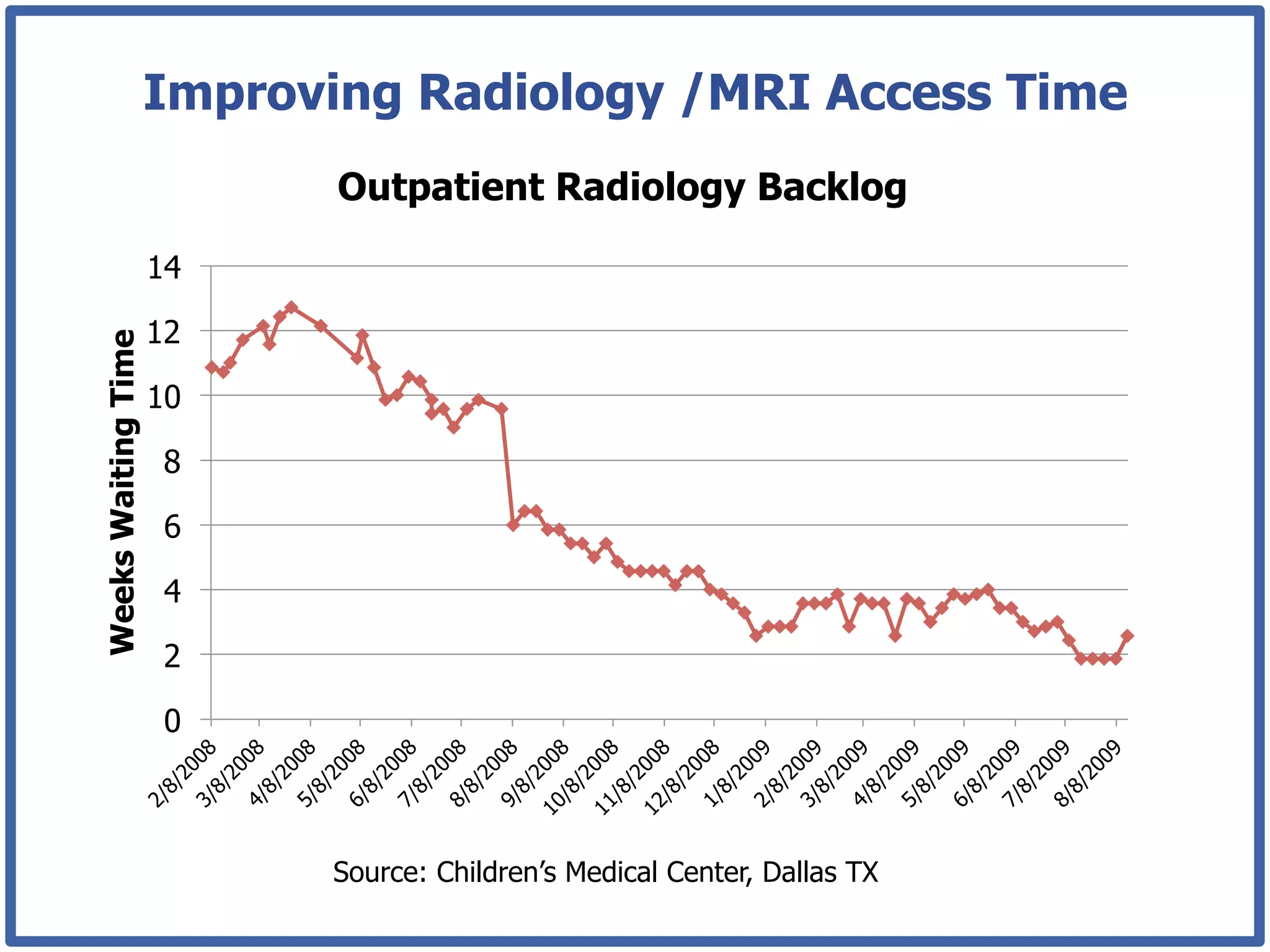
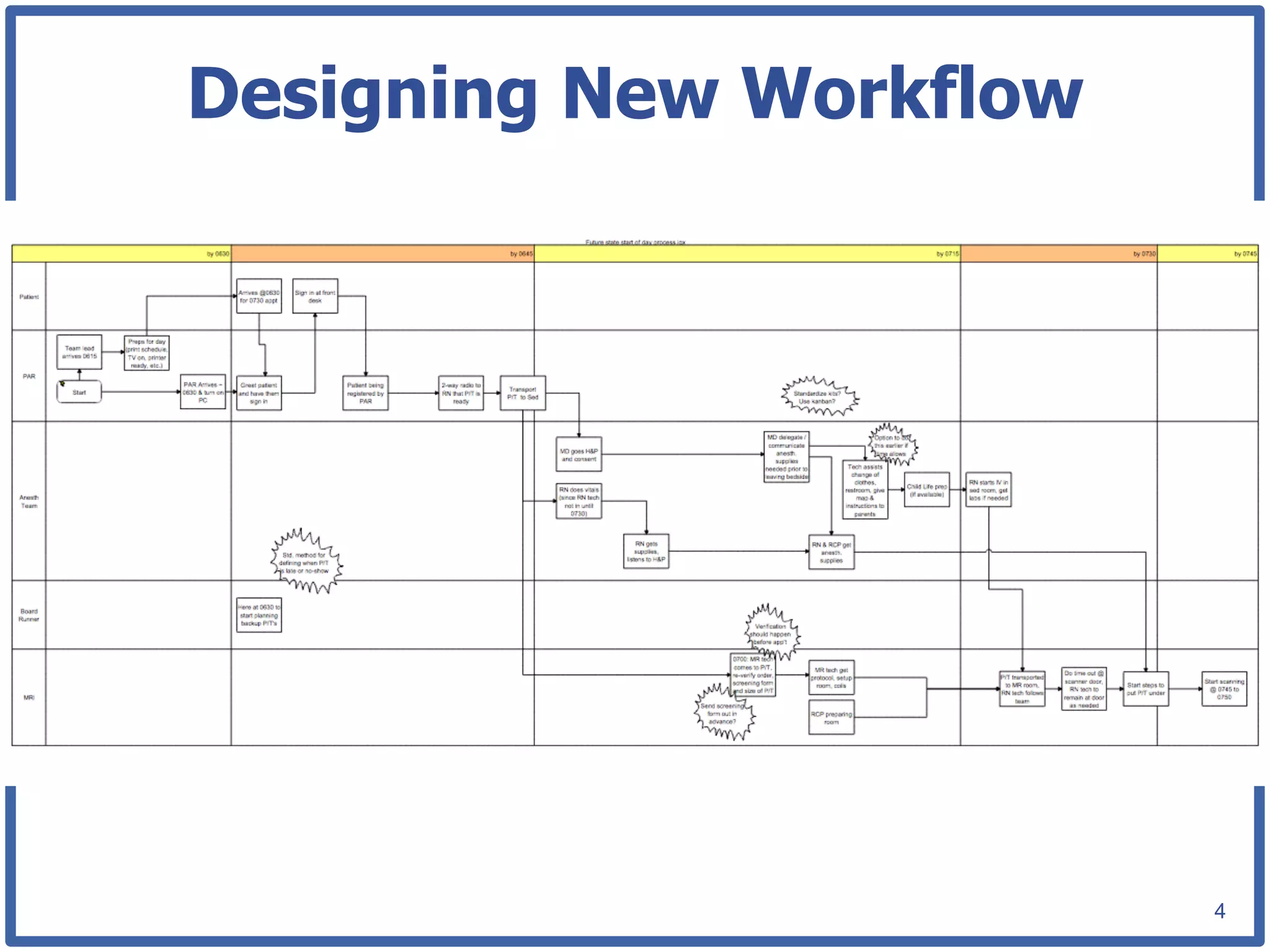
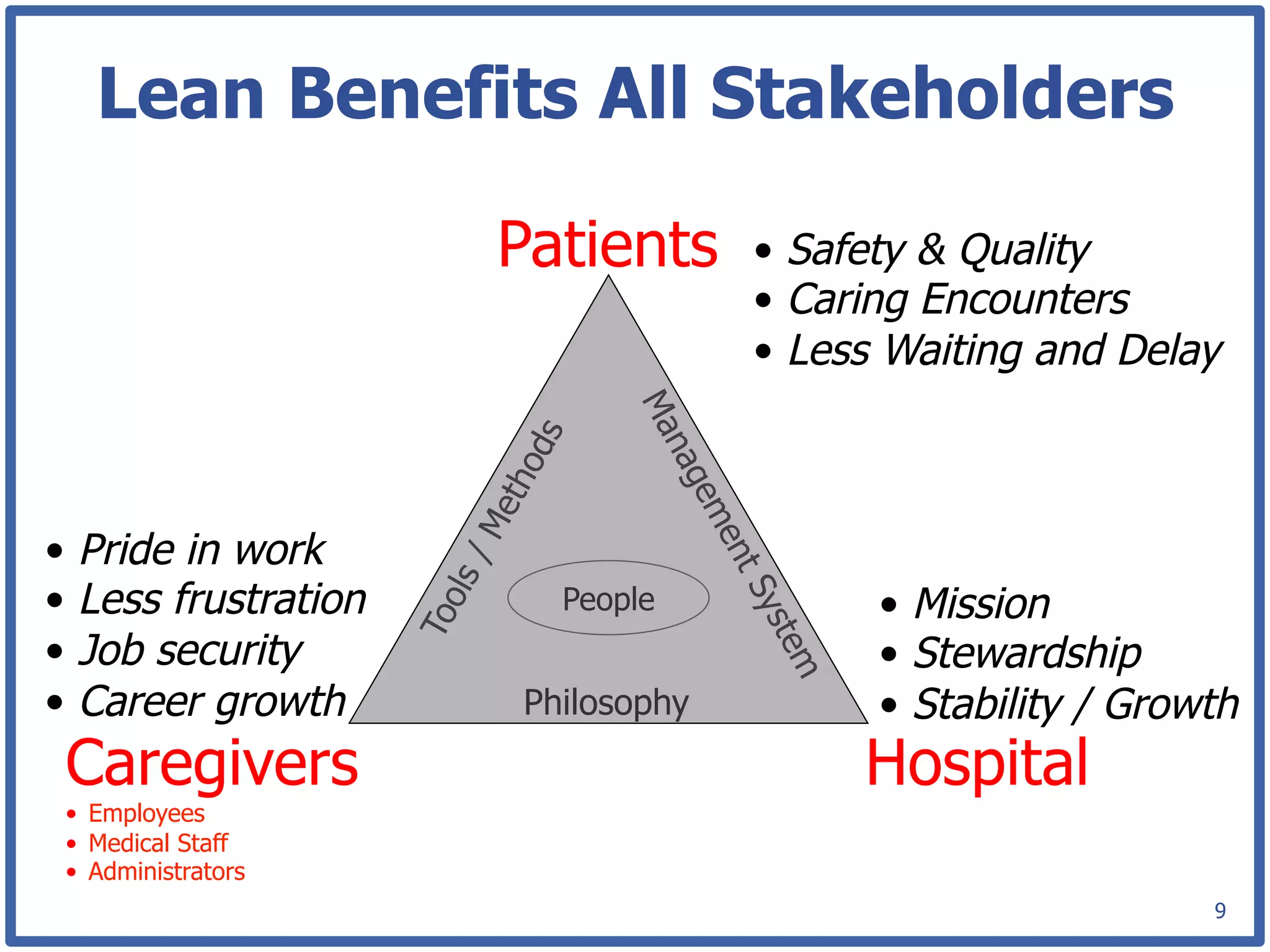
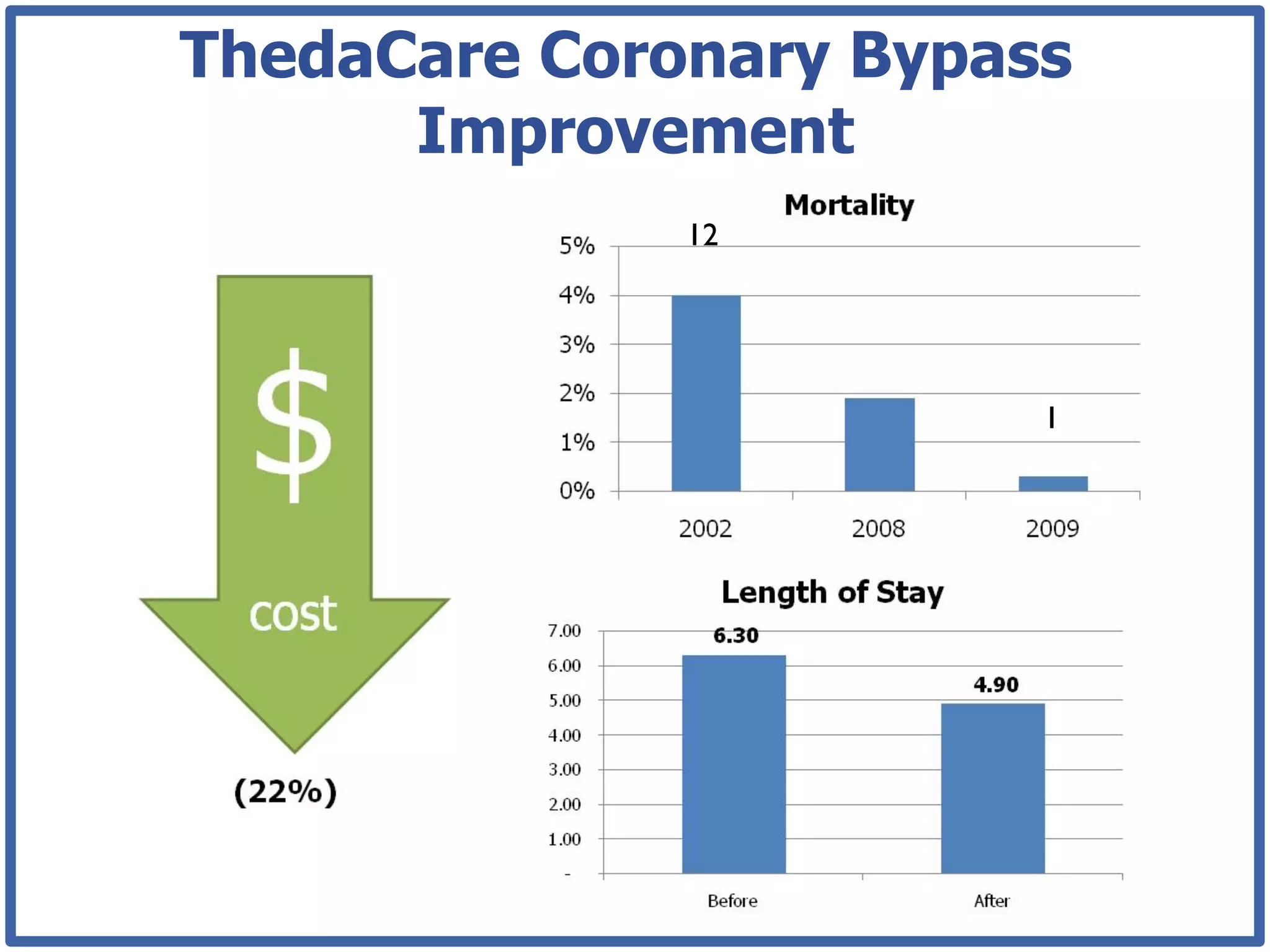
