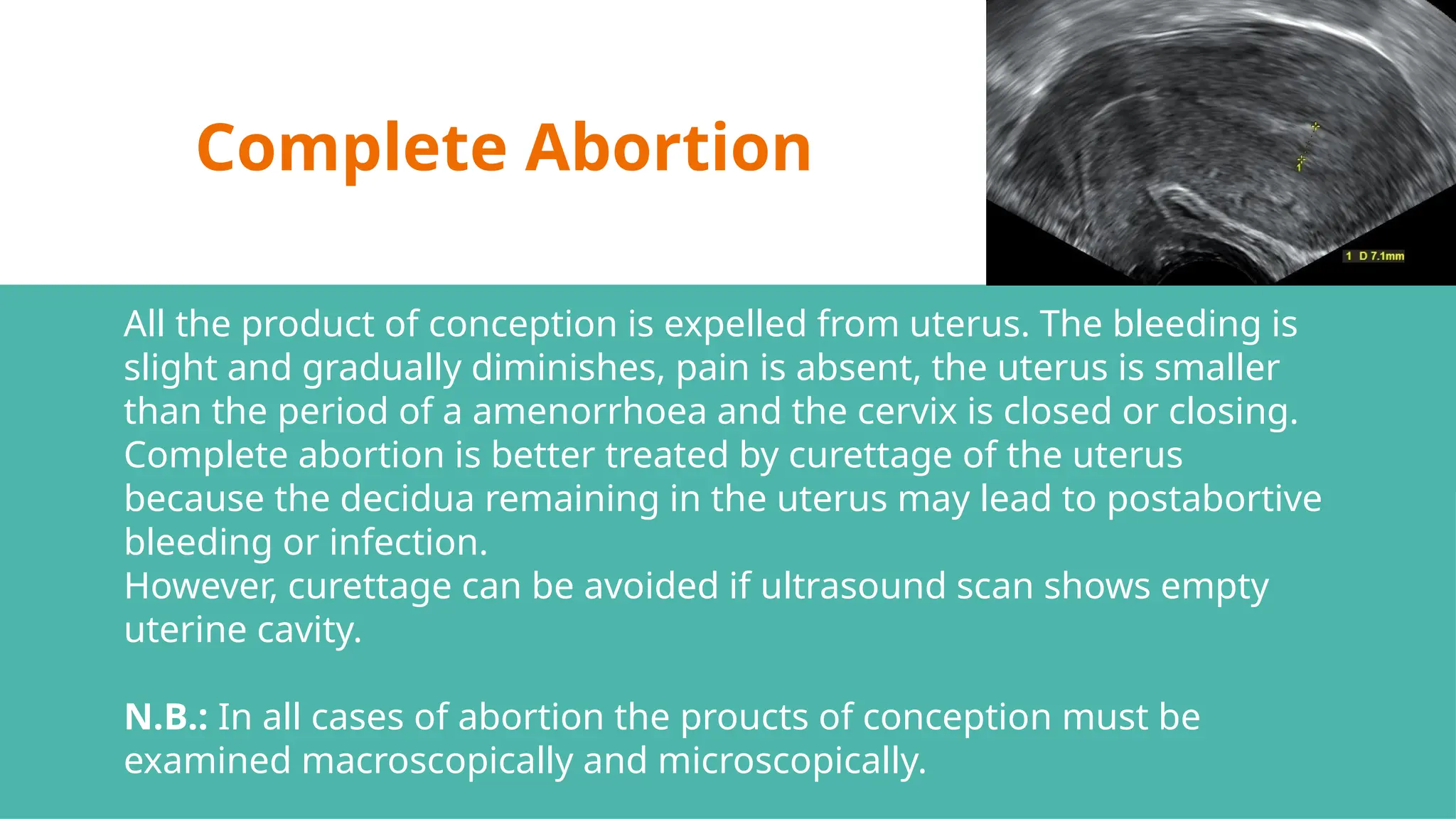
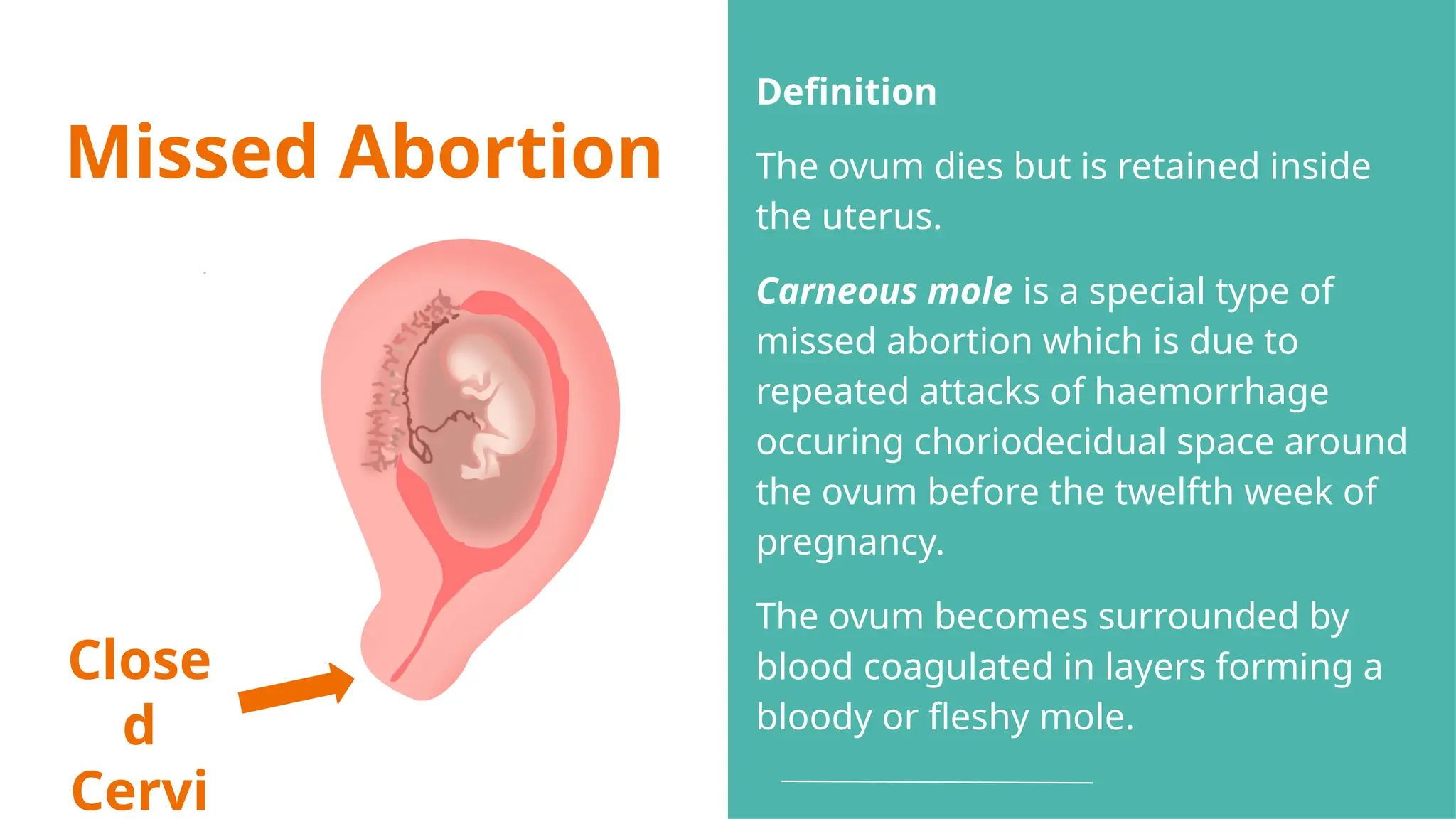
