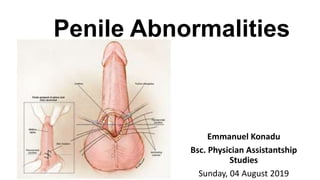
Penile abnormalities
- 1. Penile Abnormalities Emmanuel Konadu Bsc. Physician Assistantship Studies Sunday, 04 August 2019
- 2. OUTLINE • Definition • Embryology and Anatomy • Epidemiology • Aetiology • Pathophysiology • Clinical Presentation • Investigations • Complications • Differential Diagnosis • Management
- 3. DEFINITION Penile abnormalities encompass a variety of disorders of the soft tissues of the male genitalia
- 4. EMBRYOLOGY OF MALE UROGENITAL TRACT • All the components of the urogenital tract undergoes: • Indifferentiation stage: • mesenchyme migrates to cloacal membrane to form genital tubercle • caudal portion of the cloacal membrane develops into urogenital folds • genital swellings become visible on each side of urethral folds
- 5. EMBRYOLOGY OF THE MALE UROGENITAL TRACT • Differentiation into external genitalia in male: • It is under influence of androgens(testosterone) • Rapid elongation of the genital tubercle called the phallus • Phallus pulls the urethral folds to form the lateral walls of the urethral groove • At end of the third month, the two urethral folds close over the urethral plate, forming the penile urethra
- 7. ANATOMY OF THE MALE PENIS • Penis is divided into three parts: • Root of the penis: • lies under the pubic bone • provides stability when the penis is erect • 2 cavernosal bodies and corpus spongiosum • Glans: • Distal expansion of corpus spongiosum
- 8. Phimosis
- 9. DEFINITION Inability to retract the prepuce over the glan of the penis
- 11. TYPES OF PHIMOSIS • Phimosis is divided into two form: • Physiological Phimosis • Occurs naturally in newborn males • Pathological Phimosis • Inability to retract the foreskin after it was previously retractible or after puberty
- 12. EPIDEMIOLOGY • 4% of new-borns will have retractable foreskin • By the age of 3, 90% of the prepuces are retractable • Remaining 10%, will have physiologic phimosis • 1% of 16-year-old will have non-retractile foreskins • 46.5% of adult circumcision was attributed to phimosis
- 13. AETIOLOGY • Congenital • Acquired • Inflammatory • Balanitis • Posthitis • Balanoposthitis • Traumatic • Fibrosis of prepuce • Neoplastic • Underling Ca
- 14. PHYSIOLOGIC PHIMOSIS • Formation of the prepuce is completed by 16 weeks’ gestation • Inner prepuce and glans penis share a common, fused mucosal epithelium • Epithelium separates via desquamation • Desquamation is due to hormonal and growth factors are produced
- 15. PATHOLOGIC PHIMOSIS • Usually the result of poor hygiene or chronic balanoposthitis • Eventually leads formation of fibrotic ring of tissue close to opening of the prepuce • When foreskin is forcefully retracted, it results in significant bleeding • This leads to dense fibrous adhesions formation during healing process leading to pathologic phimosis
- 16. CLINICAL PRESENTATION • HISTORY • Age • Symptoms • Ballooning of foreskin during voiding • Pain • Dysuria • Urinary infections • PHYSICAL EXAMINATION • Inspection • Redness, purulent foreskin • Scarring of the foreskin (white) • Palpation • Tenderness • Retraction of the foreskin not possible
- 17. MANAGEMENT • Management depends on: • age of child • type of non retraction • severity of phimosis • the cause • associated morbid conditions
- 18. TREATMENT • Reassurance and Vigilance • Proper preputial care and hygiene • Topical Steroids • 0.05% Betamethasone twice daily for 4-6 weeks • Dilation and Stretching • Surgical • Conservative Surgical Alternatives • Conventional Male Circumcision
- 19. CIRCUMCISION INDICATIONS • Religious, cultural, hygienic • Phimosis • Paraphimosis • Balanitis • Posthitis CONTRAINDICATIONS • Prematurity • Anomalies of the penis • Bleeding diatheses are not absolute contraindications
- 20. TYPES OF CIRCUMCISION • Using surgical devices • Gomco Clamp • Mogen Clamp • Plastibell • Dorsal Slit • Excision • Sleeve Resection
