Diabetes mellitus - 2
- 1. Diabetes Mellitus- Clinical manifestations and complications (Part-2) Biochemistry for medics www.namrata.co 11/2/2013 Biochemistry for medics 1
- 2. Contents Clinical Manifestations of Type 1 DM Clinical manifestations of Type 2 DM Acute complications Chronic complications
- 3. Clinical Manifestations Type 1 DM • Polyuria-Increased urination is a consequence of osmotic diuresis secondary to sustained hyperglycemia. This results in a loss of glucose as well as free water and electrolytes in the urine. • Thirst (Polydipsia) is a consequence of the hyperosmolar state, as is blurred vision, which often develops as the lenses are exposed to hyperosmolar fluids. • Weight loss despite normal or increased appetite is a common feature of type 1 when it develops sub acutely. The weight loss is initially due to depletion of water, glycogen, and triglycerides; thereafter, reduced muscle mass occurs as amino acids are diverted to form glucose and ketone bodies. 11/2/2013 Biochemistry for medics 3
- 4. Clinical Manifestations Type 1 DM (contd.) • Lowered plasma volume produces symptoms of postural hypotension. Total body potassium loss and the general catabolism of muscle protein contribute to the weakness. • Paresthesias may be present at the time of diagnosis, particularly when the onset is sub acute. They reflect a temporary dysfunction of peripheral sensory nerves, which clears as insulin replacement restores glycemic levels closer to normal, suggesting neurotoxicity from sustained hyperglycemia. When absolute insulin deficiency is of acute onset, the above symptoms develop abruptly. 11/2/2013 Biochemistry for medics 4
- 5. Clinical Manifestations Type 1 DM (contd.) Ketoacidosis o Ketoacidosis exacerbates the dehydration and hyperosmolality by producing anorexia , nausea and vomiting, interfering with oral fluid replacement. o The patient's level of consciousness can vary depending on the degree of hyperosmolality. 11/2/2013 Biochemistry for medics 5
- 6. Diabetic ketoacidosis – contd. oWhen insulin deficiency develops relatively slowly and sufficient water intake is maintained, patients remain relatively alert and physical findings may be minimal. oWhen vomiting occurs in response to worsening ketoacidosis, dehydration progresses and compensatory mechanisms become inadequate to keep serum osmolality below 320–330 mOsm/L. oUnder these circumstances, stupor or even coma may occur. oThe fruity breath odor of acetone further suggests the diagnosis of diabetic ketoacidosis. 11/2/2013 Biochemistry for medics 6
- 7. Clinical Manifestations Type 1 DM (contd.) • Hypotension in the recumbent position is a serious prognostic sign. • Loss of subcutaneous fat and muscle wasting are features of more slowly developing insulin deficiency. In occasional patients with slow, insidious onset of insulin deficiency, subcutaneous fat may be considerably depleted. 11/2/2013 Biochemistry for medics 7
- 8. Clinical Manifestations Type 2 DM • While many patients with type 2 diabetes present with increased urination and thirst, many others have an insidious onset of hyperglycemia and are asymptomatic initially. This is particularly true in obese patients, whose diabetes may be detected only after Glycosuria or hyperglycemia is noted during routine laboratory studies. 11/2/2013 Biochemistry for medics 8
- 9. Clinical Manifestations Type 2 DM (contd.) o Occasionally, type 2 patients may present with evidence of neuropathic or cardiovascular complications because of occult disease present for some time prior to diagnosis. o Chronic skin infections are common. Generalized pruritus and symptoms of vaginitis are frequently the initial complaints of women. o Diabetes should be suspected in women with chronic Candida vulvovaginitis as well as in those who have delivered large babies (> 9 lb, or 4.1 kg) or have had polyhydramnios, preeclampsia, or unexplained fetal losses. 11/2/2013 Biochemistry for medics 9
- 10. Clinical Manifestations Type 2 DM (contd.) •Obese diabetics may have any variety of fat distribution; however, diabetes seems to be more often associated in both men and women with localization of fat deposits on the upper segment of the body (particularly the abdomen, chest, neck, and face) and relatively less fat on the appendages, which may be quite muscular. •Standardized tables of waist-to-hip ratio indicate that ratios of "greater than 0.9" in men and "greater than 0.8" in women are associated with an increased risk of diabetes in obese subjects 11/2/2013 Biochemistry for medics 10