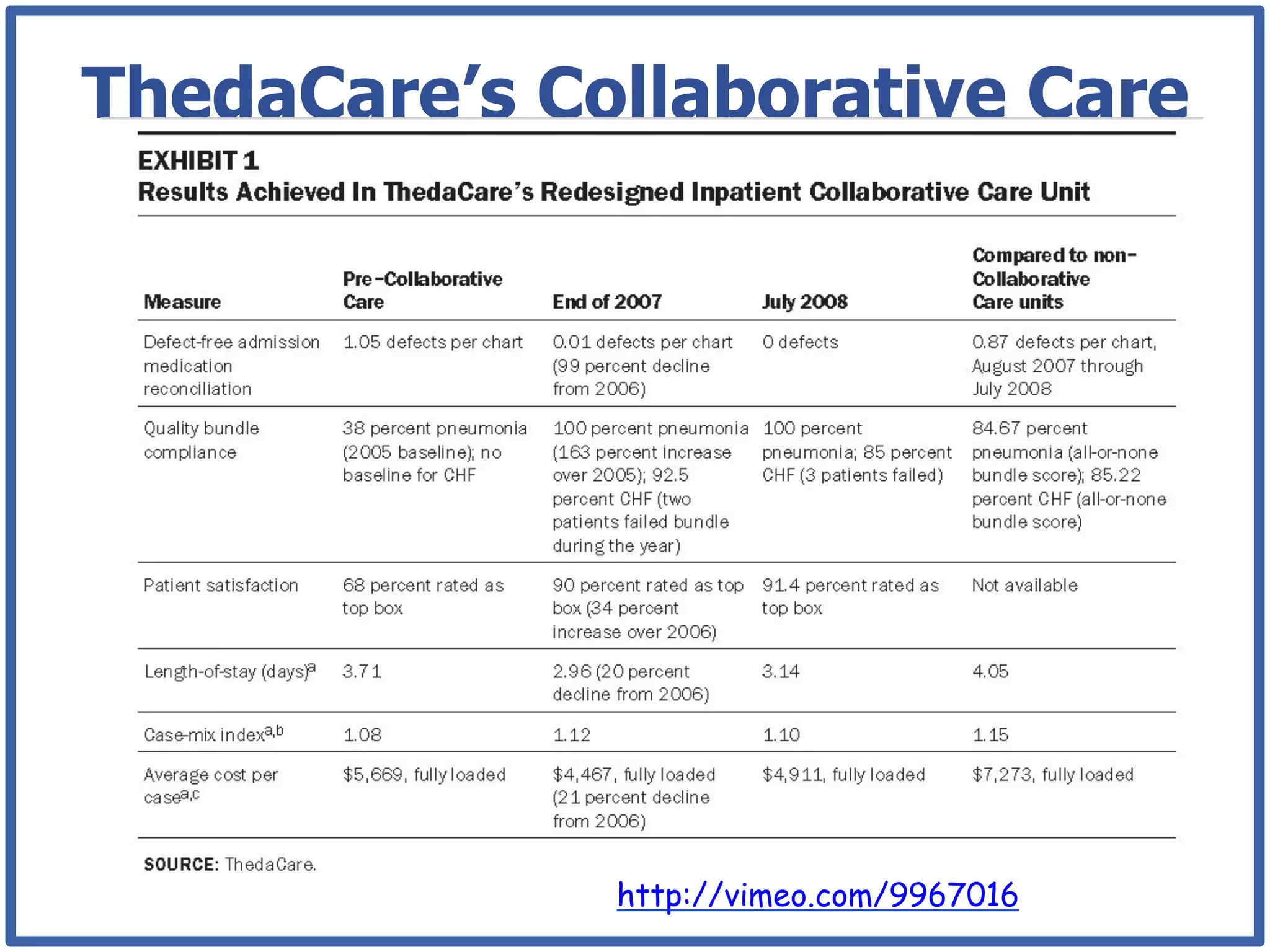
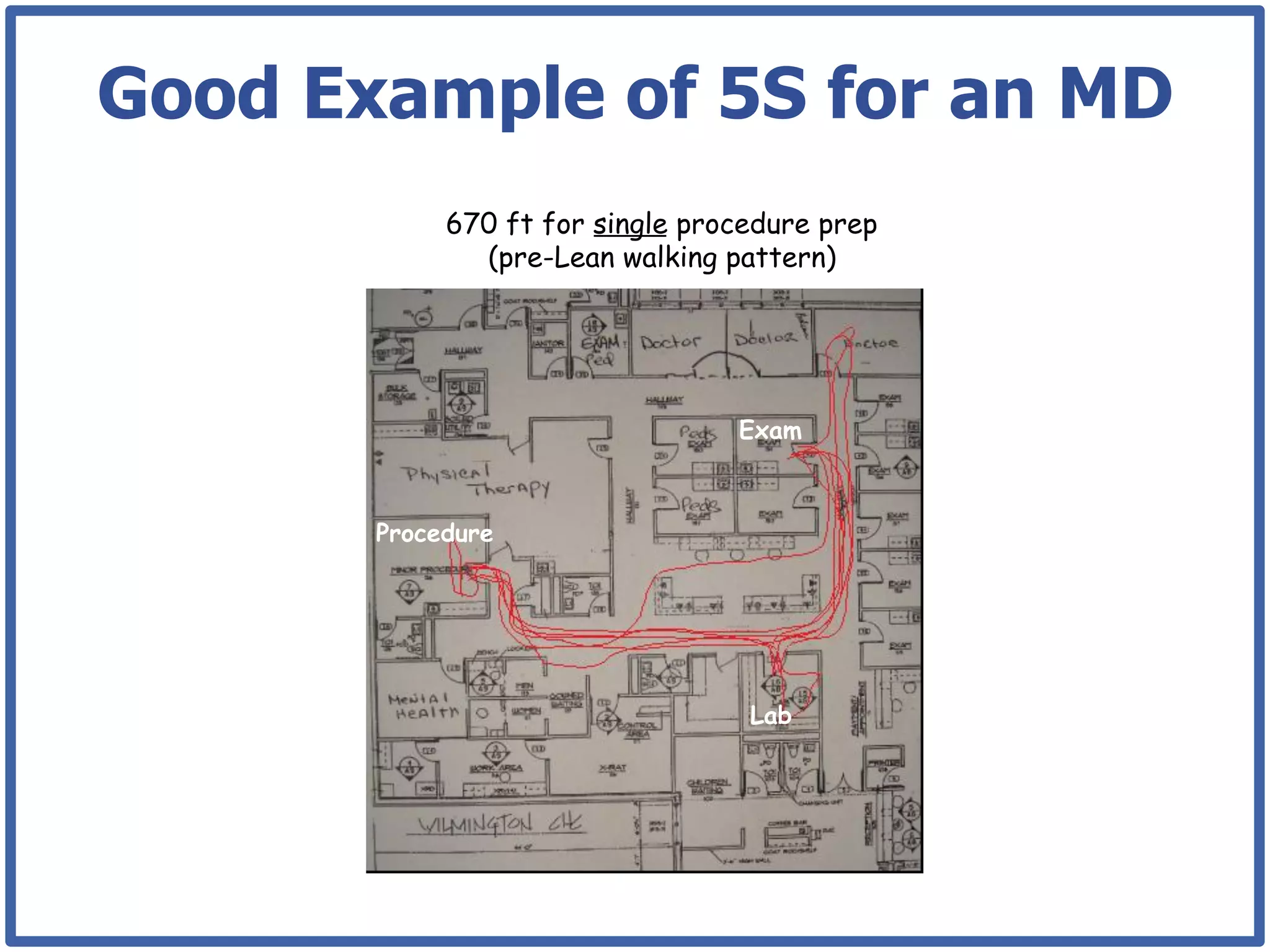
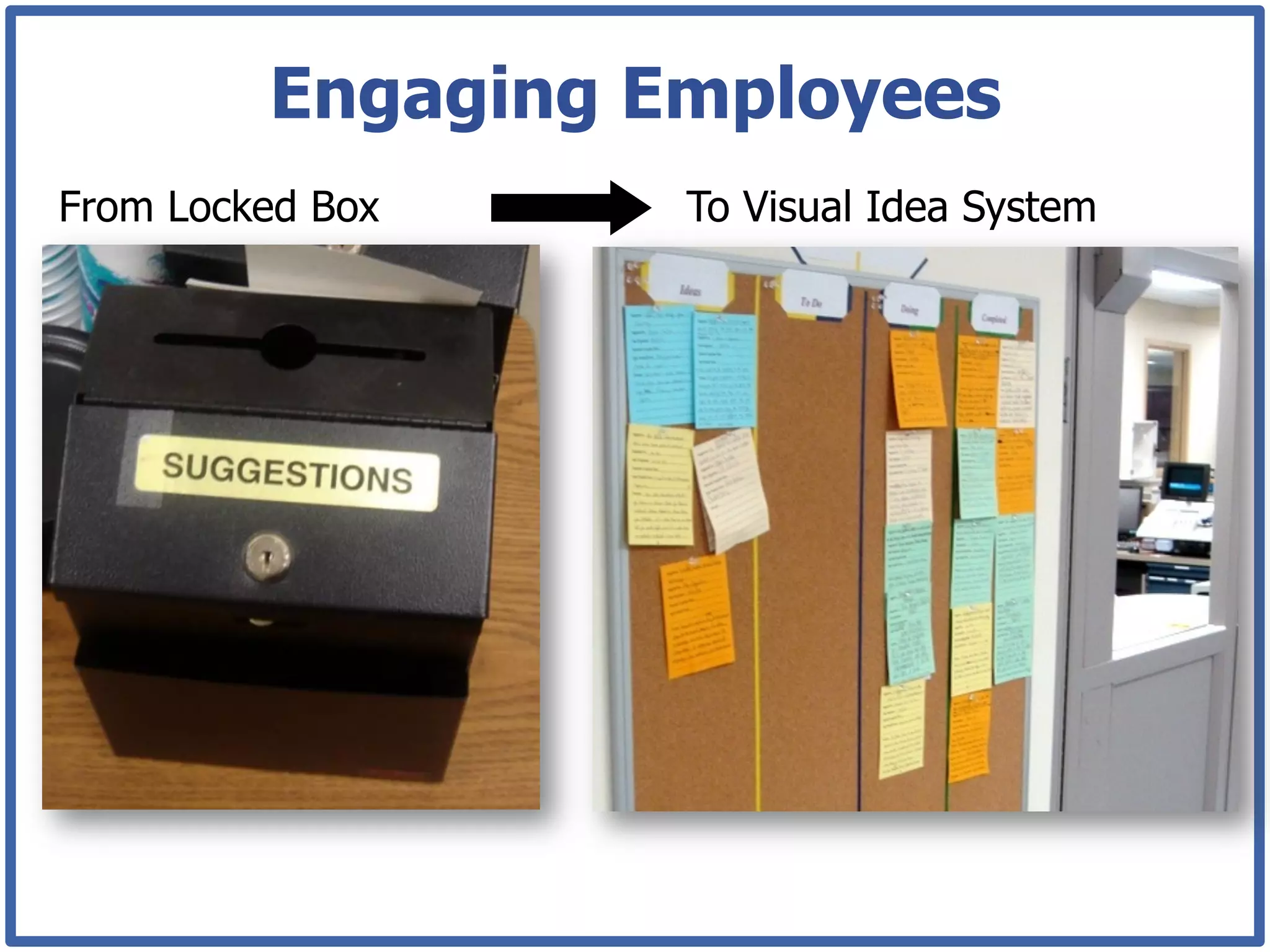
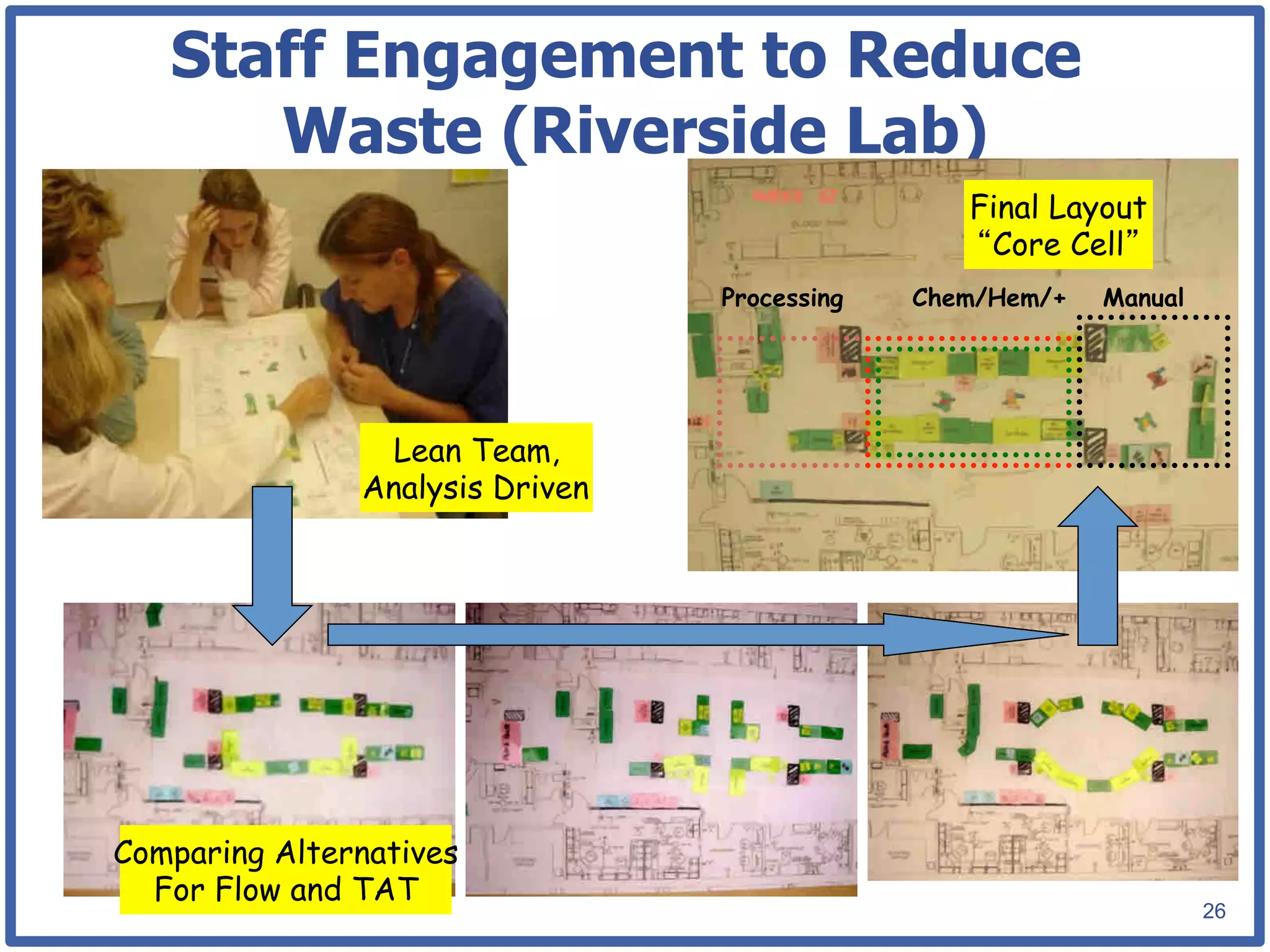