- 21. TYPES OF CIRCUMCISION • Gomco Clamp: • Bell is placed over glans and foreskin is replaced into the anatomic position • Yoke is then placed over the bell and clamp is tightened, crushing the foreskin • Scalpel is run around the upper surface of the plate to remove the prepuce
- 23. Mogen Clamp • Foreskin is extended using straight hemostats • Mogen clamp is then slid over the foreskin • Clamp is then locked • Scalpel is used to skin from the upper side of the clamp
- 25. Plastibell • Plastibell is placed under foreskin and secured with circumferential ligature • Ring falls off after 4-7 days leaving a circumferential wound
- 26. Dorsal Slit Procedure • Identification of plane b/n dorsal foreskin and corona • Haemostat is used to crush foreskin at 12 o’clock position for 30-60 seconds • Crushed area is sharply incised with scissors • Edges are often over sewn with an interrupted or running dissolvable suture
- 27. Sleeve Resection • Prepuce is retracted over the glans • Circumferential incision is made around the shaft • Prepuce is returned to cover the glans and another incision is made round the shaft • Longitudinal cut is made between the two circumferential • Free raw edges are then sutured with absorbable suture
- 28. Sleeve Resection
- 29. Complications of Circumcision • Early Complications • Bleeding • Infection • Late Complications • Meatitis and Meatal Stenosis • Urethocutaneous Fistula • Necrosis • Phimosis • Glans Injury
- 32. FOLLOW-UP • Routine follow-up after adult circumcision is advisable • Patient may be seen 2-3 weeks after operation
- 33. COMPLICATIONS Associated with Phimosis: • Balanitis • Posthitis • Paraphimosis • Voiding Dysfunction • Penile Carcinoma
- 34. PROGNOSIS • Physiologic phimosis has an excellent prognosis with or without appropriate treatment • Pathologic phimosis usually require treatment and the prognosis is good, if the underlying condition is treated successfully
- 35. Paraphimosis
- 36. Definition Urological emergency in which the retracted foreskin of an uncircumcised male cannot be returned to its anatomical position
- 38. Epidemiology • Relative uncommon condition • The incidence in unknown • Few cases have been reported in literature • Almost always an iatrogenically or inadvertently induced condition
- 39. Aetiology IATROGENIC CAUSES: • Penile examination • Urethral catherization • Cystoscopy OTHER CAUSES: • Self-inflicted injury to the penis • Secondary to penile erection
- 40. PATHOPHYSIOLOGY • Retraction of the foreskin behind the glans penis leads to phimotic ring • Ring causes constriction of the distal glans • Leads to vascular engorgement as the lymphatic and venous are impaired • Causes impediment of the arterial flow and potential ischemia of the penis distal to ring • Eventual necrosis of the glan penis may be observed
- 41. Clinical Presentation• HISTORY • Age • Occurs in young men • Symptoms • Swelling • Penile pain • Obstructive voiding symptom • Past Medical History • No history of circumcision • History of endoscopic surgery of the bladder or urethra • PHYSICAL EXAMINATION • Presence of the foreskin • Colour of the glans • Degree of constriction • Palpation of the glans
- 42. Management • Treatment modalities include • Medical Therapy • Surgical Therapy • The goals of management involves: • Reassuring the patient • Reducing the preputial oedema • Restoring the prepuce to its original position and condition
- 43. MEDICAL THERAPY • Non-pharmacological • Ice packs • Manual Reduction • Pharmacological • Injection of hyaluronidase into oedematous prepuce • Osmotic agents (Mannitol soaked-guaze)
- 44. MANUAL REDUCTION • A gloved hand is circled around the distal penis • A circumferential pressure is applied to disperse the oedema
- 45. SURGICAL THERAPY • Minimally invasive • Puncture technique • Blood aspiration • Dorsal slit • Circumcision
- 46. PUNCTURE TECHNIQUE • Hypodermic needle (21-26 gauge) is used to puncture the oedematous prepuce at multiple sites to release the trapped fluid • External drainage results in rapid resolution of oedema • It is then followed by manual reduction of the prepuce