- 11. Clinical Manifestations Type 2 DM (contd.) • Mild hypertension is often present in obese diabetics. • Eruptive xanthomas on the flexor surface of the limbs and on the buttocks and Lipemia retinalis due to hyperchylomicronemia can occur in patients with uncontrolled type 2 diabetes who also have a familial form of hypertriglyceridemia. 11/2/2013 Biochemistry for medics 11
- 12. Complications of Diabetes Mellitus • Acute Complications of DM o Diabetic ketoacidosis o Hyperosmolar non ketotic coma o Lactic acidosis o Hypoglycemia 11/2/2013 Biochemistry for medics 12
- 13. Diabetic ketoacidosis • Diabetic Ketoacidosis (DKA) is a state of inadequate insulin levels resulting in high blood sugar and accumulation of organic acids and ketones in the blood. • It is a potentially life-threatening complication in patients with diabetes mellitus. • It happens predominantly in type 1 diabetes mellitus, but it can also occur in type 2 diabetes mellitus under certain circumstances. 11/2/2013 Biochemistry for medics 13
- 14. Diabetic ketoacidosis- Causes • DKA most frequently occurs in known diabetics. • It may also be the first presentation in patients who had not previously been diagnosed as diabetics. • There is often a particular underlying problem that has led to the DKA episode. • This may be intercurrent illness (pneumonia, influenza, gastroenteritis, a urinary tract infection), pregnancy, inadequate insulin administration (e.g. defective insulin pen device), myocardial infarction (heart attack), stroke or the use of cocaine. 11/2/2013 Biochemistry for medics 14
- 15. Diabetic ketoacidosis- Causes (contd.) • Young patients with recurrent episodes of DKA may have an underlying eating disorder, or may be using insufficient insulin for fear that it will cause weight gain. • In 5% of cases, no cause for the DKA episode is found. • Diabetic ketoacidosis may occur in those previously known to have diabetes mellitus type 2 or in those who on further investigations turn out to have features of type 2 diabetes (e.g. obesity, strong family history); • This is more common in African, African-American and Hispanic people. • Their condition is then labeled "ketosis-prone type 2 diabetes". 11/2/2013 Biochemistry for medics 15
- 16. Diabetic ketoacidosis- Pathophysiology • DKA results from relative or absolute insulin deficiency combined with counter regulatory hormone excess (Glucagon, Catecholamines, cortisol, and growth hormone). • The decreased ratio of insulin to Glucagon promotes Gluconeogenesis, glycogenolysis, and Ketone body formation in the liver, as well as increases in substrate delivery from fat and muscle (free fatty acids, amino acids) to the liver. 11/2/2013 Biochemistry for medics 16
- 17. Diabetic ketoacidosis- Pathophysiology • Normally, the free fatty acids released by adipolysis are converted to triglycerides or VLDL in the liver. • However, in DKA, hyperglucagonemia alters hepatic metabolism to favor Ketone body formation, through activation of the enzyme carnitine palmitoyl Transferase I. • This enzyme is crucial for regulating fatty acid transport into the mitochondria, where beta oxidation and conversion to ketone bodies occur. 11/2/2013 Biochemistry for medics 17
- 18. Diabetic ketoacidosis- Pathophysiology • The ketone bodies, however, have a low pH and therefore turn the blood acidic (metabolic acidosis). • The body initially buffers this with the bicarbonate buffering system, but this is quickly overwhelmed and other mechanisms to compensate for the acidosis, such as hyperventilation to lower the blood carbon dioxide levels. • This hyperventilation, in its extreme form, may be observed as Kussmaul respiration. • Ketones, too, participate in osmotic diuresis and lead to further electrolyte losses. 11/2/2013 Biochemistry for medics 18
- 19. DKA- Clinical manifestations • Nausea and vomiting • Pronounced thirst • Excessive urine production and abdominal pain that may be severe. • Hyperglycemia is always present . •In severe DKA, breathing becomes labored and of a deep, gasping character (a state referred to as "Kussmaul respiration"). 11/2/2013 Biochemistry for medics 19
