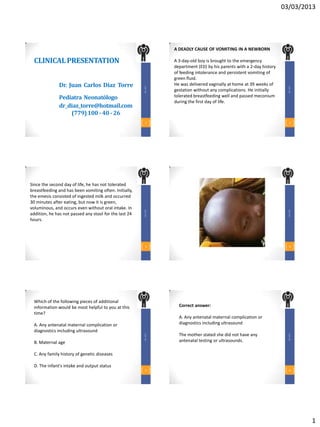
A deadly cause of vomiting in a newborn
- 1. 03/03/2013 A DEADLY CAUSE OF VOMITING IN A NEWBORN CLINICAL PRESENTATION A 3-day-old boy is brought to the emergency department (ED) by his parents with a 2-day history of feeding intolerance and persistent vomiting of green fluid. Dr. Juan Carlos Díaz Torre He was delivered vaginally at home at 39 weeks of DR. JCDT DR. JCDT gestation without any complications. He initially Pediatra Neonatólogo tolerated breastfeeding well and passed meconium during the first day of life. dr_diaz_torre@hotmail.com (779) 100 - 40 - 26 1 2 Since the second day of life, he has not tolerated breastfeeding and has been vomiting often. Initially, the emesis consisted of ingested milk and occurred 30 minutes after eating, but now it is green, voluminous, and occurs even without oral intake. In DR. JCDT DR. JCDT addition, he has not passed any stool for the last 24 hours. 3 4 Which of the following pieces of additional information would be most helpful to you at this Correct answer: time? A. Any antenatal maternal complication or A. Any antenatal maternal complication or diagnostics including ultrasound diagnostics including ultrasound The mother stated she did not have any DR. JCDT DR. JCDT B. Maternal age antenatal testing or ultrasounds. C. Any family history of genetic diseases D. The infant's intake and output status 5 6 1
- 2. 03/03/2013 On exam, you have a full-term baby boy in poor general condition. He is awake but hypotonic and Our patient's head is normocephalic, with a hyporeactive. His temperature is 96.6°F (35.9°C), depressed anterior fontanel, and the mucous heart rate is 175 beats/min, respiratory rate is 48 membranes are dry. breaths/min, and blood pressure is 75/40 mm Hg. He has a generalized grayish coloration, with The trachea is in a central position and there is no DR. JCDT DR. JCDT acrocyanosis, and poor skin turgor. jugular venous distension. On chest examination, the respiratory movements are fast and shallow. Both lungs are clear to auscultation. Although tachycardic, the heart rate is regular and without murmurs. 7 8 The patient's upper abdomen is grossly distended and the lower abdomen is scaphoid. There is a mild bluish discoloration of the abdominal skin, which also appears shiny and thin. Subcutaneous veins are You should initiate all of the following easily seen. The baby retracts his legs upwards and EXCEPT: cries while the abdomen is being palpated. No masses are palpated, and no bowel sounds are A. 20 cc/kg bolus of ringer lactate DR. JCDT DR. JCDT noted. There is no rebound tenderness. On rectal examination with a thermometer, bloody mucus is B. Heel-stick glucose seen. The external genitalia are normal for the patient's C. Oxygen by nasal cannula at 1 L/min age and gender. The extremities are thin and there is skin tenting. The capillary refill time is documented 9 D. Lumbar puncture 10 at 4 seconds. The nurse starts a 20 cc/kg bolus of Correct answer: ringer lactate, oxygen by nasal cannula at 1 L/min, serum glucose, A. 20 cc/kg bolus of ringer lactate places a urine catheter with no urine present in the bladder, places an DR. JCDT DR. JCDT B. Heel-stick glucose orogastric tube and evacuates 35 cc of bilious material. C. Oxygen by nasal cannula at 1 L/min D. Lumbar puncture **** 11 12 2
- 3. 03/03/2013 The infant is then brought to the radiology department for a plain supine abdominal x-ray that This x-ray should be followed by is depicted below. which diagnostic test? A. CT of the abdomen and pelvis DR. JCDT DR. JCDT B. Ultrasonography C. Upper gastrointestinal (GI) series D. Barium enema 13 14 Correct answer: A. CT of the abdomen and pelvis B. Ultrasonography DR. JCDT DR. JCDT C. Upper gastrointestinal (GI) series **** D. Barium enema The upper GI contrast study lateral 15 view comes back as the above. 16 What is the cause of the child's persistent Correct answer: vomiting? A. Malrotation with midgut volvulus **** A. Malrotation with midgut volvulus DR. JCDT DR. JCDT B. Intussusception B. Intussusception C. Necrotizing enterocolitis (NEC) C. Necrotizing enterocolitis (NEC) D. Hirschsprung disease D. Hirschsprung disease 17 18 3