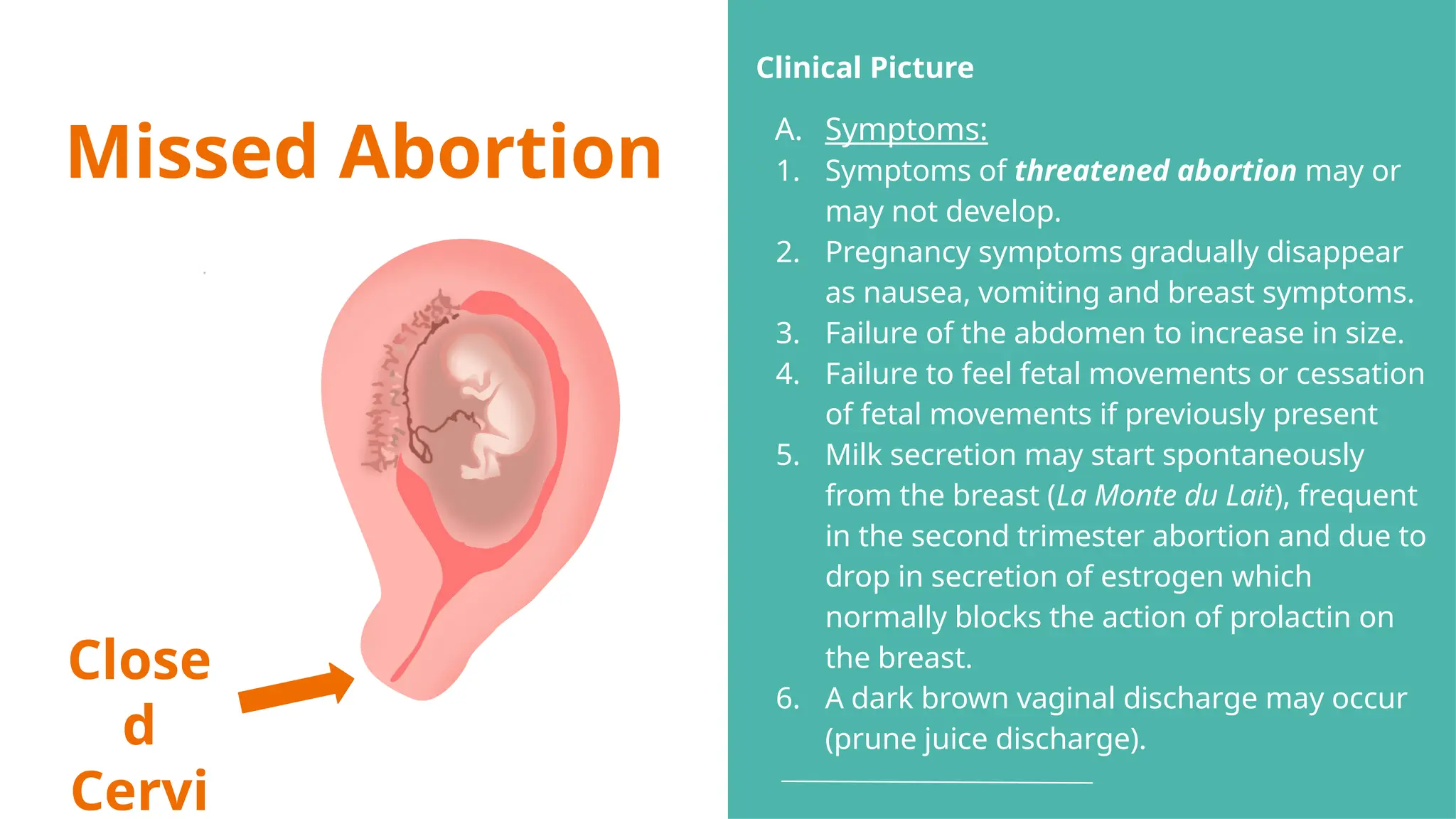
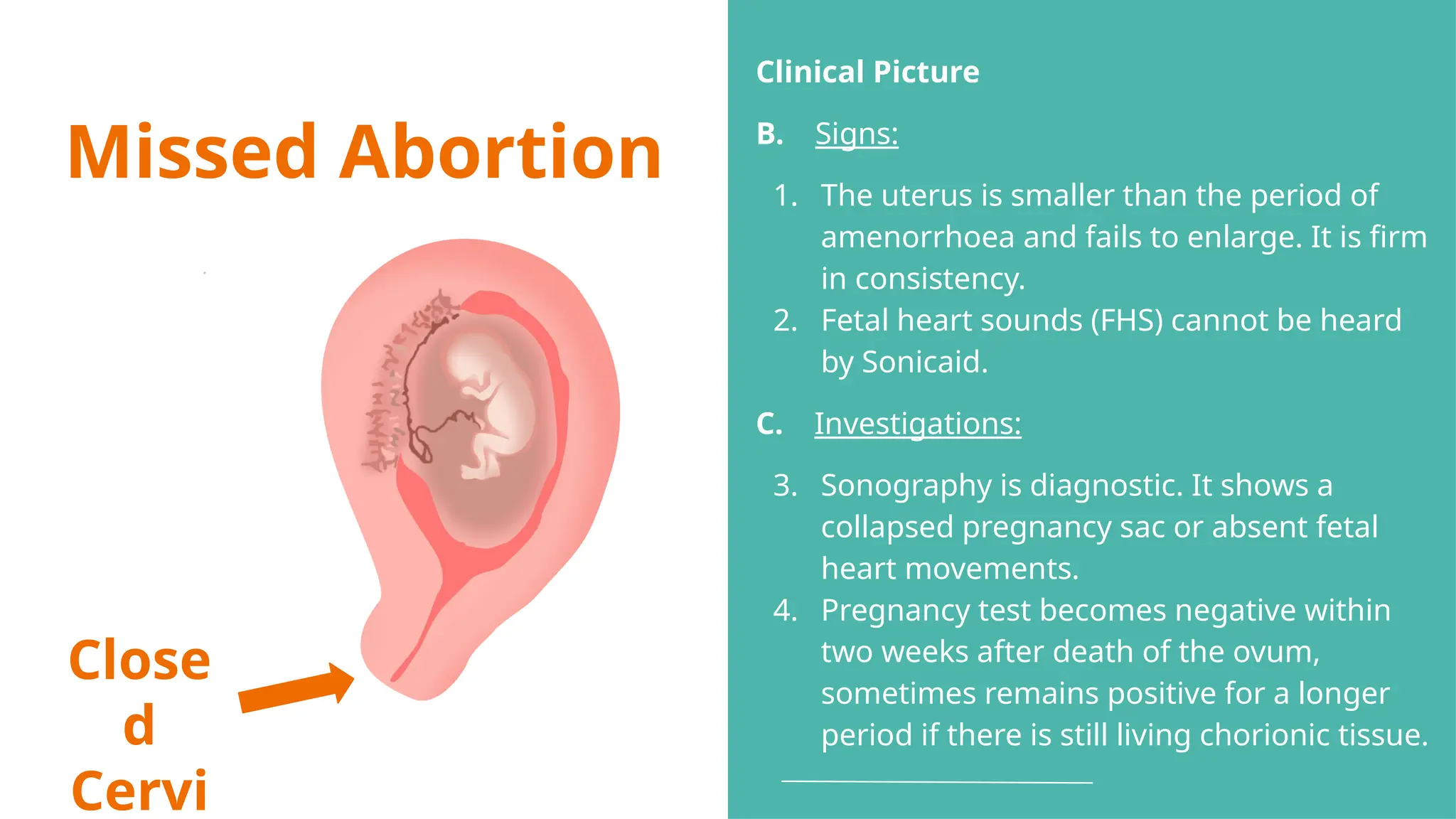
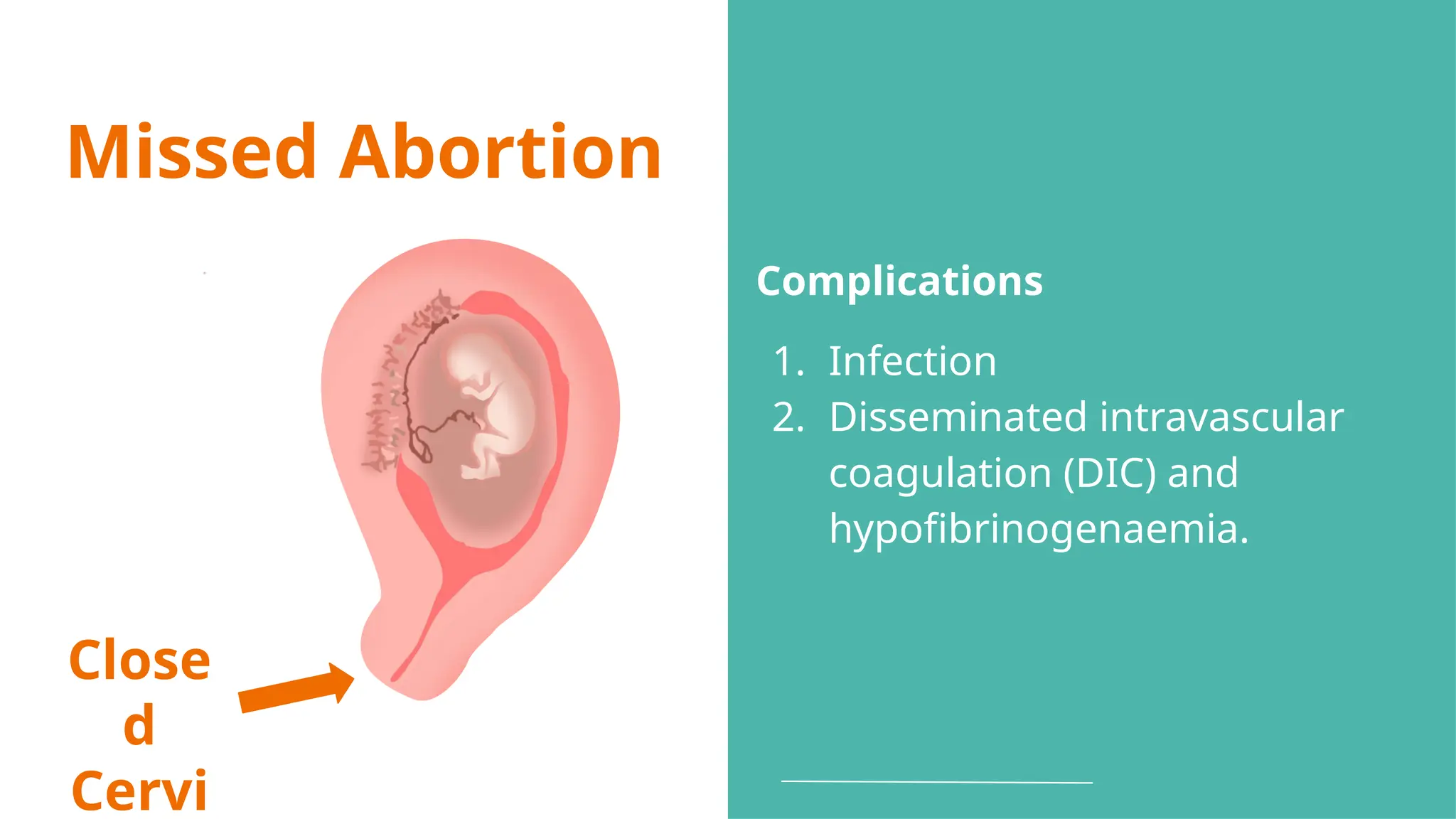