- 20. DKA- Clinical manifestations (contd.) •The abdomen may be tender to the point that an acute abdomen may be suspected, such as acute pancreatitis, appendicitis or gastrointestinal perforation. •Coffee ground vomiting (vomiting of altered blood) occurs in a minority of patients; this tends to originate from erosions of the esophagus. • In severe DKA, there may be confusion, lethargy, stupor or even coma (a marked decrease in the level of consciousness). 11/2/2013 Biochemistry for medics 20
- 21. DKA- Clinical manifestations (contd.) • On physical examination there is usually clinical evidence of dehydration, such as a dry mouth and decreased skin turgor. • If the dehydration is profound enough to cause a decrease in the circulating blood volume, tachycardia (a fast heart rate) and low blood pressure may be observed. • Often, a "ketotic" odor is present, which is often described as "fruity". • If Kussmaul respiration is present, this is reflected in an increased respiratory rate. 11/2/2013 Biochemistry for medics 21
- 22. Diagnosis of DKA • Diabetic Ketoacidosis may be diagnosed when the combination of hyperglycemia (high blood sugars), ketones on urinalysis and acidosis are demonstrated. • Arterial blood gas measurement is usually performed to demonstrate the acidosis • Urea and creatinine estimations (measures of kidney function, which may be impaired in DKA as a result of dehydration) and electrolytes. 11/2/2013 Biochemistry for medics 22
- 23. Diagnosis of DKA • Markers of infection (complete blood count, Creactive protein) and acute pancreatitis (amylase and lipase) may be measured. • Given the need to exclude infection, chest radiography and urinalysis are usually performed. • If cerebral edema is suspected because of confusion, recurrent vomiting or other symptoms, computed tomography may be performed to assess its severity and to exclude other causes such as stroke. 11/2/2013 Biochemistry for medics 23
- 24. Management of DKA • The main aims in the treatment of diabetic ketoacidosis are replacing the lost fluids and electrolytes while suppressing the high blood sugars and ketone production with insulin. • Fluid replacement- The amount of fluid depends on the estimated degree of dehydration • Insulin is usually given continuously. 11/2/2013 Biochemistry for medics 24
- 25. Management of DKA (contd.) • Potassium levels can fluctuate severely during the treatment of DKA, because insulin decreases potassium levels in the blood by redistributing it into cells. • Serum potassium levels are initially often mildly raised even though total body potassium is depleted. Hypokalemia often follows treatment. • This increases the risk of irregularities in the heart rate. Therefore, continuous observation of the heart rate is recommended, as well as repeated measurement of the potassium levels and addition of potassium to the intravenous fluids once levels fall below 5.3 mmol/l. •If potassium levels fall below 3.3 mmol/l, insulin administration may need to be interrupted to allow correction of the hypokalemia. 11/2/2013 Biochemistry for medics 25
- 26. Management of DKA (contd.) Bicarbonate • Sodium bicarbonate solution is administered to rapidly improve the acid levels in the blood. • Cerebral edema- administration of fluids is slowed; intravenous Mannitol and hypertonic saline (3%) are used 11/2/2013 Biochemistry for medics 26
- 27. 2) Hyperglycemic Hyperosmolar State (HHS) Pathophysiology • Relative insulin deficiency and inadequate fluid intake are the underlying causes of HHS. • Insulin deficiency increases hepatic glucose production (through glycogenolysis and gluconeogenesis) and impairs glucose utilization in skeletal muscle . • Hyperglycemia induces an osmotic diuresis that leads to intravascular volume depletion, which is exacerbated by inadequate fluid replacement. 11/2/2013 Biochemistry for medics 27
- 28. 2) Hyperglycemic Hyperosmolar State (HHS)- contd. Clinical Features• HHS occurs in elderly individuals with type 2 DM, with a several week history of polyuria, weight loss, and diminished oral intake that culminates in mental confusion, lethargy, or coma. The physical examination reveals• Profound dehydration and hyperosmolality • Hypotension, tachycardia, and altered mental status. • Nausea, vomiting, abdominal pain and the Kussmaul respirations characteristic of DKA are absent. • HHS is often precipitated by a serious, concurrent illness such as myocardial infarction or stroke. • Sepsis, pneumonia, and other serious infections are frequent precipitants and should be sought. 11/2/2013 Biochemistry for medics 28