- 4. 03/03/2013 This upper GI study confirms the malrotation with midgut volvulus, with a dilated fluid-filled duodenum (blue arrow), a "corkscrew" pattern (red arrow), and the classic "C" shape of the small bowel on the right side of the abdomen. DR. JCDT DR. JCDT An upper GI study is preferable because malrotation includes a spectrum of conditions, which may prevent the intestine from being completely nonrotated to only partially rotated and can be missed on a barium enema. 19 20 When normal rotation is not completed, or it does not happen at all, the small bowel is fixed and Between the 4th and 10th week of embryonic life, supported only by a narrow base of the mesentery. the developing small intestine moves outside the abdominal cavity and into the umbilical cord. By the It can twist in a clockwise direction, causing both a 11th week, rotation and final placement of the bowel obstruction and simultaneously DR. JCDT DR. JCDT intestines occurs, including a 270° counterclockwise compromising perfusion to the entire midgut, giving turn that leaves the duodenojejunal junction at the it a dark, dusky appearance when viewed surgically. ligament of Treitz fixed to the left of midline and the cecum fixed in the right lower quadrant. Malrotation is found in 0.5%-2% of asymptomatic patients, and it is twice as common in boys as it is in girls. 21 22 Bilious emesis is the hallmark feature of the diagnosis, with more than 95% of volvulus patients presenting with this symptom; an infant who presents with acidosis should heighten your suspicion for volvulus. It is commonly associated with polyhydraminos on prenatal ultrasound. DR. JCDT DR. JCDT Midgut volvulus, as depicted in this image, is the most The initial management of suspected midgut volvulus common and catastrophic complication of a pre- should include fluid administration, nasogastric existing malrotation. Approximately 30% of cases occur suctioning, and imaging with plain radiography. Blood during the first week of life, and greater than 50% of should be sent to the laboratory for a complete blood cases occur before 1 month of age. cell count and metabolic panel. A finding of acidosis 23 24 should raise suspicion. 4
- 5. 03/03/2013 The other causes of vomiting in an infant should be excluded with history, physical examination, or diagnostic imaging. The treatment for malrotation with or without volvulus is surgical fixation. The differential diagnosis of a vomiting infant DR. JCDT DR. JCDT includes infectious etiologies, congenital malformations like malrotation or tracheoesophogeal fistula, or surgical causes including NEC or pyloric stenosis. 25 26 While malrotation can present at ages from infancy to older childhood depending on the amount of malrotation and obstruction, older children would DR. JCDT DR. JCDT Since malrotation can cause a very proximal present with failure to thrive, malabsorption, and obstruction, it can be easily confused with duodenal recurrent abdominal pain. atresia, which presents in the same time period as malrotation with volvulus. X-ray evidence of duodenal atresia can show a 27 28 "double bubble" sign, which is evidence of a proximal small bowel obstruction or a gasless abdomen. If our patient had a very similar acute presentation of Correct answer: inconsolable episodic crying, vomiting, and with blood in the stool but presented at 6 months of age A. Ultrasound with a round, hyperechoic mass at the and had the above x-rays, what would you expect on gastric outlet your next diagnostic test? B. Ultrasound with a swirled appearance of A. Ultrasound with a round, hyperechoic mass at the sonolucent and hyperechoic bowel wall with a DR. JCDT DR. JCDT gastric outlet loop-within-a-loop appearance **** B. Ultrasound with a swirled appearance of sonolucent and hyperechoic bowel wall with a C. CT scan with thickened enlarged appendix loop-within-a-loop appearance C. CT scan with thickened enlarged appendix D. A normal x-ray, no need for further evaluation at D. A normal x-ray, no need for further evaluation at 29 this time 30 this time 5