- 47. DORSAL SLIT PROCEDURE • Skin preparation, draping and anaesthesia • Identification of the plane between the dorsal foreskin and corona • A haemostat is then used to crush the foreskin at 12 o’clock position for 30-60 seconds • The crushed area is then sharply incised with scissors • The edges are often over sewn with an interrupted or running dissolvable suture
- 49. FOLLOW-UP • Follow-up examination in 2-3 weeks
- 50. COMPLICATIONS Associated with Paraphimosis: • Infection • Swelling of the glans • Ischemia and necrosis Associated with Dorsal Slit: • Infection • Bleeding • Urethral Injury • Shortening of penile skin
- 51. OUTCOME AND PROGNOSIS • Does not occur after a proper circumcision • Outcome of dorsal slit is excellent
- 52. Hypospadias
- 53. DEFINITION An abnormal ventral opening of urethral meatus located anywhere from the ventral aspect of glans penis to perineum
- 54. CLASSIFICATION OF HYPOSPADIAS • Is based on the position of meatus • Anterior • Glanular • Subcoronal • Middle • Distal penile • Midshaft • Proxiaml penile • Posterior • Penoscrotal • Scrotal • Perineal
- 55. EPIDEMIOLOGY • Most common congenital malformation • Occurs in one of 350 male births • Incidence is higher in whites than in blacks • Increased rate in premature babies
- 57. AETIOLOGY • The aetiologies for hypospadias include: • Genetic factors • Higher incidence in monozygotic twins • Endocrine factors • Dysfunction in androgen production and utilization. • Mutations in 5-alpha reductase • Maternal exposure to progesterone • Environmental factors
- 58. PATHOPHYSIOLOGY • Occurs embryologically during urethral development • As phallus grows, the open groove extends from its base to the level of the corona • 2 theories proposed to explain pathophysiology • Urethral folds coalesce in midline from base to tip, forming a tubularized penile urethra and median scrotal raphe. • Ectodermal core forming at tip of the glans penis, which canalizes to join with the more proximal urethra at the level of the corona
- 59. DIAGNOSIS • Diagnosis is usually made at birth • History • Familial pattern of hypospadias • History of Infertility • Physical Examination • Position, shape and width of the meatal orifice • Appearance of the preputial hood and scrotum • Size of the penis • Curvature of the penis on erection (chordee) • Deficiency of ventral foreskin
- 60. MANAGEMENT • Treatment is surgical repair • The goals of surgical treatment is to: • To create a straight penis by repairing curvature (chordee) • To create a urethra with its meatus at the tip of penis • To reform the glans into a more natural conical configuration • To achieve cosmetically acceptable penile skin coverage • To create a normal-appearing scrotum
- 61. SURGICAL • Timing of Surgery • Before 1980, repair was performed in children older than 3years • Currently, repair is between 4 and 18 months • Preoperative Hormonal Simulation • HCG 250-500U sc twice a week for 3weeks • Testosterone propionate cream 2% three times daily for 3 weeks
- 62. SURGICAL PRINCIPLES • Use optical magnification • Artificial erection (when appropriate) • Chordee repair (orthoplasty) • Urethral plate preservation if possible • Use well-vascularized non hair-bearing local tissue for urethral construction • Neourethral coverage (1-2 layers) • Catheter (urethral) • Use an appropriate dressing
- 63. COMPLICATIONS OF REPAIR Immediate complications • Postoperative bleeding • Infection Long-term complications • Urethrocutaneous fistula • Meatal/Urethral stenosis • Diverticulum • Hair in the urethra
- 64. THANK YOU
Editor's Notes
- But for that of paraphimosis, one should identify the dorsal midline of the rolled preputial skin. A vertical incision is made at the junction of the rolled foreskin (identified as the point between the mucosal, smooth skin and preputial thicker, dull skin). This should release the constricting tissue.