- 29. 2) Hyperglycemic Hyperosmolar State (HHS)- contd. • Most notable are the marked hyperglycemia [plasma glucose may be >55.5 mmol/L (1000 mg/dL)], hyperosmolality (>350 mosmol/L), and prerenal azotemia. • In contrast to DKA, acidosis and ketonemia are absent or mild. Treatment- The rehydration in HHS should be slower to avoid neurological damage. The insulin dose requirements are usually lower than in DKA. 11/2/2013 Biochemistry for medics 29
- 30. 3) Lactic acidosis • Lactic acidosis occurs in hypoxic individuals and is due to an excessive production of lactate by peripheral tissues. •It is characterized by extreme metabolic acidosis. •There is high anion gap with low or absent ketones and high lactate levels. TreatmentSodium bicarbonate is needed to correct the acidosis. 11/2/2013 Biochemistry for medics 30
- 31. 4) Hypoglycemia •Hypoglycemia caused by excess insulin is the most common complication of insulin therapy, occurring in more than 90 % of the patients. • In normal individuals, hypoglycemia triggers a compensatory secretion of counter regulatory hormones, most notably glucagon and epinephrine, which promote hepatic production of glucose. However patients with type 1 diabetes also develop a deficiency of glucagon secretion. 11/2/2013 Biochemistry for medics 31
- 32. 4) Hypoglycemia- contd. •These patients thus rely on epinephrine secretion to prevent severe hypoglycemia. •However as the disease progresses, type 1 diabetes patients show diabetic autonomic neuropathy and impaired ability to secrete epinephrine in response to hypoglycemia. •The combined deficiency of glucagon and epinephrine secretion creates a condition sometimes called “Hypoglycemia unawareness”. •Thus patients with long standing diabetes are particularly vulnerable to hypoglycemia 11/2/2013 Biochemistry for medics 32
- 33. Chronic Complications of DM • Chronic complications can be divided into vascular and nonvascular complications. • The vascular complications of DM are further subdivided into microvascular and macrovascular • Microvascular complications includeo Retinopathy o Neuropathy, and o Nephropathy 11/2/2013 Biochemistry for medics 33
- 34. Chronic Complications of DM- contd. Macro vascular complications includeo Coronary artery disease (CAD), o Peripheral arterial disease (PAD), o Cerebrovascular disease. Nonvascular complications include Gastroparesis, infections, and skin changes. Long-standing diabetes may be associated with hearing loss. 11/2/2013 Biochemistry for medics 34
- 35. Mechanisms of Complications • Advanced Glycosylation End Products Increased intracellular glucose leads to the formation of advanced glycosylation end products (AGEs) via the nonenzymatic glycosylation of intraand extra cellular proteins. AGEs have been shown to cross-link proteins (e.g., collagen, extracellular matrix proteins), accelerate atherosclerosis, promote glomerular dysfunction, reduce nitric oxide synthesis, induce endothelial dysfunction, and alter extracellular matrix composition and structure. 11/2/2013 Biochemistry for medics 35
- 36. Mechanisms of Complications- contd. 2) Sorbitol pathway o Hyperglycemia increases glucose metabolism via the Sorbitol pathway. oIncreased sorbitol concentration alters redox potential, increases cellular osmolality, generates reactive oxygen species, and likely leads to other types of cellular dysfunction. 11/2/2013 Biochemistry for medics 36
- 37. Mechanisms of Complications- contd. 3) Activation of protein kinase C (PKC) o Hyperglycemia increases the formation of diacylglycerol leading to activation of protein kinase C (PKC). o Among other actions, PKC alters the transcription of genes for fibronectin, type IV collagen, contractile proteins, and extracellular matrix proteins in endothelial cells and neurons. 11/2/2013 Biochemistry for medics 37
- 38. Mechanisms of Complications- contd. • A fourth theory proposes that hyperglycemia increases the flux through the hexosamine pathway, which generates fructose-6phosphate, a substrate for O-linked glycosylation and proteoglycan production. • The hexosamine pathway may alter function by glycosylation of proteins 11/2/2013 Biochemistry for medics 38
- 39. Mechanisms of Complications- contd. Oxidative stress • Hyperglycemia leads to increased production of reactive oxygen species or Superoxide in the mitochondria; •These compounds may activate all four of the pathways described above. • Although hyperglycemia serves as the initial trigger for complications of diabetes, it is still unknown whether the same pathophysiological processes are operative in all complications or whether some pathways predominate in certain organs. 11/2/2013 Biochemistry for medics 39