- 6. 03/03/2013 Intussusception is the predominant cause of Ultrasound demonstrates a swirled appearance of intestinal obstruction in children 6 months to 6 sonolucent and hyperechoic bowel wall with a loop- years, with a 1-4 per 1000 live births incidence and within-a-loop appearance, as shown above. male predominance. Treatment is reduction with air or contrast enema DR. JCDT DR. JCDT Mortality with treatment is 1%-3%, but if untreated, and can be complicated by recurrence or bowel this condition is uniformly fatal in 2-5 days. perforation. Intussusception is the invagination of bowel into more distal bowel caused by intestinal abnormality, adhesions, or bowel swelling. 31 32 A. Pyloric stenosis, order an ultrasound and call a surgeon B. Malrotation with midgut volvulus, place a nasogastric tube and call a surgeon DR. JCDT DR. JCDT C. NEC, I.V. fluids administration, place a nasogastric tube, antibiotics, and admit to the intensive care Our patient was delivered at full term, but if he was delivered prematurely with very similar symptoms of D. Toxic megacolon, I.V. fluids administration, place a crying inconsolably, blood in his stool, lethargy, and nasogastric tube, and admit to the intensive 33 34 vomiting and had the above x-ray, what is your most care unit. likely diagnosis and treatment? Correct answer: NEC is a disease that, while it is classically a disease A. Pyloric stenosis, order an ultrasound and call a of premature neonates diagnosed in the neonatal surgeon intensive care unit, it may occasionally occur in the term neonate after discharge from the newborn B. Malrotation with midgut volvulus, place a nursery. nasogastric tube and call a surgeon DR. JCDT DR. JCDT Symptoms include vomiting, feeding intolerance, C. NEC, I.V. fluids administration, place a nasogastric and inconsolable crying, and the management tube, antibiotics, and admit to the intensive would be similar and also include stabilization with care **** I.V. fluids administration and nasogastric tube placement. D. Toxic megacolon, I.V. fluids administration, place a 35 36 nasogastric tube, and admit to the intensive care unit 6
- 7. 03/03/2013 As soon as the diagnosis of malrotation with midgut volvulus is seriously entertained, as it was in our patient, a pediatric surgeon should be contacted to discuss management and to expedite both confirmatory studies and definitive care. This condition is a true surgical emergency, with a DR. JCDT DR. JCDT mortality of approximately 15% and, when surgery is delayed, there is significant morbidity associated with An abdominal x-ray like the one above necessary resection of ischemic bowel as seen by the demonstrates pneumatosis intestinalis or portal dark dusky bowel pictured. air that is pathognomonic of NEC. Administration of broad-spectrum antibiotics, pediatric surgical 37 38 consultation, and critical care management is required. Treatment of malrotation with midgut volvulus is a Recent studies have shown that laparoscopic surgical Ladd's procedure through a transverse derotation and Ladd's procedure proved effective in supraumbilical incision. In this procedure, initially the 75% of cases, with a conversion to an open bowel is untwisted in a counterclockwise fashion. procedure in 25% of cases with similar rates of complications of recurrent malrotation and/or DR. JCDT DR. JCDT The Ladd's bands, which are peritoneal attachments volvulus (19%) and significantly shorter times to from the duodenum, right colon, and cecum, are starting feeds and postoperative length of stay. divided to prevent further twisting. 39 40 Postoperative complications include recurrent volvulus (2%-6%), short bowel syndrome, adhesions causing small bowel obstruction, postoperative intussusception, and the need for total parenteral nutrition. DR. JCDT DR. JCDT Mortality rates have been reported between 2%-24% In our case, the patient was found to have necrosis of depending on the amount of bowel necrosis and the the entire midgut similar to the image above. Given age of the patient. Less than 10% of necrosis at the the dismal chance of survival, after discussion with the time of surgery carries nearly a 100% survival rate, family, palliative care was initiated and the child died while 75% necrosis has only a 35% survival rate. peacefully. This case underscores the importance of 41 diagnosis and treatment in a timely fashion. 42 7
- 8. 03/03/2013 Gracias por su atención DR. JCDT Dr. Juan Carlos Díaz Torre Pediatra Neonatólogo dr_diaz_torre@hotmail.com (779) 100 - 40 - 26 43 8