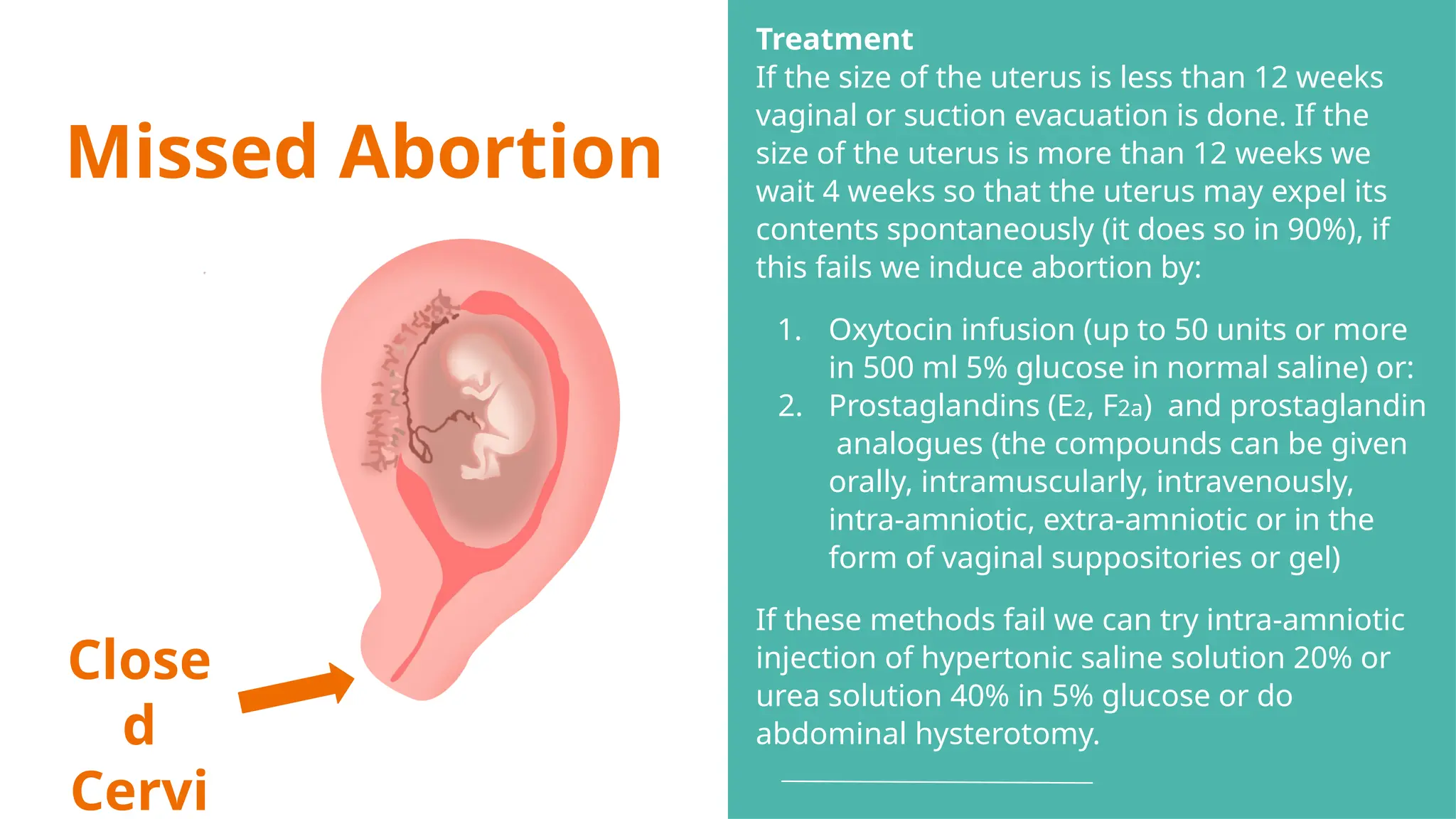
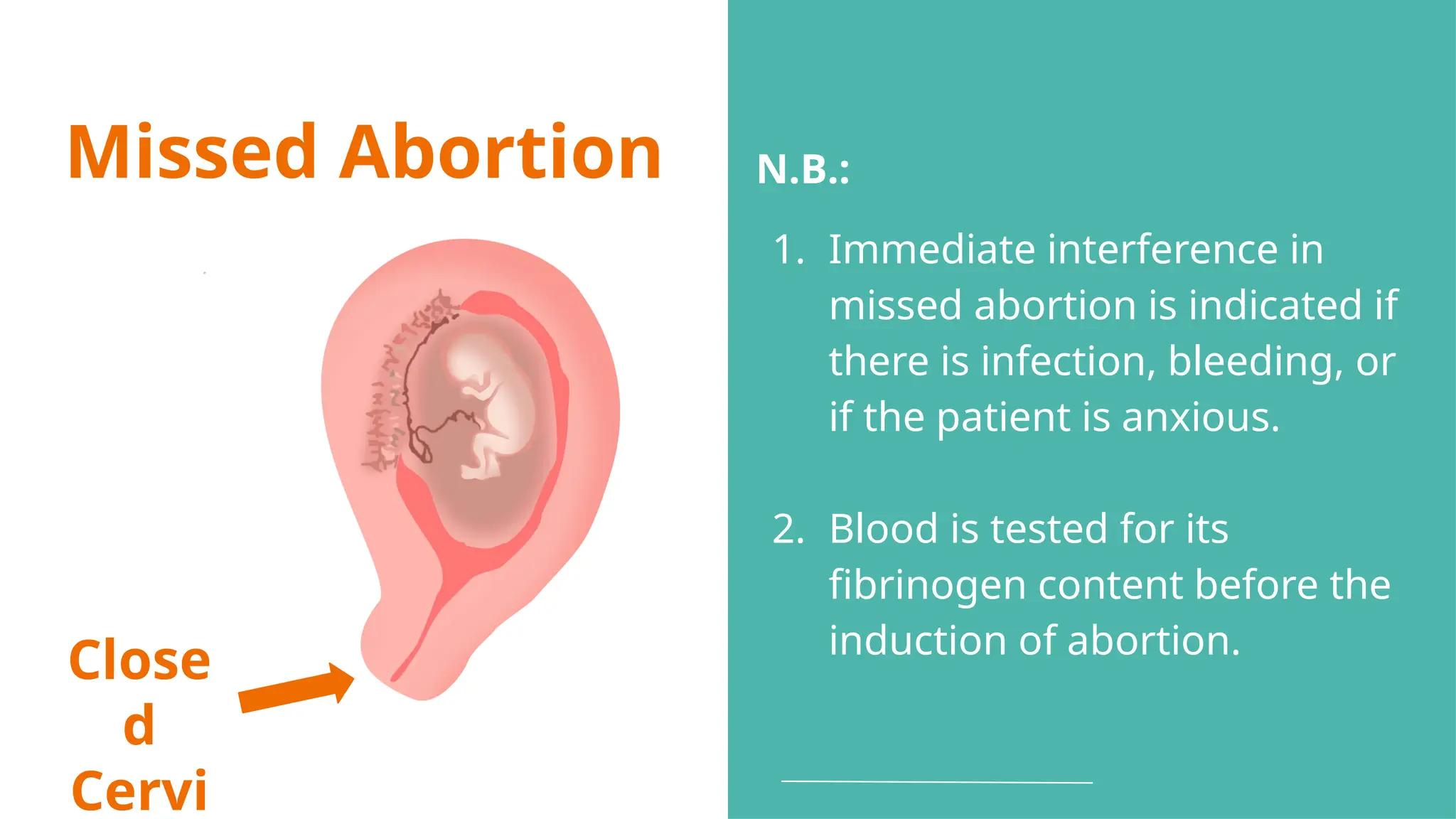