- 40. Vascular complications Microvascular complications Ocular Complications • DM is the leading cause of blindness between the ages of 20 and 74 in the United States. • Blindness is primarily the result of progressive diabetic retinopathy and clinically significant macular edema. 11/2/2013 Biochemistry for medics 40
- 41. Ocular Complications Diabetic retinopathy • Diabetic retinopathy is classified into two stages: nonproliferative and proliferative. • Nonproliferative diabetic retinopathy is marked by retinal vascular micro aneurysms, blot hemorrhages, and cotton wool spots . • The appearance of neovascularization in response to retinal hypoxia is the hallmark of proliferative diabetic retinopathy 11/2/2013 Biochemistry for medics 41
- 42. Diabetic retinopathy 11/2/2013 Biochemistry for medics 42
- 43. Ocular Complications- contd. Diabetic cataract • Premature cataracts occur in diabetic patients and seem to correlate with both the duration of diabetes and the severity of chronic hyperglycemia. • Nonenzymatic glycosylation of lens protein contributes to the premature occurrence of cataract. 11/2/2013 Biochemistry for medics 43
- 44. Diabetic Cataract 11/2/2013 Biochemistry for medics 44
- 45. Ocular Complications- contd. Glaucoma • Glaucoma occurs in approximately 6% of persons with diabetes. • It is responsive to the usual therapy for openangle disease. • Neovascularization of the iris in diabetics can predispose to closed-angle glaucoma, but this is relatively uncommon except after cataract extraction, when growth of new vessels has been known to progress rapidly, involving the angle of the iris and obstructing outflow. 11/2/2013 Biochemistry for medics 45
- 46. Renal Complications Diabetic nephropathy (nephropatia diabetica), also known as Kimmelstiel-Wilson syndrome, and intercapillary glomerulonephritis, is a progressive kidney disease • It is the principal cause of ESRD (End Stage Renal Disease) in the western world. • Like other microvascular complications, the pathogenesis of diabetic nephropathy is related to chronic hyperglycemia 11/2/2013 Biochemistry for medics 46
- 47. Diabetic nephropathy The mechanisms involves the effects of• Soluble factors oGrowth factors, oAngiotensin II, oEndothelin oAGEs • Hemodynamic alterations in the renal microcirculation (glomerular hyper filtration or hyper perfusion, increased glomerular capillary pressure), and •Structural changes in the glomerulus (increased extracellular matrix, basement membrane thickening 11/2/2013 Biochemistry for medics 47 and fibrosis).
- 48. Diabetic nephropathy-contd. • The earliest detectable change in the course of diabetic nephropathy is a thickening in the glomerulus. • At this stage, the kidney may start allowing more albumin than normal in the urine (albuminuria), and this can be detected by sensitive medical tests for albumin. • This stage is called "microalbuminuria". • After 5–10 years of type 1 DM, ~40% of individuals begin to show microalbuminuria. • Microalbuminuria is defined as 30–300 mg/d of albumin in a 24-h collection of urine. • As diabetic nephropathy progresses, increasing numbers of glomeruli are destroyed by nodular glomerulosclerosis. 11/2/2013 Biochemistry for medics 48
- 49. Diabetic nephropathy-contd. • Although the appearance of microalbuminuria in type 1 DM, is an important risk factor for progression to overt proteinuria (in>300 mg/d), only ~50% of individuals will progress to macroalbuminuria over the next 10 years. • Once macroalbuminuria is present, there is a steady decline in GFR (Glomerular Filtration Rate), and ~50% of individuals reach ESRD (End Stage Renal Disease) in 7–10 years. • Once macroalbuminuria develops, blood pressure rises slightly and the pathologic changes are likely to be irreversible. • At this stage, a kidney biopsy clearly shows diabetic nephropathy. 11/2/2013 Biochemistry for medics 49
- 50. Diabetic nephropathy-contd. Clinical Manifestations • Kidney failure provoked by glomerulosclerosis leads to fluid filtration deficits and other disorders of kidney function. • There is an increase in blood pressure and fluid retention in the body causing edema. • Other complications may be arteriosclerosis of the renal artery and proteinuria. •Foamy appearance or excessive frothing of the urine (caused by the proteinuria) • Unintentional weight gain (from fluid accumulation) 11/2/2013 Biochemistry for medics 50
