1) Inflammation is the body's response to injury and involves redness, swelling, pain, warmth, and loss of function.
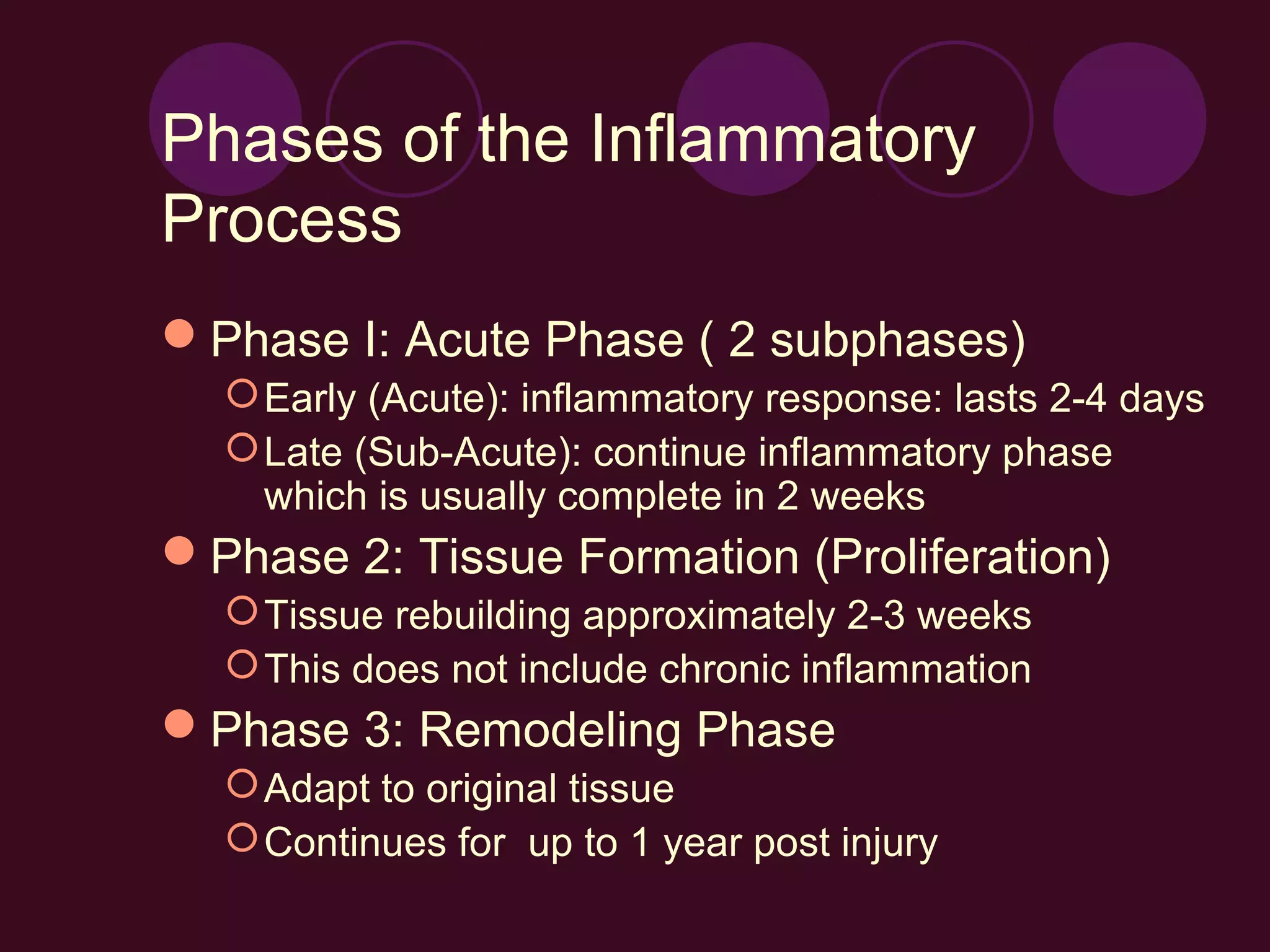
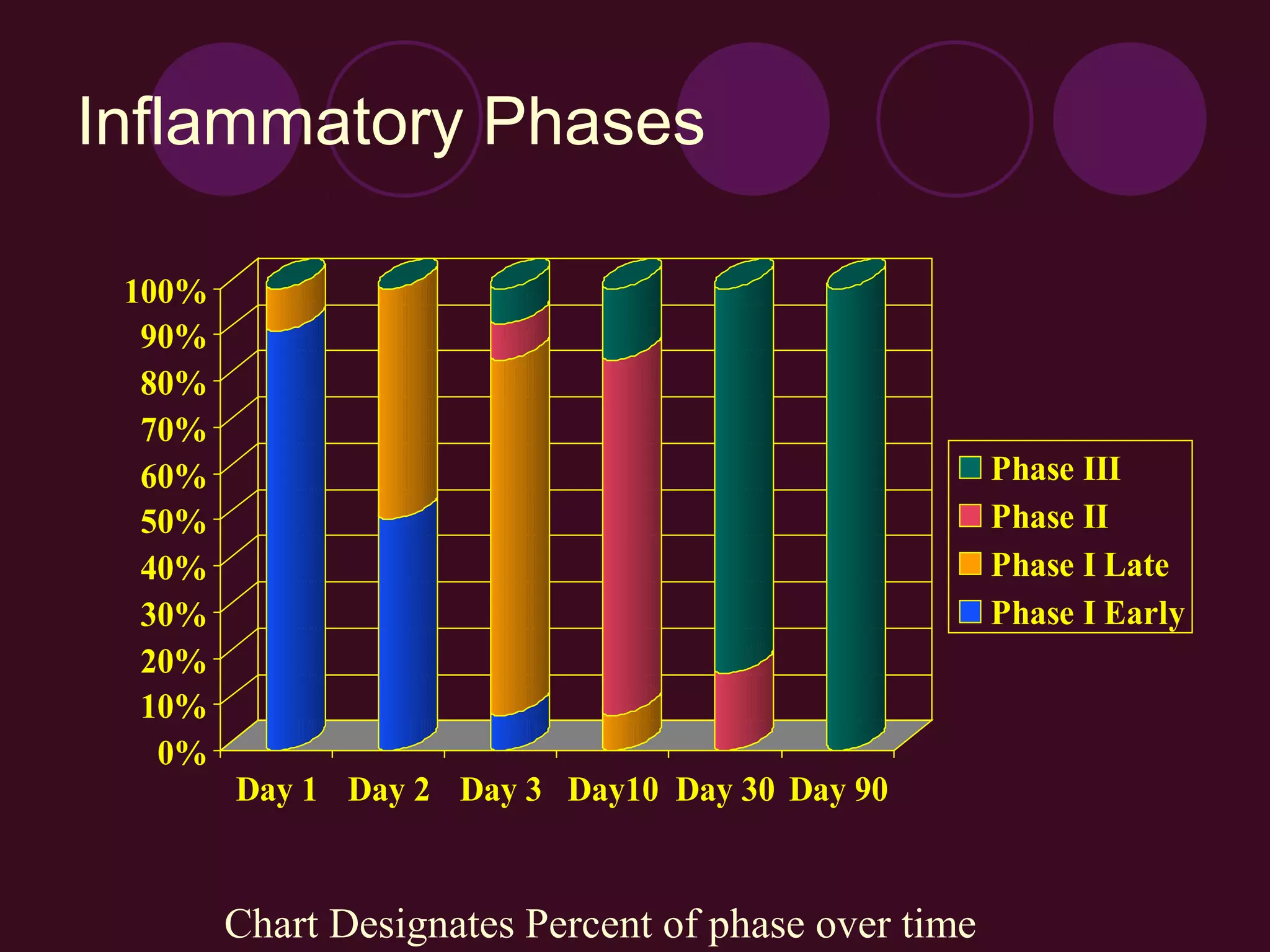
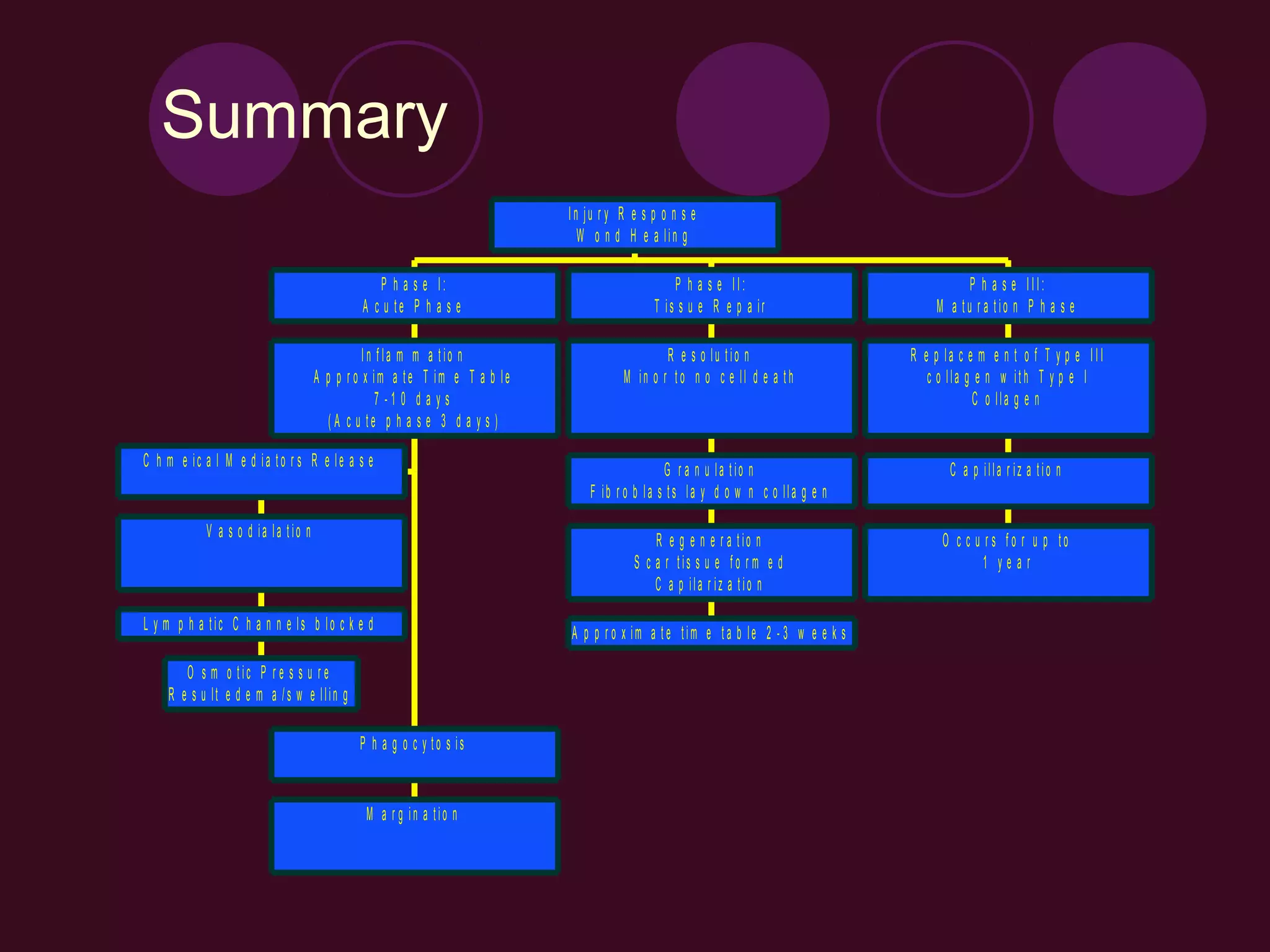