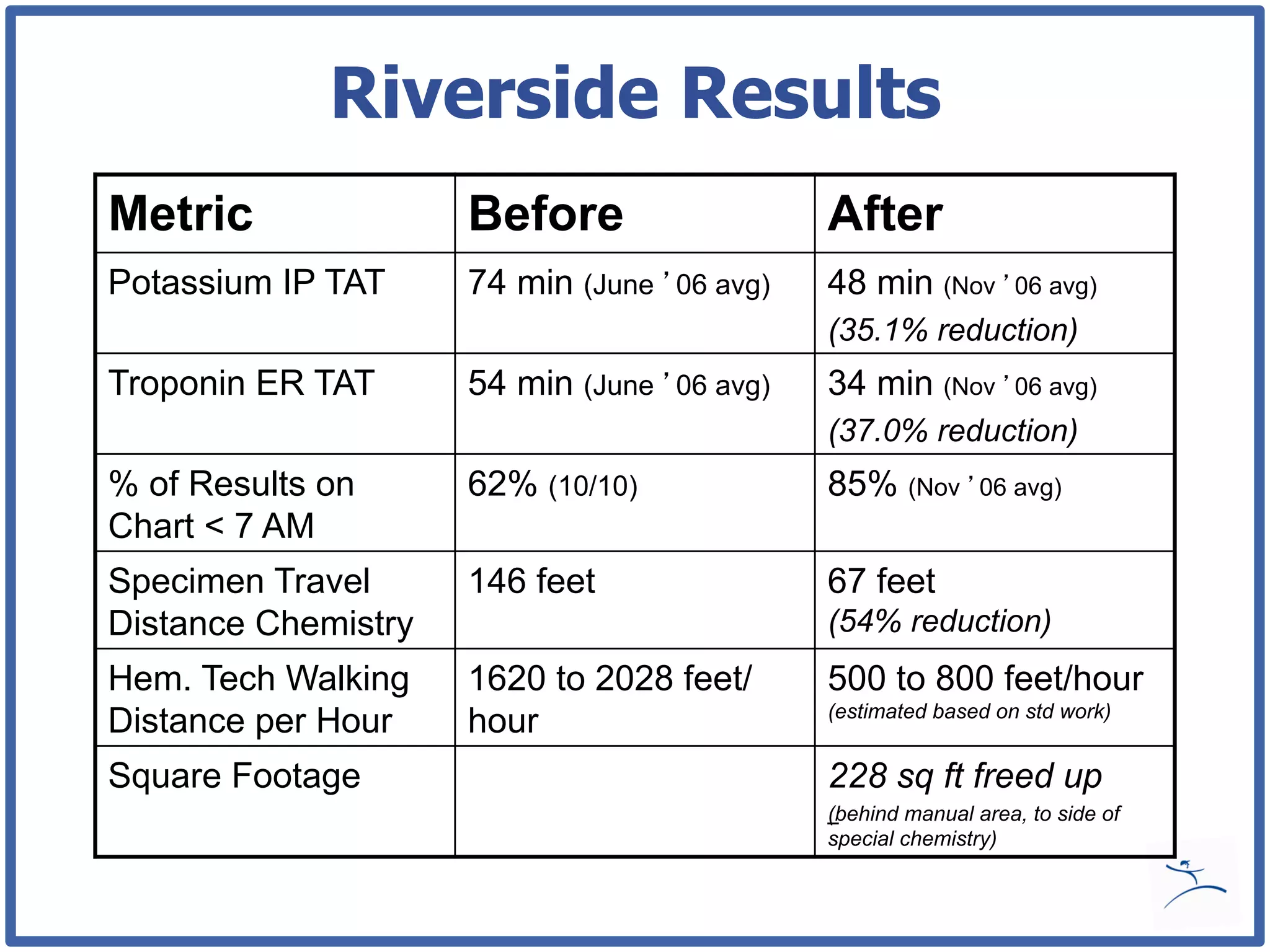
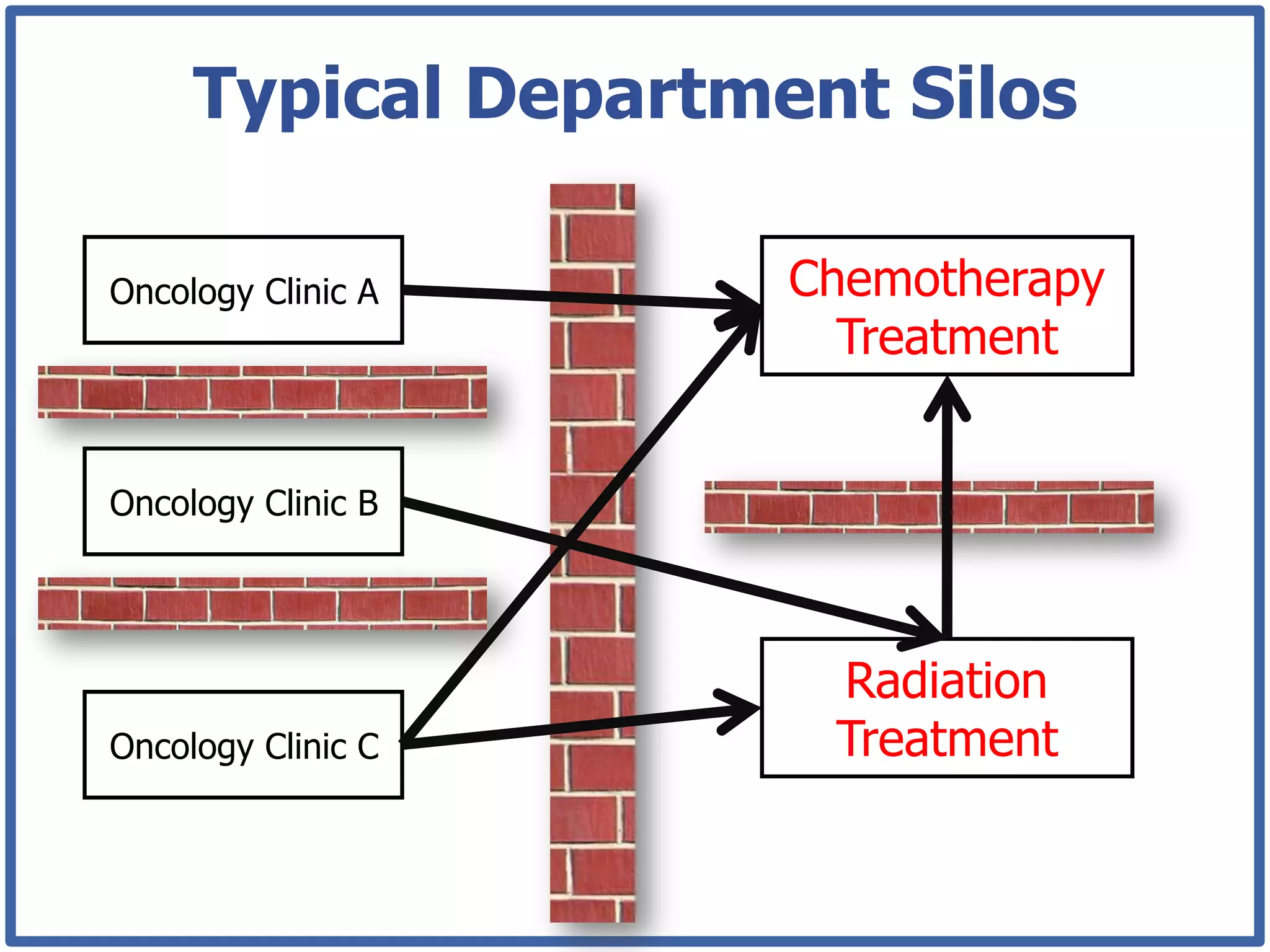
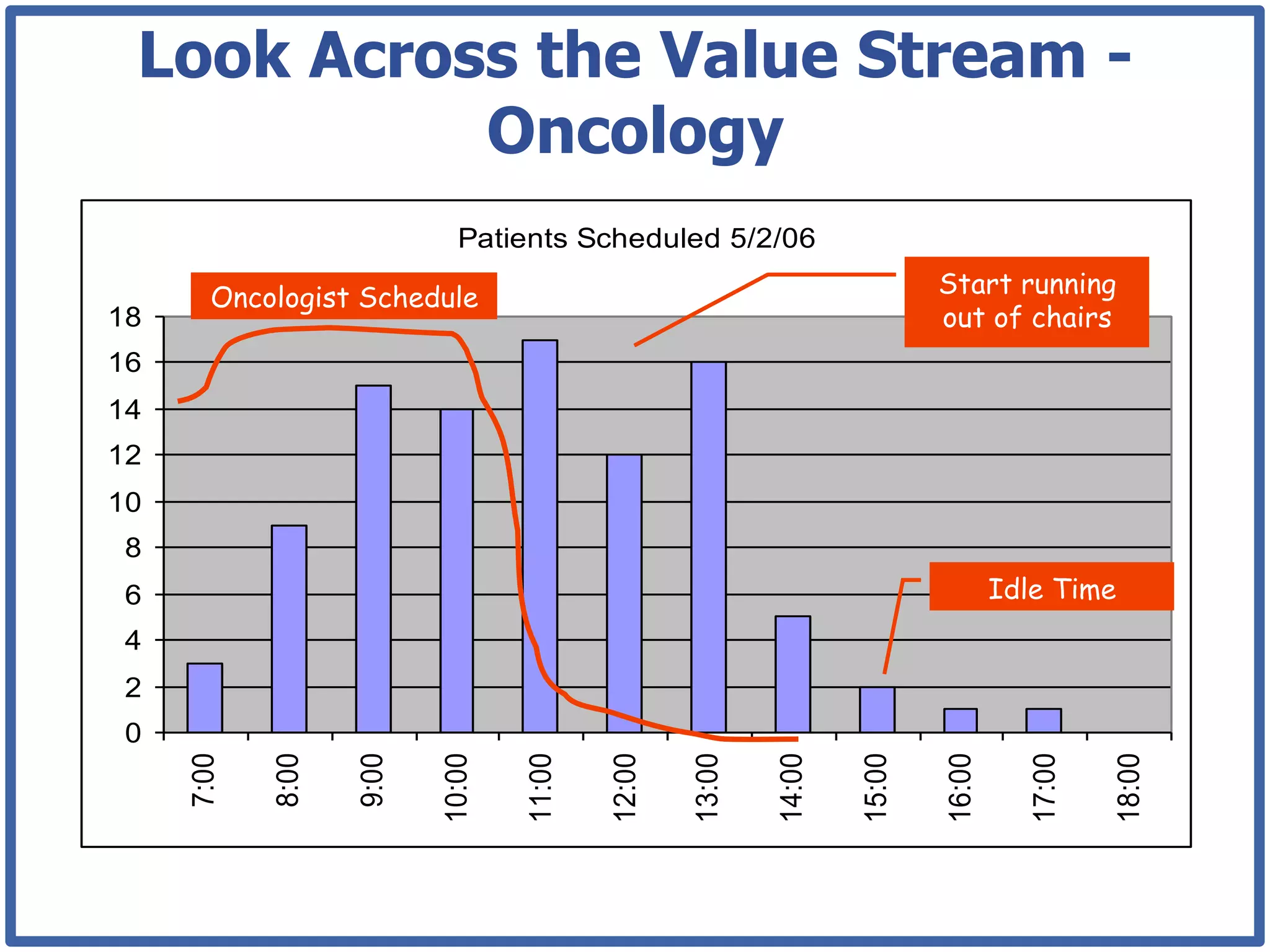
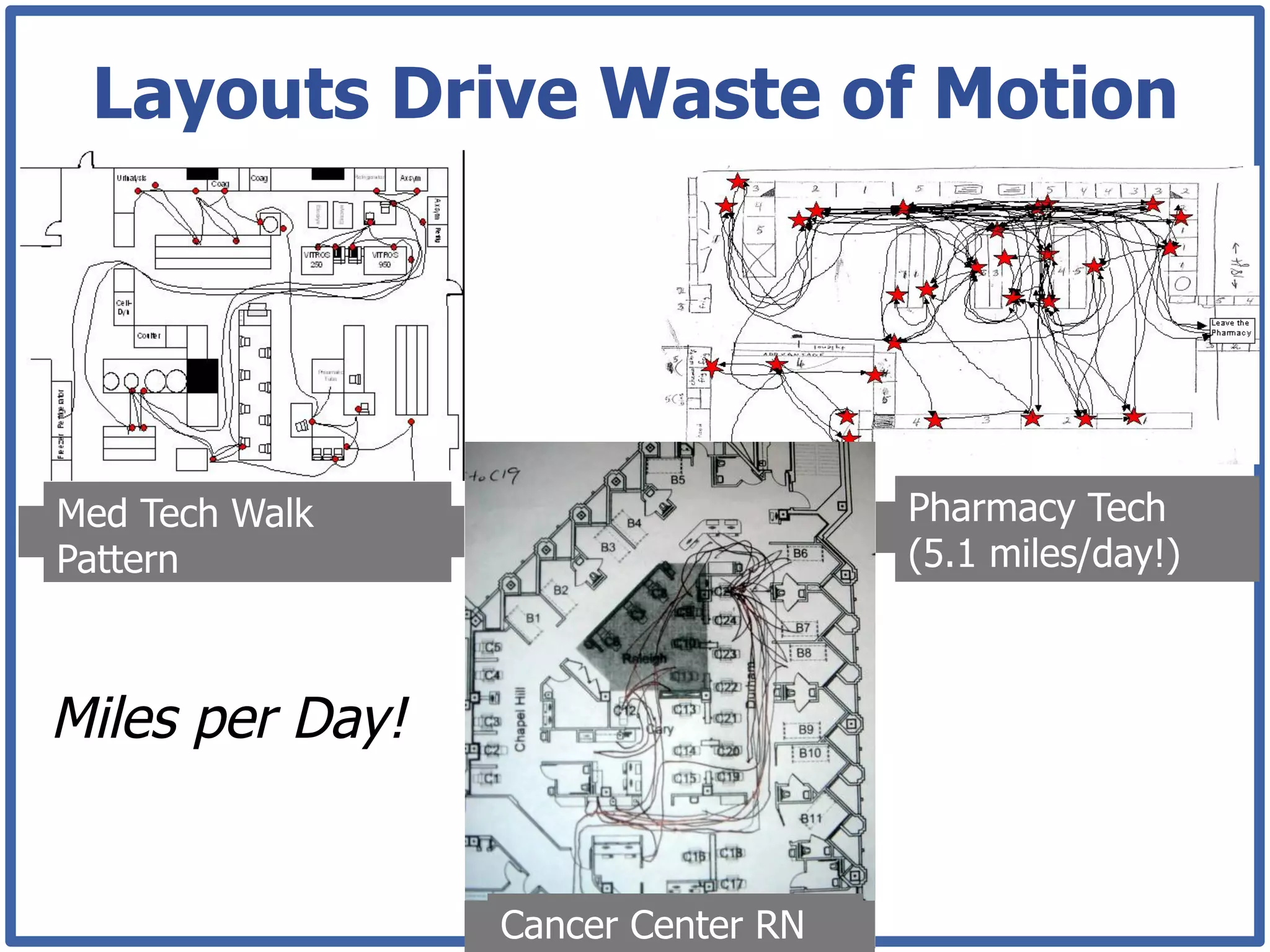