- 51. Diabetic nephropathy-contd. Laboratory Diagnosis • The first laboratory abnormality is a positive microalbuminuria test. • The urinalysis may also show glucose in the urine, especially if blood glucose is poorly controlled. • Serum creatinine and BUN may increase as kidney damage progresses. • Dyslipidemia is a common associated finding. • A Renal biopsy confirms the diagnosis. 11/2/2013 Biochemistry for medics 51
- 52. Diabetic nephropathy 11/2/2013 Biochemistry for medics 52
- 53. Neurological complications Diabetic Neuropathy •Diabetic neuropathy occurs in ~50% of individuals with long-standing type 1 and type 2 DM. • It may manifest as polyneuropathy, mononeuropathy, and/or autonomic neuropathy. • Both myelinated and unmyelinated nerve fibers are lost. 11/2/2013 Biochemistry for medics 53
- 54. Diabetic Neuropathy 11/2/2013 Biochemistry for medics 54
- 55. Diabetic Neuropathy Polyneuropathy/Mononeuropathy • The most common form of diabetic neuropathy is distal symmetric polyneuropathy. •It most frequently presents with distal sensory loss, but up to 50% of patients do not have symptoms of neuropathy. •Loss of function appears in a stocking-glove pattern. •Hyperesthesia, paresthesias, and dysesthesia also may occur. •Symptoms may include a sensation of numbness, tingling, sharpness, or burning that begins in the feet and spreads proximally. •Mononeuropathy (dysfunction of isolated cranial or peripheral nerves) is less common than polyneuropathy in DM and presents with pain and motor weakness in the distribution of a single nerve. 11/2/2013 Biochemistry for medics 55
- 56. Diabetic Neuropathy- contd. Autonomic Neuropathy • Individuals with long-standing type 1 or 2 DM may develop signs of autonomic dysfunction • DM-related autonomic neuropathy can involve multiple systems, including the cardiovascular, gastrointestinal, genitourinary, and metabolic systems. •Autonomic neuropathy may reduce counterregulatory hormone release, leading to an inability to sense hypoglycemia appropriately thereby subjecting the patient to the risk of severe hypoglycemia and complicating efforts to improve glycemic control. 11/2/2013 Biochemistry for medics 56
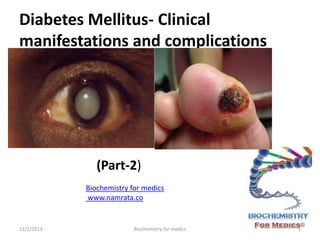
- 58. Diabetic gangrene • The incidence of gangrene of the feet in diabetics is 30 times more than that in age-matched controls. • The factors responsible for its development, in addition to peripheral vascular disease, are small vessel disease, peripheral neuropathy with loss of both pain sensation and neurogenic inflammatory responses, and secondary infection. • The peripheral sensory neuropathy interferes with normal protective mechanisms and allows the patient to sustain major or repeated minor trauma to the foot, often without knowledge of the injury. 11/2/2013 Biochemistry for medics 58
- 59. Diabetic gangrene- contd. • Peripheral artery disease(PAD) and poor wound healing impede resolution of minor breaks in the skin, allowing them to enlarge and to become infected. • Approximately 15% of individuals with DM develop a foot ulcer (great toe or MTP areas are most common), and a significant subset will ultimately undergo amputation (14–24% risk with that ulcer or subsequent ulceration). 11/2/2013 Biochemistry for medics 59
- 60. Diabetic Foot 11/2/2013 Biochemistry for medics 60
- 61. Skin and Mucous Membrane Complications • Chronic pyogenic infections of the skin may occur, especially in poorly controlled diabetic patients • Fungal infections are also very common in diabetics • It causes vulvovaginitis in most chronically uncontrolled diabetic women with persistent glucosuria and is a frequent cause of pruritus. 11/2/2013 Biochemistry for medics 61
- 62. Large vessel diseases (Macro vascular complications) Atherosclerosis and its effects produce the large vessel diseases. a) Involvement of the coronary vessels can produce myocardial infarction, b) Involvement of cerebral vessels can produce ‘stroke’. c) Peripheral vascular disease-Atherosclerosis is markedly accelerated in the larger arteries . Clinical manifestations of peripheral vascular disease include ischemia of the lower extremities, impotence, and intestinal angina. 11/2/2013 Biochemistry for medics 62
- 63. For further details FollowA case oriented approach towards Biochemistry http://www.jaypeedigital.com/BookDetails.aspx?i d=9789350901885&sr=1 11/2/2013 Biochemistry for medics 63