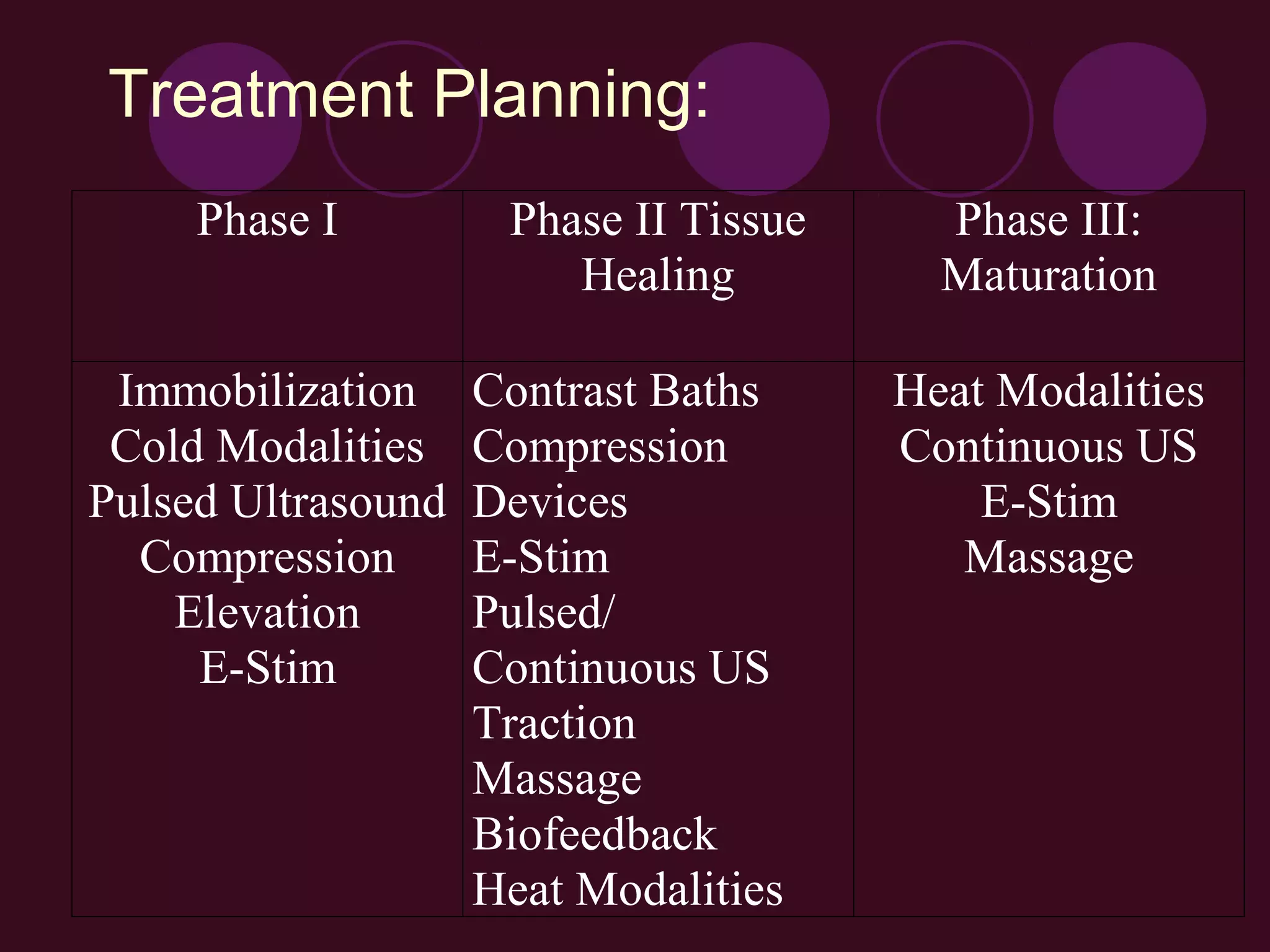
2) The inflammatory process has three phases - the acute/early phase aims to remove harmful stimuli and begin healing; the proliferation phase involves new tissue formation; and the remodeling phase adapts the new tissue.