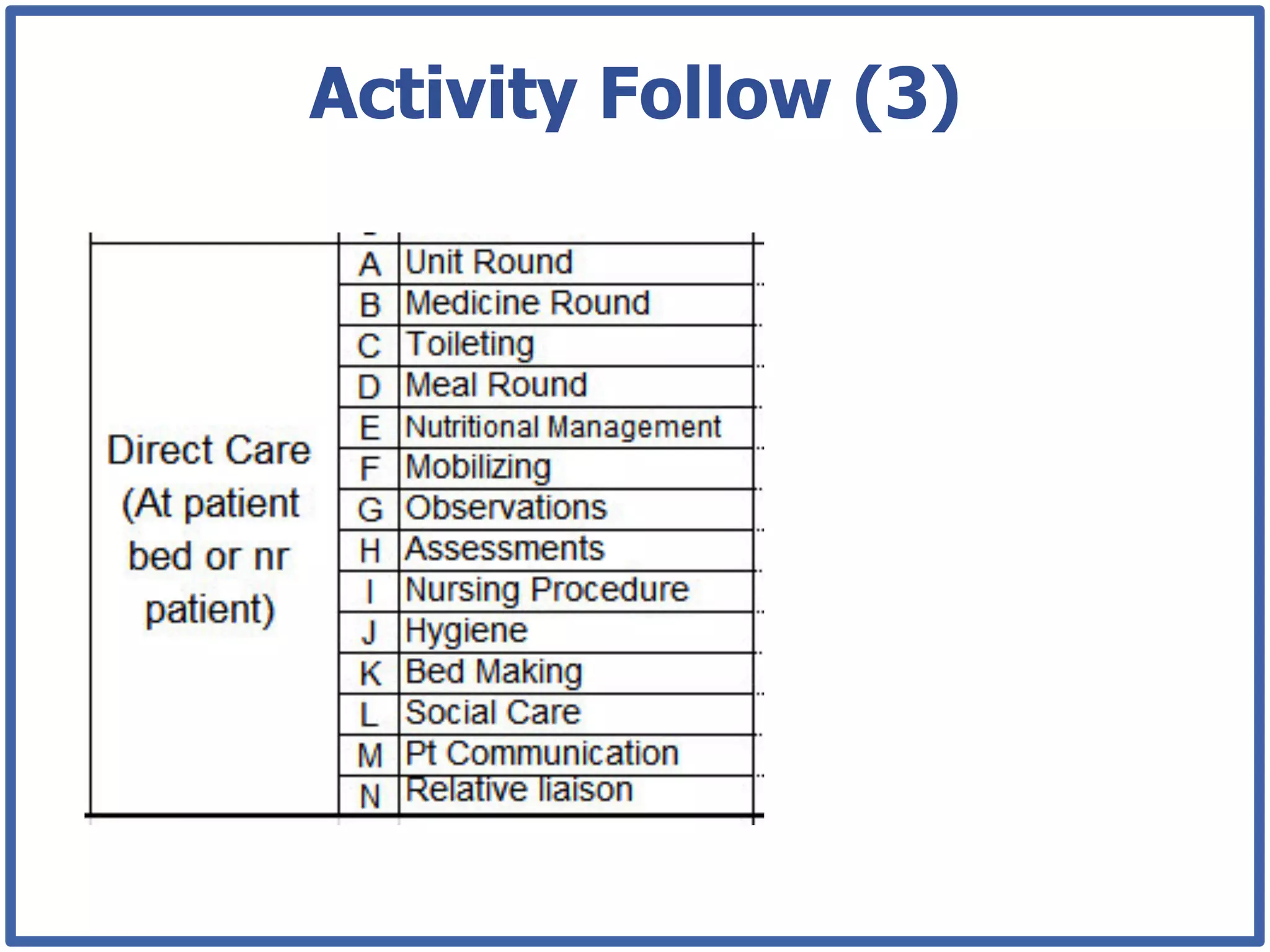
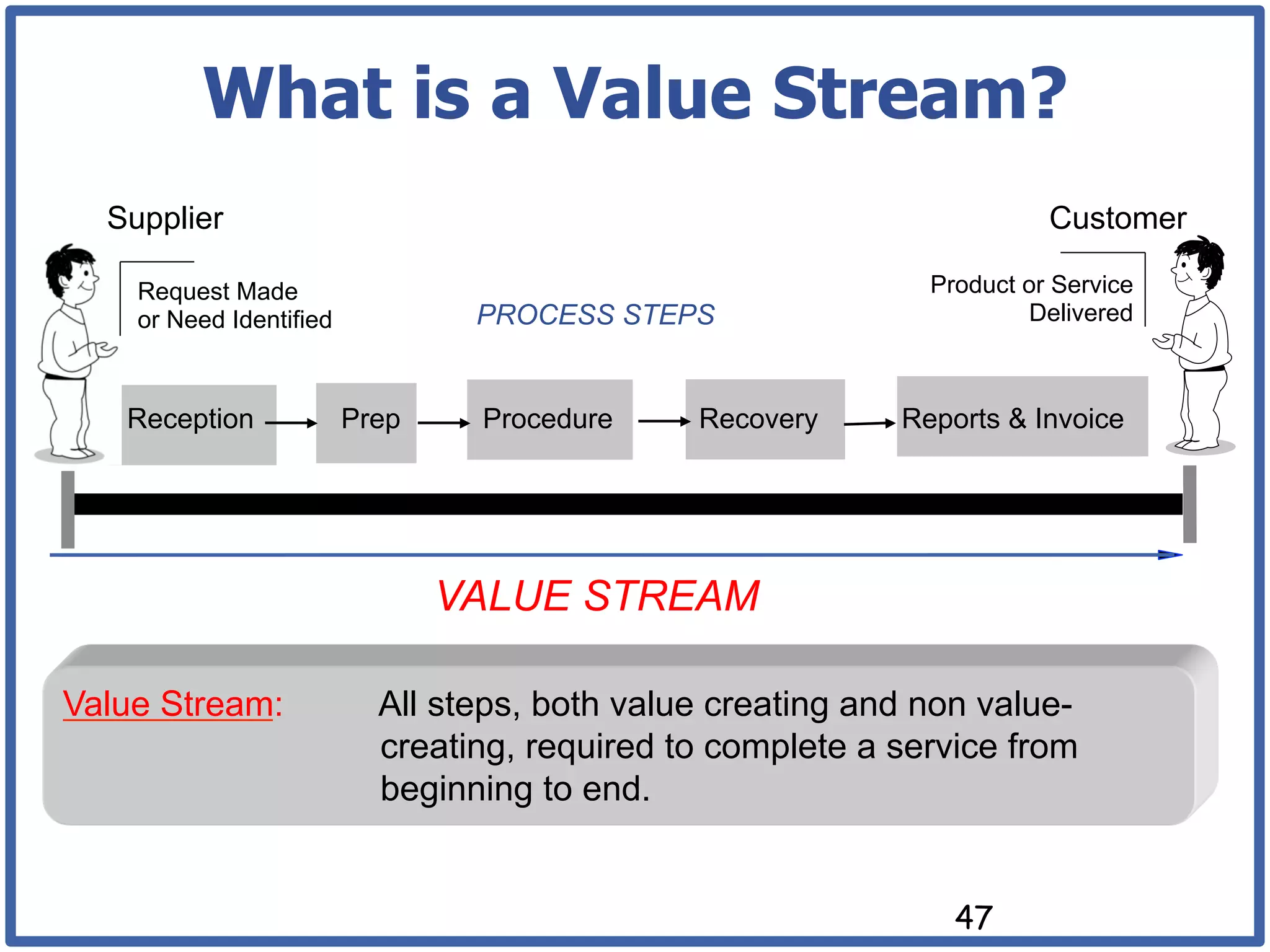
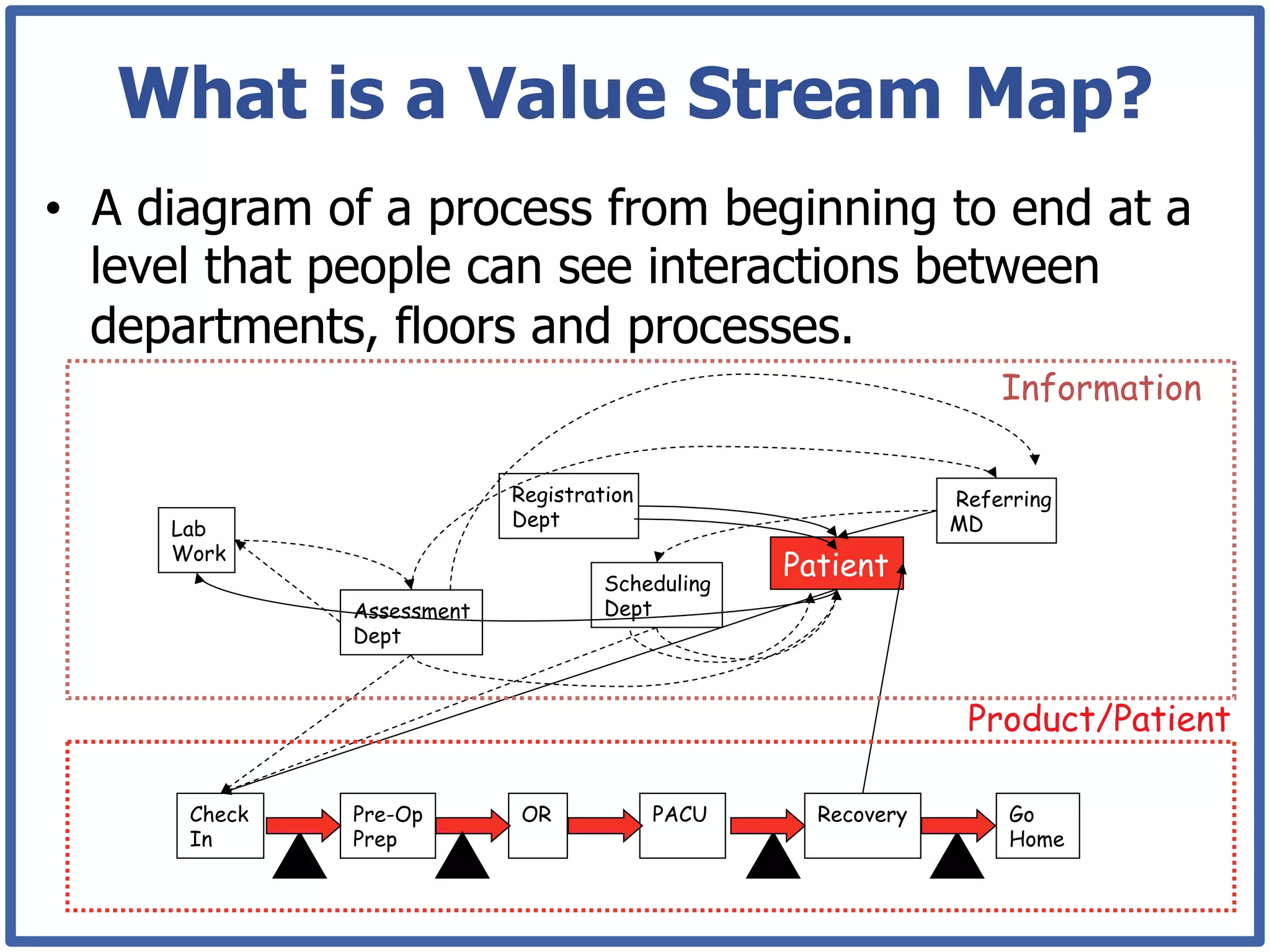
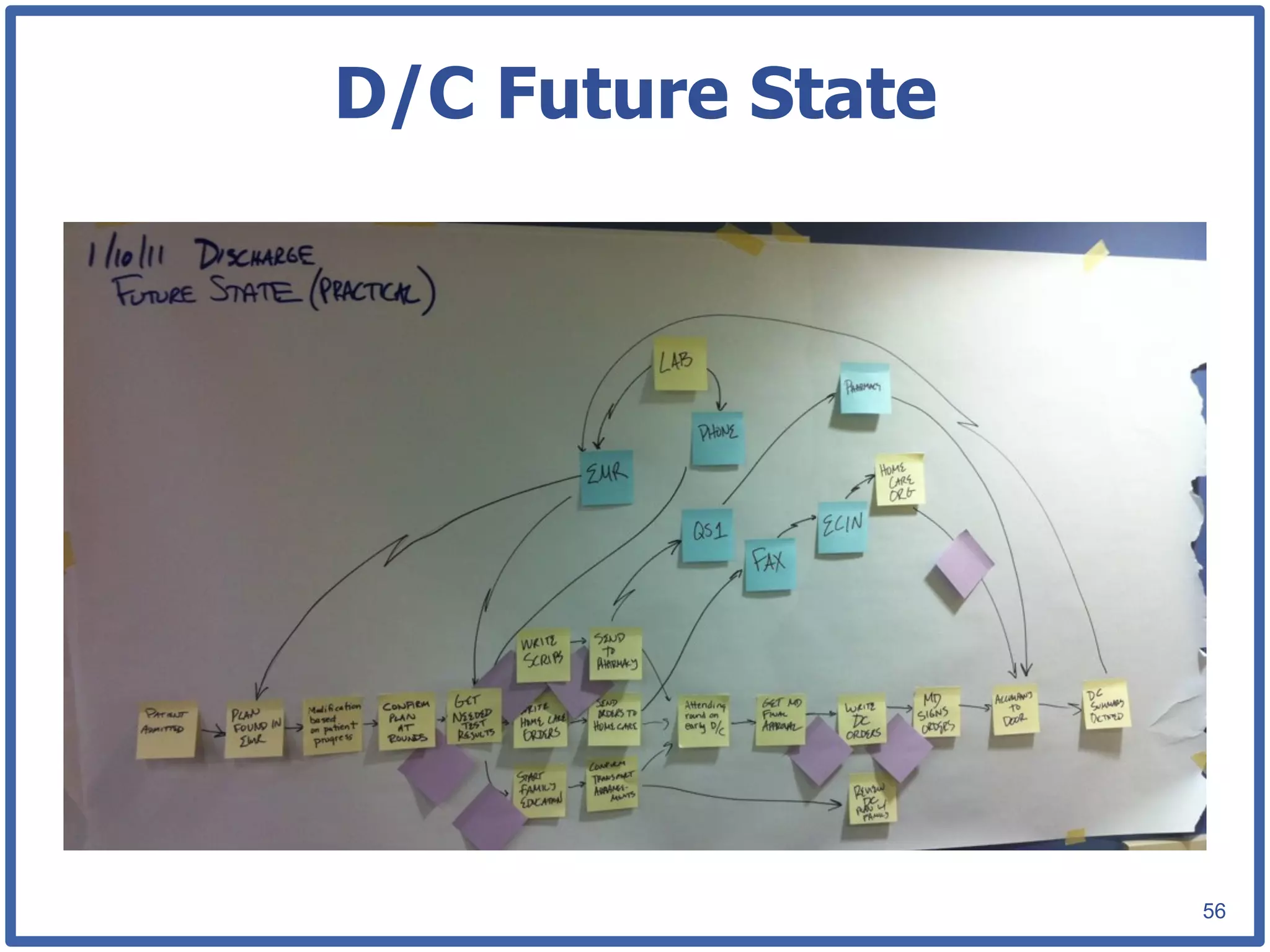