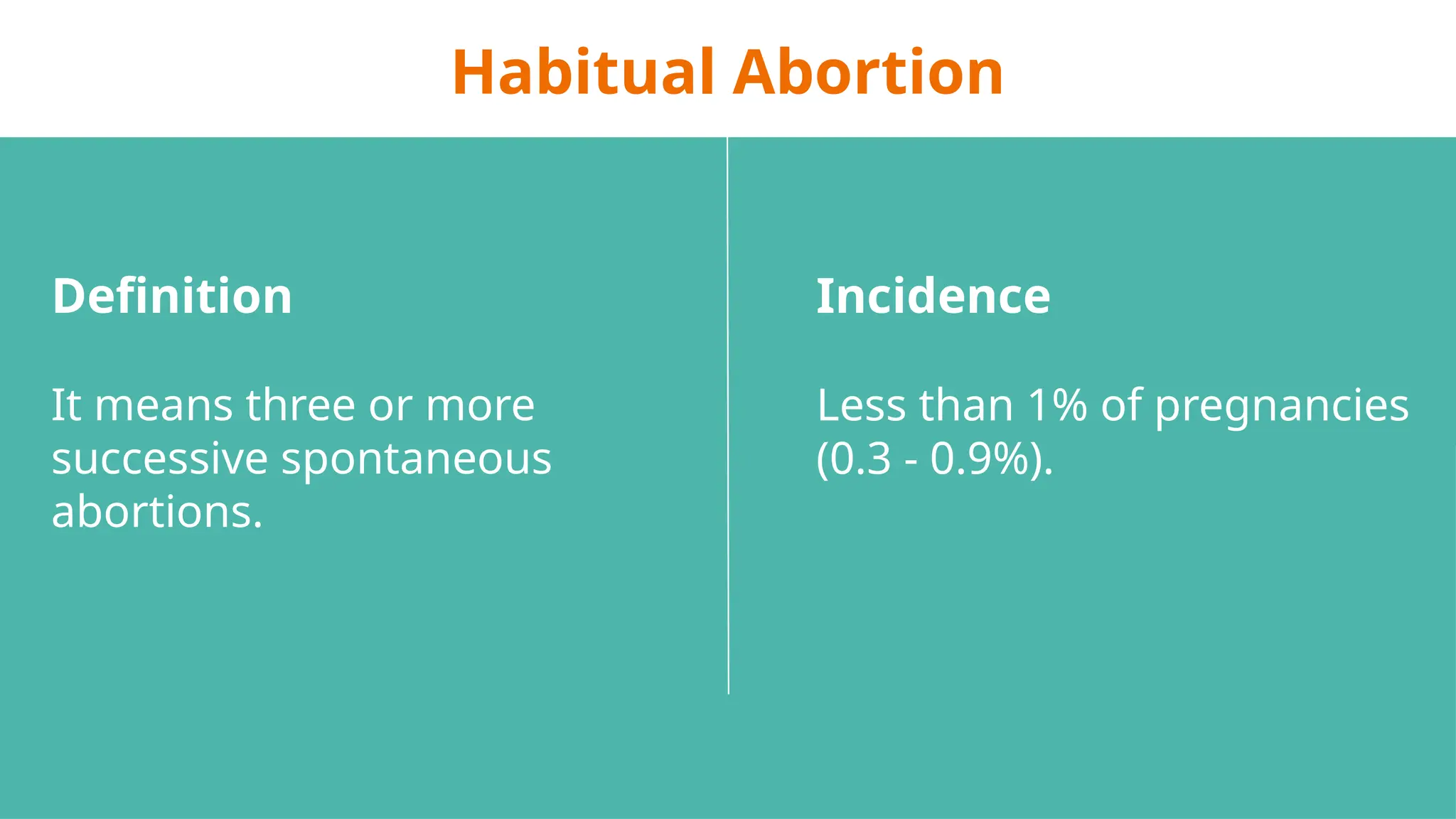
The document provides a comprehensive overview of abortion, including its definitions, types, causes, clinical presentations, and treatments. It discusses various forms of abortion, such as threatened, inevitable, and missed abortions, along with their respective symptoms and treatment options. The document also addresses complications arising from abortions, such as infections and habitual abortion, while referencing a medical text for further information.