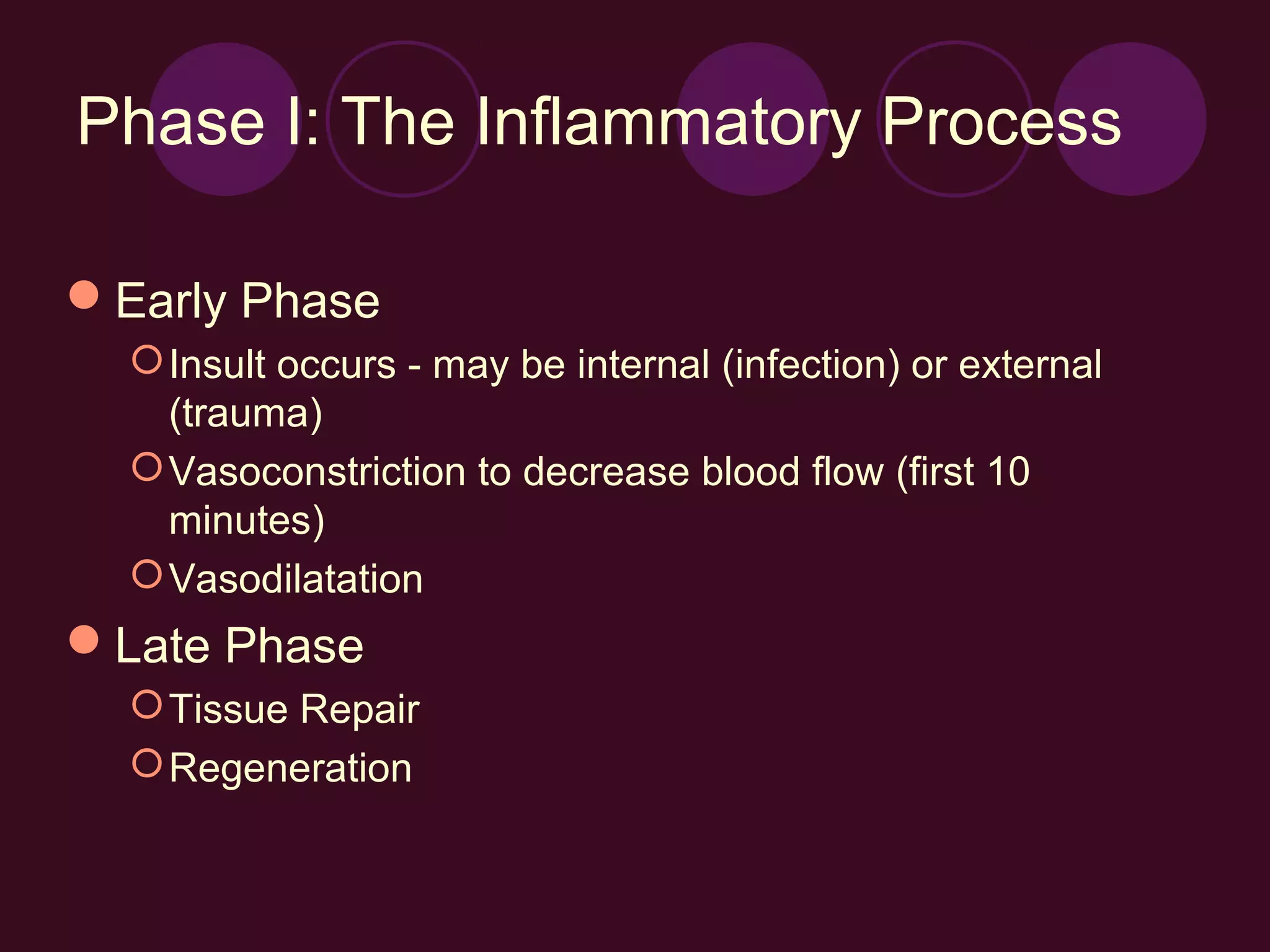
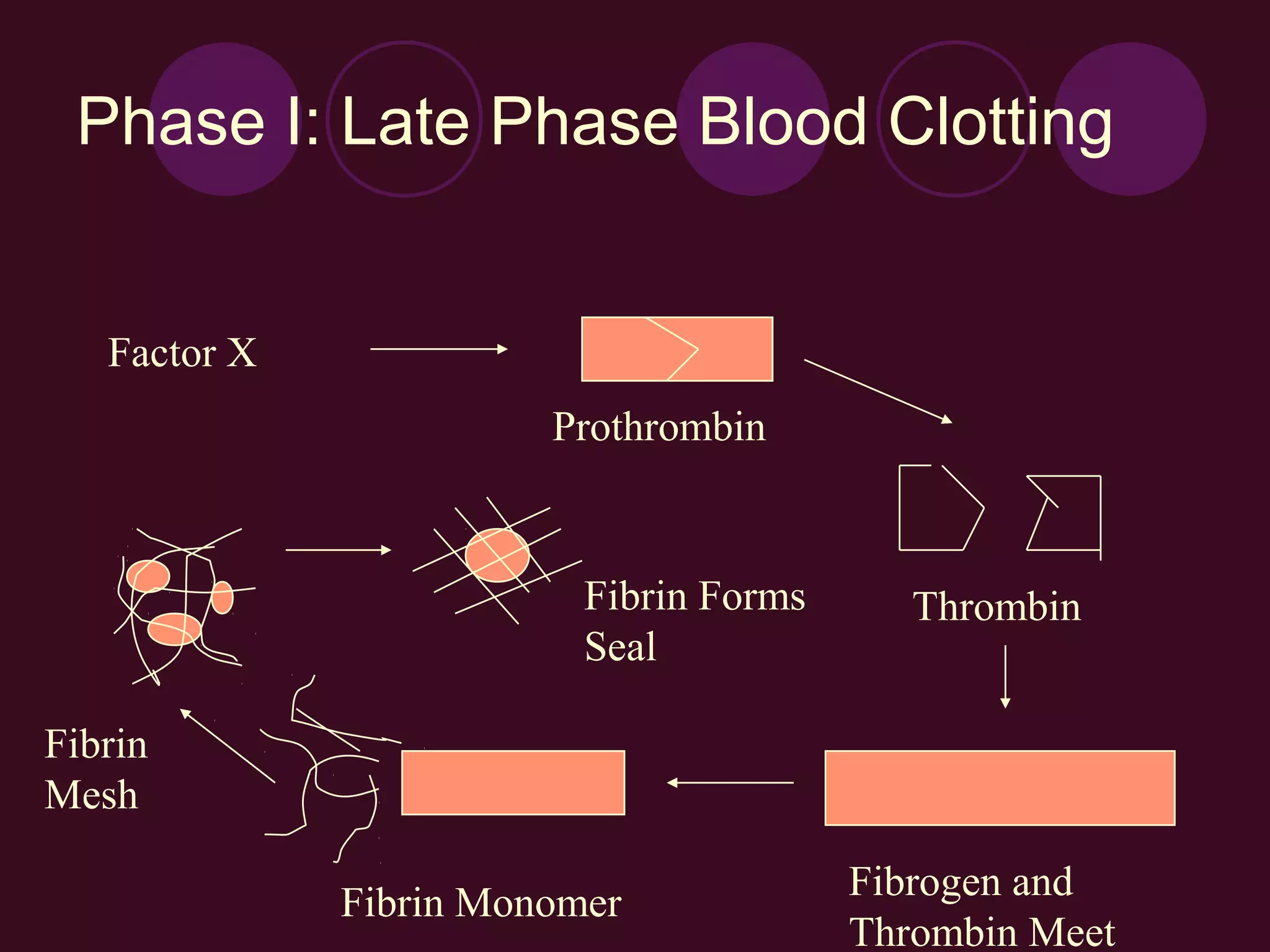
3) Key events in the early inflammatory phase include increased blood flow due to chemical mediators, fluid leakage causing swelling, and the arrival of white blood cells to remove debris.