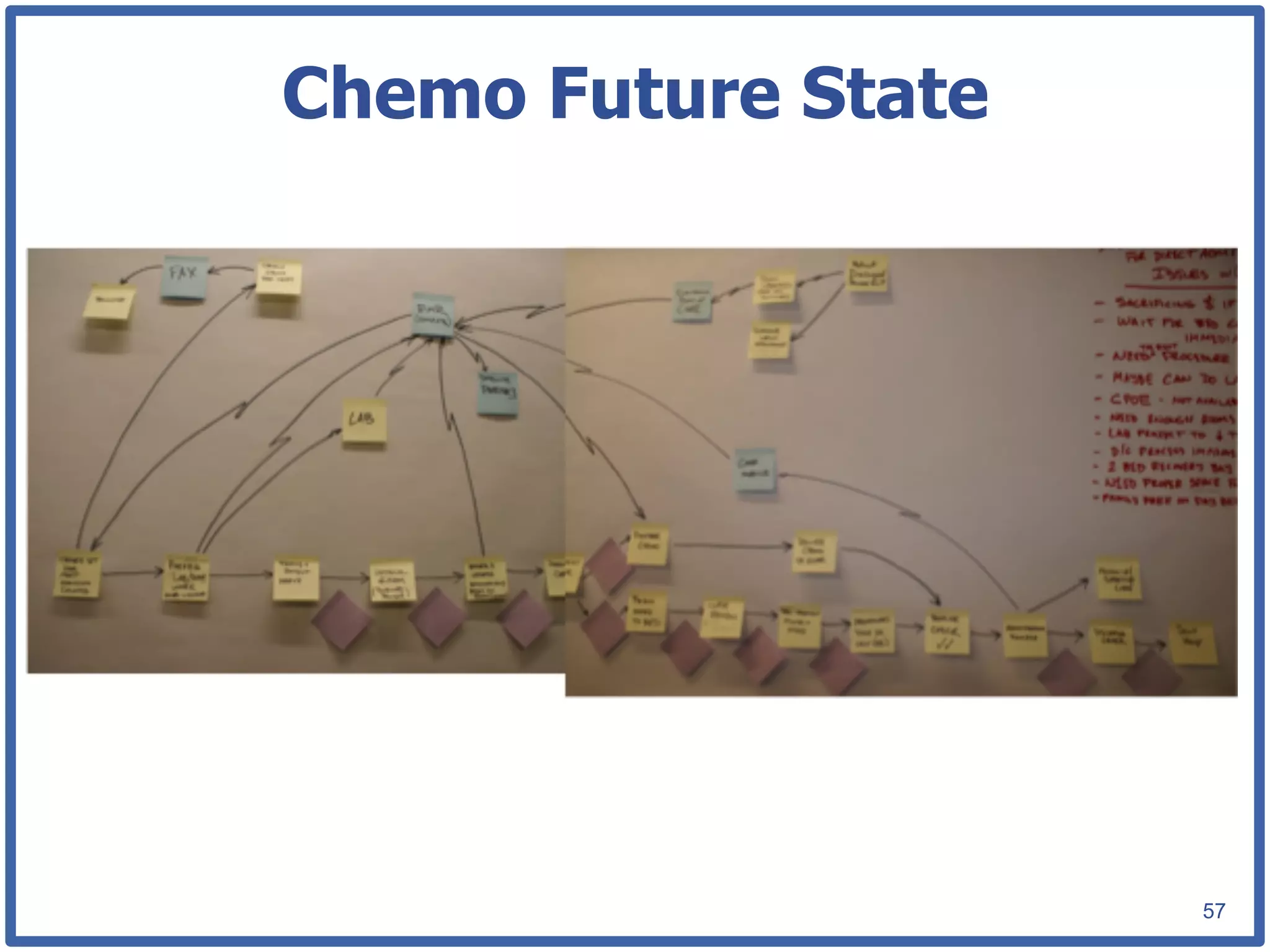
This document discusses how lean principles can be applied to healthcare design and management. It defines lean as a method focused on minimizing waste to provide the best patient care while engaging staff. Lean design uses value stream mapping and iterative improvements to understand workflow and design facilities that optimize flow. Examples show how lean design has reduced costs and space needs while improving quality, safety, and staff satisfaction at several hospitals. The document advocates applying lean principles through cross-functional teams, understanding current processes, and iteratively designing an ideal future state.